Lithium is a Lifesaver in Bipolar Disorder
Batya Swift Yasgur MA, LSW reported in Medscape Medical News on November 28, 2022 that “Mood stabilizers protect against suicide and all-cause mortality in patients with bipolar disorder (BD), including natural mortality, with lithium emerging as the most protective agent, new research suggests.
Investigators led by Pao-Huan Chen, MD, of the Department of Psychiatry, Taipei Medical University Hospital, Taiwan, evaluated the association between the use of mood stabilizers and the risks for all-cause mortality, suicide, and natural mortality in over 25,000 patients with BD and found that those with BD had higher mortality.
However, they also found that patients with BD had a significantly decreased adjusted 5-year risk of dying from any cause, suicide, and natural causes. Lithium was associated with the largest risk reduction compared with the other mood stabilizers.“
AiTBS Superior to ECT in Small Study
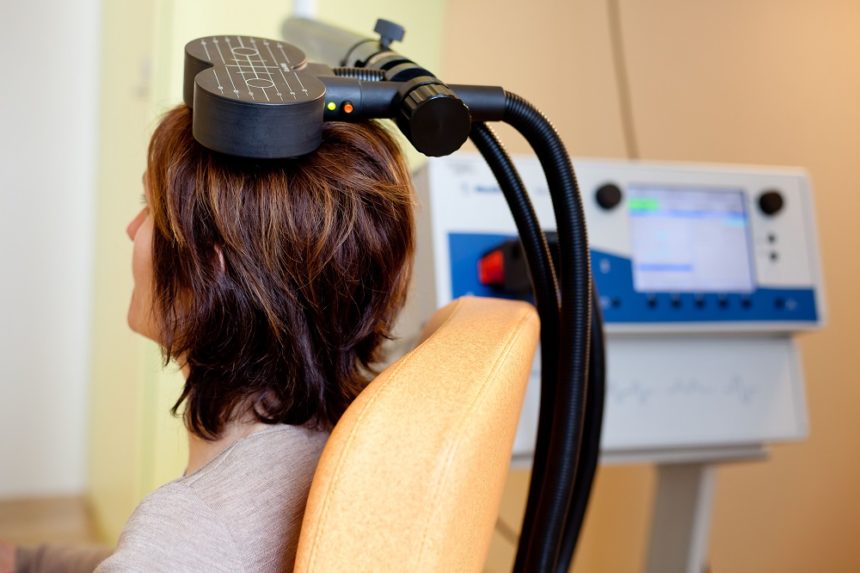
Researchers Erica Jensen and Nolan Williams reported in abstracts of a paper that they were to present at the 2020 meeting of the Society of Biological Psychiatry in May that daily sessions of accelerated intermittent theta burst transcranial stimulation (aiTBS) over five or more days produced better results in 15 patients hospitalized for depression and suicidality than in matched patients who received electro-convulsive therapy.
AiTBS is a form of repeated transcranial magnetic stimulation (rTMS), in which a magnetic coil is applied to a patient’s scalp, producing electrical changes in the brain.
The aiTBS treatment was delivered to the left dorsolateral prefrontal cortex. It consisted of 1800 pulses per session, at 80% of a patient’s resting motor threshold with a 50-minute inter-session interval.
The patients in the study were matched (for age, gender, and treatment resistance) to patients who were hospitalized and given ECT. Among patients who received aiTBS and were discharged after an average of 8.4 days, there was an 86% response rate and a 73% remission rate. Among the patients who received ECT, who were discharged after an average of 22.3 days, there was a 53% response rate and a 40% remission rate. With further ECT, response and remission rates increased to 73% and 67%. Time to remission was 3.5 days with aiTBS and 31.3 days for ECT. The investigators concluded conservatively, “Our results suggest that aiTBS could have comparable efficacy to ECT, with potentially faster resolution of acute severe depression.”
Editor’s Note: ECT has been the gold standard treatment for severe depression and suicidality and now we may have a platinum comparator. If these findings are replicated, they could represent a paradigm shift in the treatment of severe depression. Hopefully, this novel form of rTMS will be fast-tracked for approval by the Food and Drug Administration (FDA).
