Serotonin is Back
A review by Moncrieff et al in Molecular Psychiatry 2022 concluded that : “there is no convincing evidence that depression is associated with, or caused by, lower serotonin concentrations or activity.” This was widely reported in the news media.
A new analysis by 26 experts in the field finds many faults with this analysis (Jauhar et al 2023). Instead, they conclude “A more accurate, constructive conclusion would be that acute tryptophan depletion and decreased plasma tryptophan in depression indicate a role for 5-HT in those vulnerable to or suffering from depression, and that molecular imaging suggests the system is perturbed. The proven efficacy of SSRIs in a proportion of people with depression lends credibility to this position.” Long live serotonin’s role in depression.
Adolescent Delta-9-tetrahydrocannabinol induces long-term neuronal disturbances in dorsal vs. ventral hippocampus
De Felice et al reported in Neuropsychopharmacology (2022) how adolescent THC exposure in a rodent model can induce significant morphological disturbances and glutamatergic signaling abnormalities in the hippocampus. The dorsal hippocampus is critical for cognitive and contextual processing, whereas the ventral region is critical for affective and emotional processing. Adolescent THC exposure induces long-lasting memory deficits and anxiety like-behaviors concomitant with a wide range of differential molecular and neuronal abnormalities in dorsal vs. ventral hippocampal regions.
Editors Note: While these data are in rodents, they provide insights into how THC use in adolescents exerts memory deficits and anxiety-like behavior in adulthood by dysregulation of glutamate signaling in the hippocampus. These data converge with data in humans. The bottom line is: use of marijuana in adolescence is not good for brain function, cognition, and behavior in adulthood.
Review Describes Latest Findings on the Mechanisms of Psychedelic Drugs and Their Therapeutic Potential
In a 2021 review article in a special issue of the Journal of Neurochemistry devoted to “Psychedelics and Neurochemistry,” researcher Alaina M. Jaster and colleagues summarized recent findings on psychedelic drugs, including their potential as treatments for psychiatric disorders and the structural changes they produce in the brain. The review article focused on findings in humans and provided background context based on findings in animals, particularly rodents.
In the article, Jaster and colleagues write that psychedelics “have in common a battery of acute (within minutes to hours) effects in humans that include profound changes in processes related to perception, cognition, sensory processing, and mood.” They are not considered to be addictive, and recent research has identified fast-acting and long-lasting therapeutic effects of psychedelics, particularly for the treatment of depression and substance abuse.
While psychedelic drugs interact with the brain in complicated ways, the role of serotonin 5-HT2A receptors seems to be crucial to their effects. Psychedelics have classically been divided into two groups based on their chemical structures: phenethylamines (which include mescaline and its synthetic analog DOI) and tryptamines (which include psilocybin/“magic mushrooms,” DMT/ayahuasca, and ergolines like LSD, which are sometimes separated into a third category). The authors of the review highlight that other substances with different chemical structures that do not fit into this classification can also function as psychedelics. Examples include efavirenz and quipazine, which both activate serotonin 5-HT2A receptors and change rodent behavior in the same way that other psychedelic drugs do. These drugs are providing new directions for research into how psychedelics work at both serotonin 5-HT2A receptors and monoaminergic G protein-coupled receptors (GPCRs).

Rodent studies are often used to investigate how psychedelic drugs work. Rodent behaviors such as ear scratching and head twitching increase when the rodents are given drugs that have psychedelic effects in humans. These behaviors return to normal when rodents are given drugs that function as serotonin 5-HT2A receptor antagonists, preventing the stimulation of these serotonin receptors.
While it has been established that serotonin 5-HT2A receptors play an important role in the hallucinogenic effects of psychedelic drugs, how serotonin receptors are involved in some of the therapeutic effects of psychedelics, such as antidepressant effects and changes to synaptic plasticity, is not yet clear.
According to the review, “A number of studies in animal models as well as postmortem human brain samples from subjects with depression and controls has provided evidence that mood disorders occur in conjunction with a reduction in the density of dendritic spines, particularly in the frontal cortex.” Dendrites are the projections from the cell bodies of neurons upon which nerve endings from the axons of other neurons synapse. The surface of these dendrites is covered in mushroom-shaped spines that help create these synaptic connections. The review describes in vitro and in vivo research on mice that suggests that the psychedelics DOI, DMT, and LSD can remodel dendritic spines.
