FDA Warns of Potentially Lethal Reaction to Seizure Meds
Megan Brooks reports:
“The antiseizure drugs levetiracetam (Keppra, Keppra XR, Elepsia XR, Spritam, generic) and clobazam (Onfi, Sympazan, generic) can cause a rare but serious drug hypersensitivity reaction that can be life threatening if not detected and treated promptly, the US Food and Drug Administration (FDA) warns in an alert issued today.
Known as drug reaction with eosinophilia and systemic symptoms (DRESS), it may start as a rash but can quickly progress and cause injury to internal organs, the need for hospitalization, and death, the FDA notes.
Three cases occurred in the US, and 29 occurred abroad. In all 32 cases, the patients were hospitalized and received medical treatment; in two cases, the patients died.
The median time to onset of DRESS in the levetiracetam cases was 24 days; times ranged from 7 to 170 days. The reported signs and symptoms included skin rash (n = 22), fever (n = 20), eosinophilia (n = 17), lymph node swelling (n = 9), and atypical lymphocytes (n = 4). The median time to onset of DRESS in the levetiracetam cases was 24 days; times ranged from 7 to 170 days. The reported signs and symptoms included skin rash (n = 22), fever (n = 20), eosinophilia (n = 17), lymph node swelling (n = 9), and atypical lymphocytes (n = 4)…. DRESS symptoms resolved when levetiracetam was discontinued.”
Continuing Lithium Treatment Does Not Increase Kidney Failure
 A risk of long-term lithium treatment is that it can cause kidney damage. However, a new study suggests that continuing lithium treatment after a diagnosis of chronic kidney disease does not necessarily increase the risk of irreversible end-stage kidney disease, which is defined as either the need for either chronic dialysis or a kidney transplant.
A risk of long-term lithium treatment is that it can cause kidney damage. However, a new study suggests that continuing lithium treatment after a diagnosis of chronic kidney disease does not necessarily increase the risk of irreversible end-stage kidney disease, which is defined as either the need for either chronic dialysis or a kidney transplant.
The 2017 study by researcher Lars Kessing and colleagues in the journal Acta Psychiatrica Scandinavica used Danish health databases to track data from all individuals who received a diagnosis of chronic kidney disease between 1995 and 2012 and also had a history of lithium treatment (754 patients) or anticonvulsant treatment (5,004 patients). Kessing and colleagues found that patients who continued taking lithium after an initial diagnosis of chronic kidney disease had decreased rates of end-stage kidney disease. This also held true for those who continued anticonvulsant treatment after a diagnosis of kidney disease.
One point of uncertainty was introduced by the finding that the subset of participants who were taking lithium specifically to treat bipolar disorder did have a higher rate of end-stage kidney disease. This was not true of the participants who were taking anticonvulsants to treat bipolar disorder.
Kessing and colleagues concluded that after an initial diagnosis of chronic kidney disease, continuing lithium did not necessarily increase end-stage kidney disease. Switching to an anticonvulsant, as is sometimes the practice after a kidney disease diagnosis, may not confer any benefit.
Taking SSRI Antidepressants May Increase Stroke Risk
 A Taiwanese study published in the Journal of Clinical Psychiatry in 2017 finds that taking selective serotonin reuptake inhibitor (SSRI) antidepressants can increase risk of stroke. The study by Chin-Hong Chan and colleagues analyzed eight years of data from Taiwan’s National Health Insurance Research Database, comparing people who had taken SSRIs for at least two consecutive months to those who had not. First onset strokes were more common among people who had taken SSRIs, and the higher stroke rates in this group persisted for three years after exposure.
A Taiwanese study published in the Journal of Clinical Psychiatry in 2017 finds that taking selective serotonin reuptake inhibitor (SSRI) antidepressants can increase risk of stroke. The study by Chin-Hong Chan and colleagues analyzed eight years of data from Taiwan’s National Health Insurance Research Database, comparing people who had taken SSRIs for at least two consecutive months to those who had not. First onset strokes were more common among people who had taken SSRIs, and the higher stroke rates in this group persisted for three years after exposure.
Ischemic strokes (which occur when a blood vessel carrying blood to the brain is obstructed) were more common than hemorrhagic strokes (which occur when a weak blood vessel ruptures). Younger adult participants exposed to SSRIs were more likely to have strokes, while people older than 65 saw only a slight increase in stroke risk from taking SSRIs. More strokes occurred during the first three years of SSRI treatment than later in treatment.
