Early Precursors of Mood Disorders in Young Children of Parents with Bipolar or Unipolar Disorder

At the 2020 meeting of the International Society for Bipolar Disorders, researcher Caroline Vandeleur presented findings from a 13-year study of children in Switzerland who have a parent with bipolar disorder or major depressive disorder. In contrast to findings from the US presented by Danella Hafeman, Vandeleur and colleagues found no evidence of psychopathology in 4 year-olds. They did find that in 7-year-olds, children of a parent with major depressive disorder were four times more likely to have a separation anxiety disorder. In an overall sample of 449 children with a mean age of 10 who were followed up for 13 years, major depression tended to be preceded by anxiety disorders. Participants who went on to be diagnosed with bipolar disorder had earlier symptoms of depression, subthreshold hypomania, conduct disorders, and drug abuse. These were especially common in those who had a parent with bipolar disorder.
Editor’s Note: These data indirectly confirm other observations in which children at high risk for mood disorders in the US showed earlier signs of psychopathology than those in other countries including the Netherlands and Canada.
Clinical Risk Prediction in Youth at Risk for Bipolar Spectrum Disorder and Relapse

Researchers from two 15-year studies of bipolar youth, COBY (The Coarse and Outcome of Bipolar Youth Study) and BIOS (Bipolar Offspring Family Study), have used the longitudinal data from their studies in order to create a risk calculator that can predict an individual’s likelihood of illness.
At the 2020 meeting of the International Society for Bipolar Disorders, researcher Danella Hafeman presented research on a risk calculator that predicts the 5-year risk for onset of a bipolar disorder spectrum diagnosis (BPSD) in young people at high risk and can reasonably distinguish those who will receive a diagnosis from those who will not.
Some of the factors used in the risk calculator include dimensional measures of mania, depression, anxiety, and mood lability; psychosocial functioning; and the age at which parents were diagnosed with a mood disorder.
Hafeman reported that there was a 25% risk that offspring of a bipolar parent would develop a bipolar disorder spectrum diagnosis. In a population ranging in age from 6 to 18 years, Hafeman and colleagues found that anxiety and depression symptoms were a sign of vulnerability to a bipolar spectrum disorder, while subthreshold manic symptoms indicated that a bipolar spectrum disorder could soon emerge. Sudden or exaggerated changes in mood were also an important predictor of BPSD.
Hafeman and colleauges noted that even in children as young as 2 to 5 years old, there were already signs of anxiety, aggression, attention problems, depression, and sudden mood changes in those who would go on to receive a diagnosis of bipolar spectrum disorder.
The researchers were also able to predict which patients with BPSD would have a relapse. According to Hafeman and colleagues, “The most influential recurrence risk factors were shorter recovery lengths, younger age at assessment, earlier mood onset, and more severe prior depression.”
Editor’s Note: Offspring of a parent with bipolar disorder are at high risk for anxiety, depression, attention deficit hyperactivity disorder (ADHD), oppositional defiant disorder, and bipolar disorder. Parents should be alert for the symptoms of these illnesses and seek evaluation and treatment for their children as necessary. Parents should also be aware of the risk factors above that contributed to the risk calculator.
Parents can aid physicians in their evaluation by joining our Child Network and keeping weekly ratings of their children’s symptoms of depression, anxiety, ADHD, oppositional behavior, and mania.
Danish Population-Based Study Identifies New Drug Candidates for Bipolar Disorder
At the 2020 meeting of the International Society for Bipolar Disorders, Lars Kessing of the Psychiatric Center Copenhagen described a study that examined incidence of bipolar disorder among a total of 1,605,365 participants who purchased one of six common medications over a ten-year-period, with the goal of identifying drugs that might be repurposed to prevent or treat bipolar illness. The drugs were non-aspirin nonsteroidal anti-inflammatory drugs (NSAIDs such as ibuprofen), low-dose aspirin, high-dose aspirin, statins, allopurinol, and angiotensin.
Because Denmark has population-based healthcare data, the researchers were able to identify participants who purchased these medications between 2005 and 2015, and could also assess these participants for two outcome measures: 1) whether they had received a diagnosis of mania or bipolar disorder as an inpatient or outpatient at a psychiatric hospital, and 2) a combined measure of whether they had received a diagnosis for mania or bipolar disorder in any setting or initiated lithium use. The data on these participants were compared to a random sample of 30% of the population of Demark.
Kessing and colleagues found that among those with steady use of low-dose aspirin, statins (used to lower blood cholesterol), and angiotensin agents (which can lower blood pressure), there was a significant decreased incidence of mania/bipolar disorder on both outcome measures.
In contrast, among those taking non-aspirin NSAIDs and high-dose aspirin, there was an increased incidence of bipolar disorder. (There were no statistically significant findings with regard to allopurinol, which is used to treat gout and kidney stones.)
The researchers concluded that population-based studies such as these can be used to identify drugs that may have secondary benefits, in this case low-dose aspirin, statins, and angiotensin agents, which have already been identified as potentially therapeutic in other research.
Increased Risk for Dementia in Bipolar Disorder