Cannabis Use in Adolescence Linked to Depression and Suicidality in Young Adulthood

In a meta-analysis published in the journal JAMA Psychiatry in 2019, researcher Gabriella Gobbi and colleagues analyzed findings from 11 studies including a total of 23,317 participants and found that cannabis use in adolescence (before age 18) was associated with a significantly increased risk of depression, suicidality, and suicide attempts in young adulthood (between 18 and 32 years of age).
The researchers did not find a link between cannabis use and anxiety.
Editor’s Note: Cannabis use is not as harmless as many teens may believe.
Lithium Better than Other Mood Stabilizers for Youth with Bipolar Disorder
A new study by Danella M. Hafeman and colleagues finds that lithium is superior to other mood stabilizers in young people. The data in this case come from 340 youth aged 7–17 who participated in a study known as Course and Outcome of Bipolar Youth (COBY).
At each visit over an average of 10 years, participants reported medications taken, symptoms they had experienced, etc. during the preceding six-month period. During times that participants had taken lithium (compared to other mood stabilizers) they were older, on fewer antidepressants, and they were less likely to have an anxiety disorder.
Those participants who took lithium had half as many suicide attempts, fewer depressive symptoms, less psychosocial impairment, and less aggression than those who took other mood stabilizers.
The researchers concluded, “Findings are consistent with adult studies, showing that lithium is associated with decreased suicidality, less depression, and better psychosocial functioning. Given the paucity of evidence regarding lithium in children and adolescents, these findings have important clinical implications for the pharmacological management of youth with bipolar disorder.”
Editor’s Note: Lithium should especially be considered in those with a family history of mood disorders, and in particular in those with a family history of good response to lithium. Lithium is under-prescribed in both adults and children and should be given much higher consideration in light of the multiple benefits it provides in addition to mood stabilization. These include maintenance of memory, increases in longevity (perhaps based in its ability to increase the length of telomeres, the bits of protective material at the end of DNA strands that deteriorate with age and illness), and neuroprotection against loss of gray and white matter volume in the brain, which often occurs in mood disorders.
Early Predictors of Suicide and Lithium as an Anti-Suicide Drug
 At the 2019 meeting of the International Society for Bipolar Disorders, researcher Gin S. Malhi discussed early predictors of suicide in people with bipolar disorder, such as younger age of illness onset, early life stressors, and family history of suicide. Impulsivity, hopelessness, cognitive deficits and substance use are risk factors, both for suicide in general and for an imminent suicide attempt. Proximal risk factors that indicate someone may make a suicide attempt soon include: mood swings, rapid cycling, increased depression, hospitalization, and severe anxiety.
At the 2019 meeting of the International Society for Bipolar Disorders, researcher Gin S. Malhi discussed early predictors of suicide in people with bipolar disorder, such as younger age of illness onset, early life stressors, and family history of suicide. Impulsivity, hopelessness, cognitive deficits and substance use are risk factors, both for suicide in general and for an imminent suicide attempt. Proximal risk factors that indicate someone may make a suicide attempt soon include: mood swings, rapid cycling, increased depression, hospitalization, and severe anxiety.
Editor’s Note: Among all psychotropic drugs, lithium has the best data supporting its anti-suicide effects, both at therapeutic doses in patients with bipolar disorder and at trace levels in the water supply in the general population. People who live in locations where more lithium is naturally present in the water supply have lower rates of suicide than those who live in places with less lithium in the water. Malhi also noted that the antioxidant N-acetylcysteine (NAC), which has positive effects on mood and habitual behaviors, can reduce the incidence of lithium-induced dysfunction of the kidneys.
Lithium Superior to Other Mood Stabilizers in a Longitudinal Study of Bipolar Youth
At a late-2018 scientific meeting, researcher Danella Hafeman and colleagues reported some results of the Course and Outcome of Bipolar Youth (COBY) study. The study includes long-term follow up of 413 youth with bipolar disorder, who ranged in age from 7 to 17 years old. Hafeman and colleagues reported that taking lithium more than 75% of the time was linked to fewer suicide attempts, fewer depressive symptoms, and fewer psychosocial difficulties than taking another mood stabilizer (such as an atypical antipsychotic, lamotrigine, or valproic acid) more than 75% of the time after adjusting for demographic variables.