Chan and colleagues suggest that these strokes are caused by cerebral microbleeding or by overcorrection of hemostasis, the process by which the body slows or stops bleeding by constricting blood vessels and coagulating blood.
Making Lithium Treatment More Tolerable For Patients
 In a slideshow at Psychiatric Times, Chris Aiken describes seven ways to improve lithium’s tolerability. Since many researchers, including BNN Editor-in-Chief Robert M. Post, have suggested that lithium should be used more often as a treatment for bipolar disorder, ways of making its side effects more manageable are of great interest. Here we summarize Dr. Aiken’s seven points and add a few perspectives of our own.
In a slideshow at Psychiatric Times, Chris Aiken describes seven ways to improve lithium’s tolerability. Since many researchers, including BNN Editor-in-Chief Robert M. Post, have suggested that lithium should be used more often as a treatment for bipolar disorder, ways of making its side effects more manageable are of great interest. Here we summarize Dr. Aiken’s seven points and add a few perspectives of our own.
Aiken writes that “when it comes to the side effects that matter most to patients—sedation, weight gain, and cognition—lithium’s tolerability ranks right behind lamotrigine.” In fact, lithium plus lamotrigine is an excellent combination, as lithium excels at preventing manias while lamotrigine excels at depression prevention.
Post’s philosophy is that many of lithium’s side effects can be avoided in the first place through judicious dose titration. He suggests gradually increasing dosage, and stopping before side effects become difficult, or reducing a dosage that has already become a problem. The idea is to avoid lithium side effects even if blood levels of lithium remain below clinically therapeutic levels. Post suggests using lithium at whatever dose is not associated with side effects.
Many of lithium’s positive therapeutic effects emerge at low doses, and if this improvement is insufficient, the rest of the needed efficacy can be achieved by adding other medications. As noted above, lamotrigine is a good option for break-through depression, as is lurasidone. For breakthrough mania, the mood stabilizers valproate and carbamazepine or an atypical antipsychotic can be added to lithium.
A little-appreciated option for enhancing lithium’s mood stabilizing effects is nimodipine, a dihydropyridine calcium blocker. It has both antimanic and antidepressant efficacy without lithium’s side effects. Research showed that a year on the combination of lithium and nimodipine was more effective than a year of either drug alone.
If a patient taking lithium experiences a tremor at a dose that is not fully effective, nimodipine can be added in order to lower the lithium dose enough to eliminate the tremor.
Nimodipine specifically blocks the calcium influx gene CACNA1C that has been repeatedly been associated with the vulnerability to bipolar disorder and depression.
If side effects do occur on lithium, they can often be managed. The following suggestions are adapted from Aiken’s article with input from Post. Read more
The New News About Lithium
Robert M. Post, Editor-in-Chief of the BNN, recently published an open access article in the journal Neuropsychopharmacology, “The New News About Lithium: An Underutilized Treatment in the United States.” Here we summarize the main points of the publication, including: the multiple benefits of lithium, its relative safety, predictors of lithium responsiveness, and principles for treatment.
Benefits of lithium
Lithium prevents both depressions and manias in bipolar disorder, and also prevents depressions in unipolar disorder and can augment antidepressant effects acutely. In addition to these mood benefits, lithium has anti-suicide effects. Lithium also enhances the efficacy of atypical antipsychotics and other mood stabilizers when used in combination with them.
Lithium is good for the brain. It has been shown to reduce the incidence of dementia. Lithium increases the volume of the hippocampus and cortex, and can increase the production of new neurons and glia. It also protects neurons. In animals, lithium has been shown to reduce lesion size in neurological syndromes that are models for human disorders such as AIDS-related neurotoxicity, ischemic/hemorrhagic stroke, traumatic brain/spinal cord injury, Huntington’s disease, Alzheimer’s disease, amyotrophic lateral sclerosis (ALS or Lou Gehrig’s disease), fragile X syndrome, Parkinson’s disease, retinal degeneration, multiple sclerosis, alcohol-induced degeneration, Down’s syndrome, spinocerebellar ataxia-1, and irradiation.
Lithium’s benefits include more general ones as well. It can increase the length of telomeres, bits of DNA on the ends of chromosomes that protect them during replication. Short telomeres have been linked to various illnesses and the aging process. Lithium also decreases the incidence of several medical illnesses and enhances survival.
Side Effects Are Often Benign, Treatable
Lithium side effects are more benign than many people think. Even low levels of lithium may be therapeutically sufficient. Read more
Some Antacids Cause Kidney Damage with No Prior Symptoms
 Commonly used antacids such as Prevacid, Nexium, Prilosec, and Protonix can impair kidney function, according to a 2017 article in the journal Kidney International. These drugs, known as proton pump inhibitors or PPIs, should not be taken long-term without monitoring of kidney function. Other antacids that work by blocking histamine H2 receptors do not interfere with kidney function but may not work as well as PPIs.
