Bipolar I patient show dramatic reductions in white matter integrity
Thiel et al in Neuropsychopharmacology (2024) reported that “Compared with HC [healthy controls], BD-I patients exhibited lower FA [fractional anisotropy] in widespread clusters (ptfce-FWE?< 0.001), including almost all major projection, association, and commissural fiber tracts. BD-II patients also demonstrated lower FA compared with HC, although less pronounced (ptfce-FWE?=?0.049).”
Editors Note: These data once more emphasize the importance of using lithium (Li) in bipolar disorder as it can ameliorate the deficits in white matter integrity that are so prominent in the illness. Li also improve the loss of cortical grey matter volume that evolves with illness progression. Li prevents episodes of depression and mania and reduces the incidence of suicides. That Li can reverse or ameliorate brain abnormalities in bipolar disorder is one more piece of evidence that Li should be considered a disease modifying drug (DMD) and started early in the course of illness in almost all bipolar patients. The new mantra for patients and clinicians is: Use more lithium and prevent illness progression.
NEW FINDINGS BY COLVIN AWARD WINNER ROGER MCINTYRE
There is a convergence of finding of the occurrence of cognitive dysfunction in diabetes, obesity, and bipolar and unipolar mood disorders. This is based on new evidence of insulin resistance in the CNS found in examination of exosomes. Insulin is neuroprotective and neurotrophic much like lithium. People on lithium do not have evidence of loss of grey and white matter that other’s with bipolar disorder who are not on lithium have. Intra-nasal insulin can improve cognition. The widely used insulin sensitizers GLP-1s for diabetes and weight loss appear to also decrease cognitive decline. The GLP-1 liraglutide improves cognition in mood disordered patients, and increases brain NAA in obesity. The GLP-1 semaglutide appears to increase motivation, cognition and overcome reward deficits. These agents could have anti-depressant and depression preventing properties which remain to be further confirmed in ongoing clinical trials.
McIntyre finds that 80% of Alzheimer’s patients are insulin resistant and the GLP-1s are being studied for this illness as well. There is also a convergence of deficits in cognition, motivation, normal mood in Alzheimer’s patients.
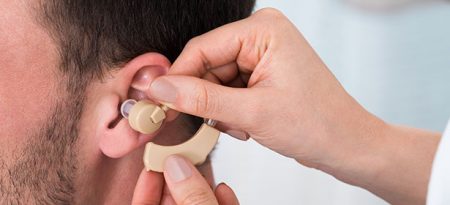
Hearing Aids May Lessen Cognitive Decline, Memory Loss
A 2018 article by researcher Asri Maharani and colleagues in the Journal of the American Geriatrics Society reports that using a hearing aid was associated with better scores on a test of episodic memory, and that declines in episodic memory slowed after participants began using hearing aids.
The study included 2,040 adults aged 50 years and up. Maharani and colleagues used data from the Health and Retirement Study, which measured participants’ cognitive functioning every two years for 18 years. Participants were asked to recall 10 words both immediately and after some delay.
The authors suggested that improving access to hearing aids earlier in the course of hearing impairment might help to stem the rise of dementia.
Bipolar Disorder and Diabetes Linked
 A systematic literature review in 2016 showed a definitive link between bipolar disorder and diabetes. Bipolar disorder almost doubles the risk of diabetes while diabetes more than triples the risk of bipolar disorder. The article by Ellen F. Charles and colleagues was published in the International Journal of Bipolar Disorders.
A systematic literature review in 2016 showed a definitive link between bipolar disorder and diabetes. Bipolar disorder almost doubles the risk of diabetes while diabetes more than triples the risk of bipolar disorder. The article by Ellen F. Charles and colleagues was published in the International Journal of Bipolar Disorders.
The review included seven large cohort studies. The studies, based on elderly populations only, examined bipolar disorder and diabetes rates. Charles and colleagues suggested that shared mechanisms could cause both illnesses. New disease models that explain the link between bipolar disorder and diabetes could lead to better treatments.
The review also reported that both bipolar disorder and diabetes were independently associated with risk of cognitive decline and dementia in these elderly individuals. People with diabetes had more brain atrophy on average than others who share their age and gender but did not have diabetes. People with bipolar disorder who also had diabetes and either insulin resistance or glucose intolerance had neurochemical changes in the prefrontal cortex that indicated poor neuronal health. In some cases, these patients also had reduced brain volume in the hippocampus and cortex.
Inactivity in Young Adulthood May Worsen Cognition Later in Life
The couch potato lifestyle common in the US may have consequences later, in the form of deficits in memory, executive functioning (including planning and execution) and processing speed.
At the 2015 Alzheimer’s Association International Conference, researcher Kristine Yaffe and colleagues reported that low levels of physical activity and high rates of television viewing in young adulthood may reduce cognitive capabilities in midlife.
The Centers for Disease Control report that less than 50% of adults aged 18–64 get the recommended minimum of physical activity each week. The guidelines recommend at least 150 minutes of moderate intensity aerobic activity (such as walking briskly) and two or more days of muscle-strengthening activities that work all major muscle groups.
Yaffe says that physical activity can protect against cognitive decline or dementia later on.
Participants in the long-term study who reported burning fewer than 300 calories per 50-minute session three times per week during two-thirds of their followup visits had worse cognition at year 25 than those participants who were more active. Those who watched more than four hours of television per day also had reduced cognition in midlife.
Yaffe stresses that exercising regularly is not just important in keeping weight down and protecting the heart, but also in protecting the brain. Regular physical activity may even prevent illnesses such as Alzheimer’s disease.
Low Vitamin D Linked to Cognitive Decline
Low levels of vitamin D levels are common, particularly in older adults and in African Americans and Hispanics. Unfortunately, low vitamin D is associated with decline in two types of cognitive functioning: episodic memory (memories of autobiographical events) and executive function (reasoning, problem-solving, planning, etc.).
A recent study with a particularly diverse group of participants, over half of whom were African American or Hispanic, found that over a period of about 5 years, episodic memory and executive function declined faster in older adults with low levels of vitamin D.
Average vitamin D levels for the entire group of 382 adults were below national standards. Levels of 25-hydroxy vitamin D should be between 20 and 50 nanograms per milliliter of blood. The average fell just below this, at 19.2 ng/mL. Over a quarter of participants had vitamin D deficiency, with levels below 12 ng/mL, and another 35.1% had vitamin D insufficiency, with levels between 12 and 20 ng/mL.
African Americans and Hispanics had lower levels of vitamin D (17.9 ng/mL and 17.2 ng/mL, respectively) than whites (21.7 ng/mL). Average vitamin D levels were lower in participants with dementia compared with those who had mild cognitive impairment or normal cognitive function.
Vitamin D levels can depend on factors such as dairy intake, sun exposure, and exercise. It has not been determined whether taking vitamin D supplements could slow down cognitive decline, but vitamin D supplementation has several benefits. Compared to placebo, supplementation with vitamin D increases response to antidepressants. A high percentage of children with major psychiatric disorders are vitamin D deficient, and it is also estimated that about 40% of adults in the US have a vitamin D deficiency.
The study by researcher Joshua W. Miller and colleagues was published in the journal JAMA Neurology in September.