At a recent scientific meeting, researcher Javier González-Maeso, one of the authors of the review, described findings from a recent study of mice given DOI. The structure of the dendritic spines in the prefrontal cortex changed rapidly in these mice. They had also been conditioned to produce a fear response, and the extinction process to get rid of this learned fear was sped up in the mice given DOI. These effects occurred via the serotonin 5-HT2 receptors. The exposure to the psychedelic also affected the regulation of genes involved in synaptic assembly for days, suggesting that epigenetic-induced changes in synaptic plasticity may underlie some of the long-lasting therapeutic effects of psychedelics.
The review also addressed “microdosing,” the recreational practice of consuming small amounts of psychedelics such as psilocybin or LSD, based on the theory that amounts too small to create a hallucinogenic effect may instead produce therapeutic results. The authors find limited data to support microdosing. Most studies in humans and rodents have found no effect or, in the case of one rat study, a worsening of dendritic spine density following microdosing.
Endocannabinoid System May Help Explain Tourette Syndrome

Endocannabinoids are neurotransmitters produced by the human body that attach to cannabinoid receptors in the brain, the same receptors that are affected by the consumption of cannabis products.
Tourette syndrome, a neurodevelopmental disorder characterized by tics and psychological symptoms, is probably caused by some dysfunction involving the neurotransmitter dopamine. The syndrome is usually treated with dopamine receptor blockers but is also eased by cannabis use and treatment with THC, the main psychoactive component in cannabis. Recently, researchers set out to determine whether concentrations of endocannabinoids in the cerebrospinal system are related to Tourette syndrome.
In an article published in the journal Neuropsychopharmacology in 2020, researcher Kirsten R. Müller-Vahl and colleagues report that endocannabinoid concentrations were significantly higher in the cerebrospinal fluid of 20 people with Tourette’s syndrome than in 19 control participants without Tourette’s.
The researchers found elevations in the endocannabinoids AEA and 2-AG, the endocannabinoid-like ligand PEA, and the metabolite AA in the participants with Tourette’s syndrome. Levels of 2-AG in the cerebrospinal fluid correlated with severity of attention-deficit hyperactivity disorder symptoms, an aspect of the syndrome.
It is possible that higher concentrations of endocannabinoids are present in the syndrome because they compensate for the overactive influence of dopamine. This explanation would fit with the effectiveness of cannabis in treating Tourette’s. However, that has not yet been determined, and it is also possible that the endocannabinoids are a reaction to dysfunction involving other neurotransmitters, are incidental to the syndrome, or in the best case that they are a direct cause of the syndrome.
Müller-Vahl and colleagues suggest that based on the effectiveness of cannabis in treating Tourette’s, it may turn out that the syndrome is a sort of endocannabinoid deficiency. They believe this hypothesis is not counteracted by the high levels of cannabinoids they found in Tourette’s patients in this study, because these high levels may be accompanied by a reduced number or reduced sensitivity of the cannabinoid receptors or overactivity in the enzymes that break down endocannabinoids, such that it is difficult to maintain normal levels of these neurotransmitters.
Inflammation Predicts Lower Frontal and Temporal White Matter Volumes in Early-Stage Bipolar Disorder
 At the 2019 meeting of the International Society for Bipolar Disorders, researcher David Bond found that seven inflammatory cytokines predicted lower white matter volumes in the left frontal and bilateral temporal lobes, as well as in the cingulate and inferior frontal gyri. Cytokines are secreted by some immune cells and send signals that can produce an effect in other cells.
At the 2019 meeting of the International Society for Bipolar Disorders, researcher David Bond found that seven inflammatory cytokines predicted lower white matter volumes in the left frontal and bilateral temporal lobes, as well as in the cingulate and inferior frontal gyri. Cytokines are secreted by some immune cells and send signals that can produce an effect in other cells.