Commonly used antacids such as Prevacid, Nexium, Prilosec, and Protonix can impair kidney function, according to a 2017 article in the journal Kidney International. These drugs, known as proton pump inhibitors or PPIs, should not be taken long-term without monitoring of kidney function. Other antacids that work by blocking histamine H2 receptors do not interfere with kidney function but may not work as well as PPIs.
Researcher Yan Xie and colleagues found that more than half of people who developed chronic kidney damage while taking PPIs showed no earlier acute signs of kidney dysfunction, meaning there may not be signs of kidney function loss until the damage is irreversible. Xie and colleagues suggest that patients and doctors should be more vigilant about monitoring the use of these medications, since waiting for outward signs of declining kidney function is not a reliable way of detecting damage.
More than 15 million Americans use prescription PPIs to reduce gastric acid, bringing relief to heartburn, ulcers, and acid reflux. Millions more buy PPIs over the counter without consulting a doctor about their use.
The study analyzed Department of Veterans Affairs data from 125,596 new users of PPIs and 18,436 new users of H2 blockers. Acute, reversible symptoms of kidney damage, such as reduction in the urine being cleared from the body, fatigue, and swelling of the legs and ankles were seen in less than 20% of the PPI users. However, more than half of those who developed chronic kidney damage and end-stage renal disease never showed these warning signals beforehand. In contrast, only 7.67% of those taking H2 blockers had chronic kidney disease without acute symptoms, and 1.27% had end-stage renal disease, when kidneys can no longer clear waste from the body, and dialysis or a kidney transplant is required.
Xie and colleagues suggest carefully monitoring kidney function in people taking PPIs, even when there are no outward signs of problems. They also suggest carefully evaluating whether PPIs are necessary, since the risk of kidney damage is serious.
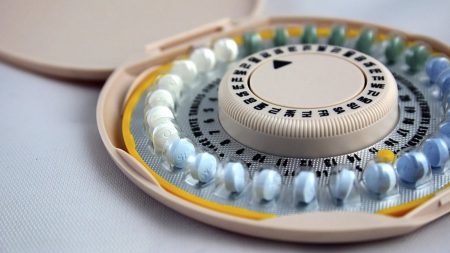
Use of Hormonal Contraceptives May Increase Depression Risk in Young Women
Women, particularly adolescent women, are at increased risk of developing depression if they use hormonal contraceptives, according to a 2016 study in the journal JAMA Psychiatry. The study by Charlotte Wessel Skovlund and colleagues used data from a Danish registry of more than one million women between the ages of 15 and 34 who had no history of depression or other psychiatric disorders. During follow-up (which lasted an average of 6.4 years), 55% of the women were using or had recently used hormonal contraceptives. These women were more likely to be prescribed an antidepressant for the first time, and more likely to be diagnosed with depression compared to women who did not use hormonal contraceptives.
The increased risk of being prescribed an antidepressant varied by contraceptive type. The norgestrolmin patch increased risk by 2.0 times, and the etonogestrel vaginal ring did so by 1.6 times. The levonorgestrel intrauterine device (IUD) made an antidepressant prescription 1.4 times more likely. Progestin-only pills increased risk by 1.34 times and combined oral contraceptive pills increased it by 1.23 times compared to women who did not use oral contraceptives.
The relative risk peaked at around six months after starting hormonal contraceptives.
Patients aged 15–19 were particularly vulnerable to depression. The likelihood of receiving an antidepressant prescription was 1.8 times higher in teens taking combined pills, 2.2 times higher in those taking progestin-only pills, and 3 times higher in teens using hormonal methods of birth control that are not delivered orally compared to those who did not use hormonal contraceptives at all.
Birth Defects from Valproate Lower in Bipolar Disorder than in Epilepsy
 The anticonvulsant valproate increases the risk of serious birth defects in fetuses exposed to it. However, a 2017 report by ANSM, France’s agency for health and product safety, and its national insurance fund for employed workers shows that these risks are lower for women taking valproate for bipolar disorder than for women taking valproate for epilepsy.
The anticonvulsant valproate increases the risk of serious birth defects in fetuses exposed to it. However, a 2017 report by ANSM, France’s agency for health and product safety, and its national insurance fund for employed workers shows that these risks are lower for women taking valproate for bipolar disorder than for women taking valproate for epilepsy.
