Harsh Physical Punishment is Associated with Mood and Other Disorders
Physical punishment of children has long been a controversial subject. A 2012 article by Afifi et al. in the journal Pediatrics suggests that having experienced harsh physical punishment during childhood is associated with mood disorders, anxiety disorders, substance abuse and dependence, and personality disorders in adulthood.
In this study harsh physical punishment included pushing, grabbing, shoving, slapping, or hitting. Participants who had experienced more severe maltreatment in childhood (including physical abuse, sexual abuse, emotional abuse, physical neglect, emotional neglect, and exposure to violence between intimate partners) were excluded from the study, and the results were adjusted for sociodemographic variables and family history of dysfunction, suggesting that physical punishment was the mediator of these effects.
Women with Bipolar Disorder at Higher Risk for Postpartum Depression
 The risk of having a depressive episode during pregnancy compared to afterward have not often been studied. A 2011 review article by Viguera et al. in the American Journal of Psychiatry compared rates of affective episodes among women with bipolar I and II disorders and recurrent major depressive disorder, both during pregnancy and the postpartum period. Risks were higher for women with bipolar disorder.
The risk of having a depressive episode during pregnancy compared to afterward have not often been studied. A 2011 review article by Viguera et al. in the American Journal of Psychiatry compared rates of affective episodes among women with bipolar I and II disorders and recurrent major depressive disorder, both during pregnancy and the postpartum period. Risks were higher for women with bipolar disorder.
Among women with bipolar disorder, 23% experienced mood episodes during the pregnancy, while 52% had an episode in the months after giving birth. Among women with unipolar depression, 4.6% had a mood episode during pregnancy, while 30% did during the postpartum period, which is about double the risk seen in the general population. Depression was the most common type of morbidity the women experienced before and after giving birth.
Risk factors associated with mood episodes during pregnancy included (in descending order): younger age at illness onset, previous postpartum episodes, fewer years of illness, bipolar disorder, fewer children, and not being married. Risk factors associated with postpartum episodes included: younger age at illness onset, illness during pregnancy, bipolar disorder, fewer children, and more education.
Editor’s Note: The risk of postpartum depression increases from 15% in the general population, to 30% among women with unipolar disorder, to 50% in women with bipolar disorder. Special precautions should be taken to monitor and treat depression during and after pregnancy, in all women but particularly in those with a prior history of unipolar or bipolar disorder.
Obesity and Bipolar Disorder: News from the American Academy of Child and Adolescent Psychiatry
 At the annual meeting of the American Academy of Child and Adolescent Psychiatry in Toronto in October 2011, a symposium on the impact of obesity on the course of childhood onset bipolar illness was held.
At the annual meeting of the American Academy of Child and Adolescent Psychiatry in Toronto in October 2011, a symposium on the impact of obesity on the course of childhood onset bipolar illness was held.
Typical Treatment of Bipolar Disorder in Youth
David Axelson described the typical outcome of bipolar illness and the medications used during naturalistic treatment. The data came from the large collaborative Course and Outcome of Bipolar Illness among Youth (COBY) study, in which he and his colleagues followed 255 patients with bipolar I disorder (BP I), 30 patients with bipolar II (BP II), and 153 patients with bipolar not otherwise specified (BP NOS) for a mean of 5 years. He discussed only BP I children at the symposium.
The study initially followed 270 BP I children for a mean of 582 weeks. They ranged in age from 7 to 17 years (average 14.4 years). Ninety-three percent of the children were treated with one or more antimanic (AM) agents. These included atypical antipsychotics (AA) in 77%, valproate or carbamazepine in 44%, and lithium in 47%. Antidepressants (ADs) were used in 46% of the children, stimulants in 43%, and benzodiazepines in 21%. Sixty percent had been on two classes of antimanic medications concurrently at some point.
A univariate analysis showed that older children received smaller amounts of antipsychotics and more anticonvulsants and lithium. Variables associated with better response, that is, a rating of either much or very much improved on the Clinical Global Impressions scale for bipolar disorder (CGI-BP), included older age and treatment with atypical antipsychotics. Those who had comorbid attention deficit hyperactivity disorder (ADHD) or psychosis at baseline did more poorly. Mean symptom scores were better when the children received any anti-manic treatment including an atypical or lithium, but worse when they received valproate or carbamazepine.
These data are similar to those from other prospective treatment outcome studies in childhood-onset bipolar I illness. Taken together they all suggest that the illness is difficult to treat and stabilize even when multiple medicines are used in combination.
Obesity and Mood Disorders in Youth
Another speaker, Ben Goldstein, indicated that in the scientific literature, obesity has been associated with a higher number of depressive episodes and longer length of depression, more recurrences of depression, more anxiety disorders, increased numbers of hospitalization, more suicide attempts, and worse functional outcomes. In the same group of patients discussed by Axelson above, 42% were overweight or obese, compared to a 34% incidence in the general population of children in this age range.
