Azithromycin Antibiotic May Help PANS
PANS is a neuropsychiatric syndrome characterized by the acute onset of obsessive compulsive and other abnormal behaviors, tics, and mood changes that appear in a child following a bacterial or viral infection. PANS refers to any pediatric acute-onset neuropsychiatric syndrome of this type, while PANDAS refers more specifically to such a syndrome that occurs after exposure to streptococcal infections.
New research suggests that treatment with the antibiotic azithromycin can treat PANS. In a study presented at the 2016 meeting of the Society of Biological Psychiatry, Tanya K. Murphy and colleagues found that among 32 children aged 4–14 who showed obsessive compulsive symptoms following an infection, those who were given a 4-week course of azithromycin (10mg/kg of body weight, up to 500 mg/day) saw a 26% drop in symptoms, compared to a 1% drop in symptoms in those who received placebo instead.
At the end of the four weeks, 38.9% of the azithromycin group were classified as much improved or very much improved, while no one in the placebo group achieved this level of improvement. Azithromycin treatment increased the QTc interval (a measure of heart rate) and pulse in the study participants, but did not have any other notable side effects.
PANS is thought to arise from an immune response to infection that goes awry and begins attacking neurons in the brain, particularly in the thalamus. For a more complete review of PANS, see several of our earlier articles about PANS and an excellent review article by researcher Kiki Chang and colleagues in the Journal of Child and Adolescent Psychopharmacology in 2015.
It is important to work up a child suspected of having PANS, as the syndrome does not usually respond to conventional psychiatric treatment and often requires anti-inflammatory drugs (steroids or immunosuppressants), intravenous immunoglobulin (IVIG), plasma exchange, the TNF alpha blocker infliximab, or antibiotics.
Antibiotic Minocycline Could Improve Bipolar Depression
In an abstract presented at the 2013 meeting of the Society of Biological Psychiatry, Iosifescu et al. reported that the antibiotic minocycline, which has showed anti-inflammatory, neuroprotective, and mitochondrial-sparing effects in animal models, brought about improvement in patients with bipolar depression. Doses of 100mg to 300mg per day were successful in this small open study.
There are some positive placebo-controlled data in patients with schizophrenia who were prescribed this antibiotic. However, until now it had not been studied in bipolar disorder. The preliminary data reported here suggest that controlled double-blind studies of this agent are needed in bipolar depression.
The abstract (#497) can be found in the 2013 convention supplement (9S) to the journal Biological Psychiatry.
The N-acetylcysteine Story: A New Potential Therapy for Bipolar Illness and Substance Abuse
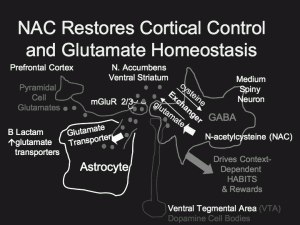
N-acetylcysteine (NAC), a readily available substance from health food stores, is able to reestablish glutamate homeostasis (regulation and balance) in the reward area of brain (the nucleus accumbens), reported Peter Kalivas of the University of South Carolina at the “Staging neuropsychiatric disorders: Implications for idiopathogenesis and treatment” meeting in Mojacar, Spain this past November. Kalivas reported that NAC appears to be effective across a spectrum of addictions, including cocaine, heroin, alcohol, cigarette smoking, and gambling.
Even more remarkably, NAC also appears to have positive effects in placebo-controlled studies in the treatment of patients with bipolar illness, report Mike Berk and colleagues, who are studying the same substance in Australia. Compared with placebo, patients taking adjunctive NAC showed improvement in all outcome measures, especially depression, after 3 and 6 months. In another article, also published in Biological Psychiatry in 2008, Berk’s research group demonstrated that NAC improved some negative symptoms of schizophrenia. NAC has also shown positive effects in trichotillomania and on nail-biting, suggesting that it has a variety of potential clinical uses in conditions associated with pathological compulsive behavioral patterns.