In France, the risk of a major fetal malformation was 10.2 per 1000 women in the general population, about twice that (22.2 per 1000) in women taking valproate for bipolar disorder, and about 4 times higher (46.5 per 1000) in women taking valproate for epilepsy. The authors suggest that treatment for bipolar disorder may be more likely to be interrupted during pregnancy, and this could explain the different levels of risk by diagnosis.
Among the risks of defects in the fetuses of women being treated with valproate for epilepsy, the risk of a ventricular septal defect (a hole in the wall separating the lower heart chambers) was 11.2% compared to 2.7% in fetuses not exposed to valproate, while risk of an atrial septal defect (a hole in the wall separating the upper heart chambers) was 19.1% in the fetuses of those prescribed valproate for epilepsy compared to 1.9% in unexposed fetuses. Risk of hypospadias (placement of the urethra opening on the underside of the penis rather than its end) was 22.7% compared to 4.8% in the general population.
Risks of a major malformation were dose dependent in those with epilepsy (but interestingly, not in those with bipolar disorder), meaning the more valproate patients with epilepsy took, the higher their risk of a fetus with birth defects.
The only birth defects that were more common in the fetuses of women taking valproate for bipolar disorder than in fetuses not exposed to valproate were hypospadias (17.5% risk compared to 4.8% in the general population) and craniostenosis, a deformity of the skull (4.2% risk compared to 0.4% in the general population).
The relative safety of valproate in women being treated for bipolar disorder compared to those being treated for epilepsy is good news for some. However, fetal exposure to valproate has also been linked to deficits in cognitive development.
The risk of spina bifida, which causes lifetime paralysis, in a fetus may no longer be such a catastrophic issue for women taking valproate for bipolar disorder (where the risk did not exceed that of the general population), as was once assumed based on data from women with epilepsy (where the risk is usually 2-4%, but was 8% in this French study). This may be of some comfort to women with bipolar disorder who require valproate treatment to remain stable and wish to become pregnant or in those who experience an unplanned pregnancy.
Some Drugs for Hypertension Come with Greater Risk of Mood Disorders
 Depression and bipolar disorder have been linked to atherosclerosis, the accumulation of fats, cholesterol, and plaques on the walls of the arteries. There is some evidence that drugs to treat hypertension may contribute to mood disorders. A large study published in the journal Hypertension in 2016 suggests that certain classes of anti-hypertensive drugs, calcium antagonists and beta blockers, may increase risk of mood disorders compared to other treatments for hypertension.
Depression and bipolar disorder have been linked to atherosclerosis, the accumulation of fats, cholesterol, and plaques on the walls of the arteries. There is some evidence that drugs to treat hypertension may contribute to mood disorders. A large study published in the journal Hypertension in 2016 suggests that certain classes of anti-hypertensive drugs, calcium antagonists and beta blockers, may increase risk of mood disorders compared to other treatments for hypertension.
The study by researcher Angela H. Boal and colleagues used data from a hospital database to identify 144,066 patients between the ages of 40 and 80 who had taken anti-hypertensive drugs for more than 90 days. There was an independent linear connection between receiving a prescription for hypertenstion and being diagnosed with a mood disorder. Patients who took angiotensin-converting enzyme inhibitors or angiotensin receptor blocking drugs had the lowest rates of mood disorder admissions. Those taking calcium antagonists or beta blockers had an increased risk of a mood disorder, while those taking thiazide diuretics and those not taking anti-hypertensive drugs had no change in risk.
Preventing Metformin Side Effects
Depression is a risk factor for type 2 diabetes, and the drug metformin is a common treatment for diabetes. In a 2016 article in the Journal of Clinical Psychiatry, researcher Chittaranjan Andrade suggests ways of minimizing side effects from metformin.
Gastrointestinal side effects such as nausea, vomiting, abdominal discomfort, flatulence, and diarrhea are common on metformin. In the article, Andrade writes, “These are less likely to occur with gradual dose uptitration, administration of the drug with meals, and use of a time-release formulation.”
Lactic acidosis, a buildup of lactate in the body that can result in muscle pain, burning, and other symptoms, is a rare side effect of metformin. Avoiding prescribing metformin to people with impaired kidney, liver, or cardiac functioning and other risk factors can prevent lactic acidosis.
Vitamin B12 absorption can also be affected by long-term metformin use. Andrade suggests that rather than waiting for a vitamin deficiency to be identified, a proactive approach should be taken. Long-term metformin users could be given an annual intramuscular shot of vitamin B12.