Factors associated with overweight included substance abuse, a history of physical abuse, prior hospitalization, and being on 2 or more medications. Those who were overweight or obese spent more time ill in a manic or depressive episode. Read more
Inflammation and Mood Disorders
There is increasing evidence of a link between inflammation, brain function, and treatment resistance in the mood disorders. Obesity is also linked to inflammatory processes and thus may contribute to the development of treatment resistance in both unipolar and bipolar mood disorders.
Causes of Inflammation
 Obesity is one factor that can lead to increases in inflammation. When people gain weight, the size of fat cells can increase to the point that the cells are deprived of oxygen and disintegrate. Then macrophages and other cells come in to sweep up the remaining particles of the fat cells. These scavenger cells then become activated and produce more regulatory chemicals called cytokines. The cytokines produced in the periphery (in the body outside the brain) can then enter the brain and affect brain function in a process that may ultimately be linked to fatigue, depression, and other adverse mood and behavior states that contribute to treatment resistance. There is a two-way street: the brain can influence the body and what goes on in the body can influence the brain.
Obesity is one factor that can lead to increases in inflammation. When people gain weight, the size of fat cells can increase to the point that the cells are deprived of oxygen and disintegrate. Then macrophages and other cells come in to sweep up the remaining particles of the fat cells. These scavenger cells then become activated and produce more regulatory chemicals called cytokines. The cytokines produced in the periphery (in the body outside the brain) can then enter the brain and affect brain function in a process that may ultimately be linked to fatigue, depression, and other adverse mood and behavior states that contribute to treatment resistance. There is a two-way street: the brain can influence the body and what goes on in the body can influence the brain.
Other factors that can lead to increases in inflammation and eventually to treatment resistance in the unipolar and bipolar mood disorders include early life stress, medical illness, and anxiety and personality disorders.
Anti-Inflammatory Treatments
Given the close links between inflammation and depression (discussed in BNN Volume 15, Issue 1 from 2011), Andrew H. Miller of Emory University decided to test a specific anti-inflammatory agent called infliximab (a TNF monoclonal antibody that inhibits TNF alpha actions) as an antidepressant. One sign of inflammation is a C-reactive protein (CRP) level of 2mg/L or greater. The effect of infliximab on the population of treatment refractory depressed patients who participated in Miller’s study was not significant on the whole, but the drug did have significantly greater antidepressant effects than placebo in those patients with the highest levels of CRP. The investigators believe this demonstrates the principle that a drug that inhibits TNF alpha may be useful in patients with the greatest degree of inflammation.
Other approaches to anti-inflammatory mechanisms are also being pursued, including use of aspirin, COX-2 inhibitors, and the antibiotic minocycline. Minocycline has anti-inflammatory and neuroprotective effects and has been reported to have positive effects in cognition and negative symptoms of schizophrenia.
Screening Tool for Depression and Anxiety Available via iPhone
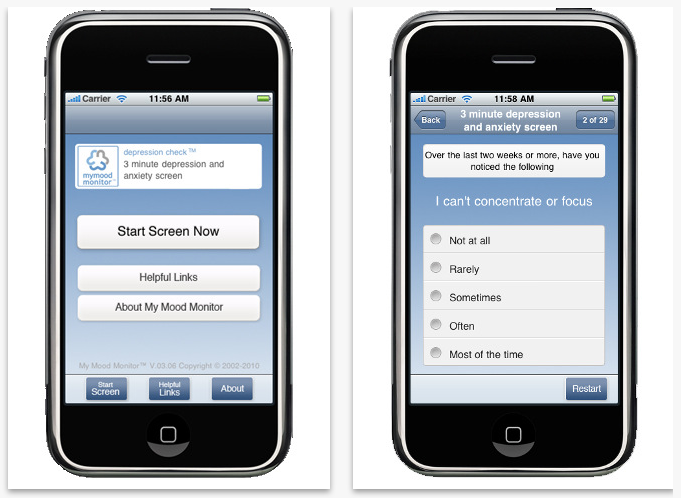
My Mood Monitor, a website for mental health screening, has introduced depressioncheck, a free, mobile version of their M-3 Checklist, a scientifically validated screening tool for mood and anxiety disorders that can now be used via Apple’s iPhone and iPod Touch. It can be found in the Itunes App Store.
Adapted from the online version, the mobile version provides a short series of questions that measure indicators of mental health. Developed by a team of mental health practitioners and experts, the checklist takes only three minutes to complete. It is ideal to fill out in the waiting room prior to an appointment with a general practitioner so the doctor can be made aware of potential problems in the area of mental health. Depressioncheck is appropriate for those 18 years and older and its accuracy was confirmed in an article published in the Annals of Family Medicine in March 2010.
We recommend My Mood Monitor and the new mobile application as simple and reliable screening tools that can assess the presence of unipolar and bipolar mood and anxiety disorders, including obsessive-compulsive disorder, panic disorder, and PTSD. Read more