At the 2020 meeting of the International Society for Bipolar Disorders, researcher Flavio Kapczinski described a recent meta-analysis of 10 studies that found that bipolar disorder is a risk factor for dementia, and that lithium treatment can decrease the incidence of dementia in people with bipolar disorder.
The ten studies included a total of 6,859 participants with bipolar disorder and 487,966 healthy control participants. People with bipolar disorder were 2.96 times more likely to develop dementia than those without bipolar disorder. Five of the studies included information about treatment with lithium, which was found to decrease the risk of dementia among those with bipolar disorder by a little more than half (0.54).
Five studies also revealed that the risk of progression to dementia was higher among those with bipolar disorder than among those with major depressive disorder. In addition, one of the ten studies explored predictors of dementia in people with bipolar disorder and found that those who experienced more mood episodes had a higher risk of dementia.
Editor’s Note: It appears that the number of mood episodes a person experiences predicts dementia, and it has previously been found to predict the emergence of cognitive impairment. Prevention is the name of the game, and lithium is the best defense. My new mantra: “Prevent Episodes, Protect the Brain, Use More Lithium.”
Cognitive Abnormalities in Patients Recently Diagnosed with Bipolar Disorder

At the 2020 meeting of the International Society for Bipolar Disorders, researcher Kamilla Miskowiak described a study in which she and her colleagues grouped 158 patients in remission from recently diagnosed bipolar disorder into groups based on their neurocognitive functioning and particularly their emotional processing, and also observed cognitive function in 52 first-degree relatives of those with bipolar disorder. These groups were compared to 110 healthy control participants.
Miskowiak and colleagues identified three clusters among the patients with bipolar disorder: 23% were globally impaired, 31% were selectively impaired, and 46% had normal cognition. Those who were globally impaired had problems recognizing facial expressions in social scenarios. Cognitive impairment has previously been documented in patients who have had a longer duration or more episodes of bipolar illness.
First-degree relatives of cognitively impaired patients had impaired recognition of facial expressions, but their cognition in non-emotional areas was normal. Miskowiak and colleagues concluded that the impaired affective cognition in relatives of patients with neurocognitive impairment was an indication of inherited risk for bipolar disorder.
Editor’s Note: Children with bipolar disorder also have this deficit in facial emotion recognition. That 23% of recently diagnosed patients with bipolar disorder were globally impaired indicates that some cognitive impairments can emerge early in the course of bipolar disorder. Researcher Lakshmi Yatham has previously found that cognition improves after a first episode of mania only if no further episodes occur in the one year following, indicating that episode prevention is crucial even after a patient’s first episode.
White Matter Disturbances in Bipolar Disorder
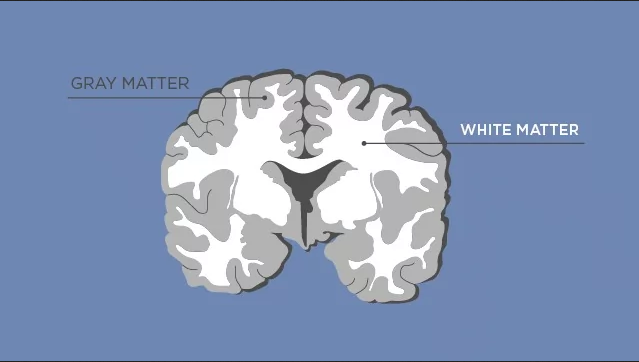
At the 2020 meeting of the International Society for Bipolar Disorders, researcher Clare Beasley described the cellular and molecular underpinnings of the white matter abnormalities typically seen in children and adults with bipolar disorder. Researchers consistently see white matter abnormalities in neuroimaging studies of bipolar disorder, but not much is understood about what creates these deficits.
Beasley and colleagues studied autopsy specimens and found that compared to controls, people with bipolar disorder had a number of abnormalities affecting glial cells, lipid composition, and axons.
The researchers found increased density of oligodendrocytes (glial cells that produce the myelin that wraps around axons, the long fibers of nerve cells where impulses travel out to other cells) and an associated protein called CNP in the prefrontal cortex. The myelin is what makes up white matter, while gray matter consists of cell bodies of neurons and glial cells.
People with bipolar disorder also had differently-shaped astrocytes, another type of glial cell that abuts synapses. The researchers found changes in lipid composition, including phospholipid and fatty acid levels, in the white matter of people with bipolar disorder. There were also problems with axons. Beasley and colleagues noted lower density of axon-associated proteins, which are involved in transport of substances along the axons in people with bipolar disorder.
The authors conclude that these data implicate specific disturbances in oligodendrocytes and axonal function associated with the white matter alterations usually seen in neuroimages of people with bipolar disorder.
Bipolar Disorder in Pregnancy and the Postpartum Period

At the 2020 meeting of the International Society for Bipolar Disorders, researcher Veerle Bergink reported several findings from a recent meta-analysis of articles on pregnancy and bipolar disorder. Bergink and colleagues found that pregnant women with bipolar disorder have a 37% risk of a postpartum relapse, more than twice the risk of postpartum mental disorders in the general population.
Using lithium as a treatment in the first trimester of pregnancy increased risk of congenital malformations in the fetus, but the risk was much smaller than previously thought and could be monitored by ultrasound.
Bergink and colleagues also reported that in a sample of 645 women with first-onset postpartum psychosis who received followup over a period of 7 to 25 years, 43% had no subsequent severe episodes outside of the postpartum period.
Another finding was that women with postpartum severe depression or mania had abnormalities in T cells, which are important in immune response.