Bond noted that greater inflammation did not predict lower parietal or occipital white matter volumes, suggesting that inflammation had a greater effect on white matter volume in those parts of the brain most closely linked to mood disorders.
Scientific Mechanisms of Rapid-Acting Antidepressants
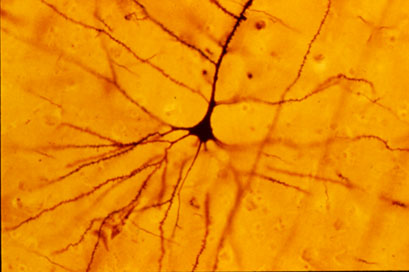
A pyramidal cell (Photo by Bob Jacobs, Laboratory of Quantitative Neuromorphology Department of Psychology Colorado College)
At a recent symposium, researcher Francis McMahon provided electrophysiological evidence that several different types of rapid-acting antidepressants—low-dose ketamine, scopolamine, and rapastinel (a partial agonist of the neurotransmitter NMDA)—act by decreasing the inhibitory effects of GABAergic interneurons on excitatory neurons called pyramidal cells, thus increasing synaptic firing.
Researcher Ronald Duman further dissected these effects, showing that ketamine and its active metabolite norketamine reduce the steady firing rate of GABA interneurons by blocking NMDA receptors, while the partial agonist rapastinel acts on the glutamate neurons directly, and both increase the effects of a type of glutamate receptors known as AMPA. These effects were demonstrated using a virus to selectively knock out GluN2B glutamate receptor subunits in either GABA interneurons or glutamate neurons.
Increasing AMPA activity increases synapse number and function and also increases network connectivity, which can reverse the effects of stress. Duman and colleagues further showed that when light is used to modulate pyramidal cells (a process called optogenetic stimulation) in the medial prefrontal cortex, different effects could be produced. Stimulating medial prefrontal cortex cells that contained dopamine D1 receptors, but not D2 receptors, produced rapid and sustained antidepressant effects. Conversely, inhibiting these neurons blocked the antidepressant effects of ketamine. Stimulating the terminals of these D1-containing neurons in the basolateral nucleus of the amygdala was sufficient to reproduce the antidepressant effects. These data suggest that stimulation of glutamate D1 pyramidal neurons from the medial prefrontal cortex to the basolateral nucleus of the amygdala is both necessary and sufficient to produce the antidepressant effects seen with ketamine treatment.
Researcher Hailan Hu reported that NMDA glutamate receptors drive the burst firing of lateral habenula (LHb) neurons, which make up the depressogenic or “anti-reward center” of the brain and appear to mediate anhedonic behavior (loss of interest or enjoyment) in animal models of depression. Ketamine blocks the burst firing of the LHb neurons, which disinhibits monoamine reward centers, enabling ketamine’s rapid-onset antidepressant effects. This may occur because inhibitory metabotropic glutamate receptors (mGluR-2) are activated, decreasing the release of glutamate.
MGluR-2 may also help explain the antidepressant effects of acetyl-L-carnitine supplements. L-carnitine is an amino acid that is low in the blood of depressed patients. The supplement acetyl-L-carnitine (ACL) activates the DNA promoter for mGluR-2, increasing its production and thus decreasing excess glutamate release. The acetyl group of the ACL binds to the DNA promoter for mGluR-2, thus this process seems to be epigenetic. Epigenetic mechanisms affect the structure of DNA and can be passed on to offspring even though they are not encoded in the DNA’s genetic sequence.
Inflammatory Marker CRP Higher in Bipolar Disorder, Particularly Mania
Inflammation has been linked to mood disorders. A 2016 meta-analysis in the journal Lancet Psychiatry described the role of inflammatory marker C-reactive protein (CRP) in bipolar episodes. Researchers led by Brisa S. Fernandes identified 27 studies that measured CRP levels in a total of 2,161 patients with bipolar disorder and 81,932 healthy participants. The researchers determined that compared to healthy controls, people with bipolar disorder have higher levels of CRP. CRP levels were moderately elevated between episodes and during depression, and substantially elevated during episodes of mania.
Editor’s Note: This meta-analysis shows that CRP is linked to bipolar disorder, and the inflammatory burden is highest during mania. It remains to be seen whether anti-inflammatory treatments work best in patients with high CRP levels compared to normal CRP levels.
CRP is also a risk factor for cardiovascular disease, and lithium and other treatments for bipolar disorder probably lower CRP levels.
The same group of researchers previously showed that statins, drugs typically used to lower cholesterol, could help alleviate depression. Since statins have anti-inflammatory effects, they can probably reduce depression risk in addition to lowering cardiovascular risk, as initial studies suggest.
Other drugs with anti-inflammatory effects that may improve depression include the anti-arthritis drug celecoxib and the antibiotic minocycline. The amino acid N-acetylcysteine and omega-3 fatty acids also have anti-inflammatory effects and have been found to improve depression in some studies.
Kynurenine Pathway Suggests How Inflammation is Linked to Schizophrenia
The kynurenine pathway describes the steps that turn the amino acid tryptophan (the ingredient in turkey that might make you sleepy) into nicotinamide adenine dinucleotide. This pathway might be a connection between the immune system and neurotransmitters involved in schizophrenia.
A recent autopsy study by researcher Thomas Weickert and colleagues explored this link by determining that in the brains of people with schizophrenia and high levels of inflammation, messenger RNA for Kynurenine Aminotransferase II (KATII, a step on the kynurenine pathway) was elevated in the dorsolateral prefrontal cortex compared to the brains of people who died healthy and those with schizophrenia but low levels of inflammation.
The KATII mRNA levels also correlated with mRNA levels of inflammatory markers such as glial fibrillary acidic protein and interleukin-6.
Blood measures related to the kynurenine pathway also differentiated people with schizophrenia from healthy controls. People with schizophrenia had lower levels of tryptophan, kynurenine, and kynurenic acid in their blood. The low levels of kynurenic acid in the blood were correlated with deficits in working memory and smaller volume of the dorsolateral prefrontal cortex.
Weickert and colleagues suggest that blood levels of kynurenic acid might provide a measurable indicator of the degree to which people with schizophrenia are experiencing problems with executive functioning (planning and decision-making) and loss of brain volume.
Depression and Resilience Linked to Norepinephrine
Scientists have known for some time that heightened activity of dopaminergic neurons (neurons in the midbrain that contain the neurotransmitter dopamine) can make people vulnerable to depression. New research in animals suggests for the first time that noradrenergic neurons (those that contain the neurotransmitter norepinephrine) control the activity of dopaminergic neurons and that these noradrenergic neurons can make the difference between vulnerability to depression or resilience to stress. The research, published by Elsa Isingrini and colleagues in the journal Nature Neuroscience in 2015, showed that animals that cannot release norepinephrine are vulnerable to depression following chronic stress, but increasing the production of norepinephrine increases the animals’ resilience and reduces depression.
These findings may open up new avenues to treatment that target norepinephrine rather than or in addition to dopamine or serotonin, which is targeted by SSRI antidepressants, or selective serotonin reuptake inhibitors.
Serotonin 5-HT7 Receptors: Why Should We Care About Them?
5-HT7 is a type of receptor activated by the neurotransmitter serotonin. Some of the most potent effects of lurasidone (Latuda), an atypical antipsychotic with antidepressant effects in bipolar depression, and vortioxetine (Brintellix), a unique antidepressant for unipolar depression that also has positive effects on cognition, occur through the blockade of 5-HT7 receptors. The atypical antipsychotics aripiprazole and sulpiride also act on 5-HT7 receptors.
Researcher Agnieszka Nikiforuk summarized the research to date on 5-HT7 receptors in the journal CNS Drugs in 2015.
The receptors play a role in regulating sleep and circadian rhythms, which may explain why drugs that target them can be helpful in depression. Drugs that target 5-HT7 receptors have also improved learning and memory.
One subject of research into 5-HT7 receptors is whether better results come from blocking the receptors or stimulating them.
Blockade of 5-HT7 receptors has improved depression-like symptoms in animals and enhances the effects of sub-therapeutic doses of antidepressants. In other animal studies, stimulation of the receptors has appeared promising for the prevention of age-related cognitive decline.