Despite the limitations of observational studies such as this one, the authors concluded, “Our findings are consistent with studies in adult populations, showing that lithium (compared to other mood stabilizers) is associated with decreased suicidality, less depression, and better psychosocial functioning. Given the paucity of evidence regarding lithium in children and adolescents, these findings have important clinical implications for the pharmacological management of youth with [bipolar disorder].”
Editor’s Note: These observations are consistent with several other studies. Researcher Barbara Geller and colleagues observed in eight years of follow up of children diagnosed with bipolar disorder that those who were treated with lithium spent more time in remission than those who took other medicines. A randomized controlled study by researcher Robert Findling and colleagues documented that maintenance lithium treatment was more effective than placebo at preventing bipolar episodes. Together, these data suggest that lithium should be used more often in the long-term treatment of children with bipolar disorder.
Way ahead of his time in about 1993, the renowned child psychiatrist Dennis Cantwell said something like this: “If I had an adolescent child with a first manic episode, I would have him stay on lithium for the rest of his life.” He seems to have been prescient, as evidence of the many benefits of lithium over other alternatives in the treatment of both children and adults has been accumulating.
An open-access review article this editor (Robert M. Post) published in the journal Neuropsychopharmacology in 2017, “The New News about Lithium: An Underutilized Treatment in the United States,” argues that lithium’s many benefits have been underestimated, while its side effects have been overestimated. It is my view that it would be beneficial if lithium were more often included in the treatment regimen of adults as well as children and adolescents with bipolar disorder.
Lithium has an astounding range of effectiveness. It prevents recurrent depressions and suicide (even in those with unipolar depression), increases hippocampal and cortical volume, protects memory, and increases the length of telomeres (the end portions of chromosomes that protect them as they replicate). In multiple animal models of neurological diseases, it has also been found to be neuroprotective and to reduce the size of brain lesions.
Risk of Suicide in People with Bipolar Disorder: Lowest with Lithium, Highest with Antidepressants
Researcher Markku Lähteenvuo and colleagues reported in the journal JAMA Psychiatry in early 2018 that long-acting injectable antipsychotics and lithium were best at preventing re-hospitalization in 18,018 bipolar patients in Finland who received an average of more than 7 years of follow up. Lähteenvuo and colleagues have now gone on to analyze suicide data from the same cohort of patients with bipolar disorder, and report that those taking lithium had the lowest rate of suicide, while those taking valproate had the next lowest suicide rate. Those patients with bipolar disorder who were treated with antidepressants had the greatest suicide rate. The suicide rate was particularly high for those once-hospitalized patients taking the MAO inhibitor antidepressant meclobemide, which is not approved for use in the US. Increased rates of suicide were also seen with use of sedatives and benzodiazepines.
Editor’s Note: Evidence continues to mount that lithium should be the definitive first line therapy in bipolar disorder for a multitude of reasons (as this editor Robert M. Post reviewed in an open-access article in the journal Neuropsychopharmacology in 2017). Still, lithium is not often prescribed for people with bipolar disorder in the US, and this does not seem to be in these patients’ best interests.
Use of antidepressants in bipolar disorder has remained controversial, but it is common in clinical practice despite a lack of evidence that it is effective, and the presence of some evidence that it is actually harmful. Antidepressant use in a person with bipolar disorder may cause switching into mania, cycle acceleration, dysphoria induction, and even suicide.
Clinicians should take these data seriously and overcome the impulse (leftover from treating unipolar depression) to use unimodal antidepressants as first line or adjunctive therapy for bipolar depression. Antidepressants are only effective in the long term in about 15% of patients with bipolar depression, and now it appears antidepressant use also carries an additional risk of suicide.
Single Dose of Ketamine Reduces Suicidal Ideation
A systematic review and meta-analysis by Samuel T. Wilkinson and colleagues in the American Journal of Psychiatry analyzed individual patient data from 10 studies in which a single intravenous dose of ketamine was given to patients with suicidal ideation. The review included data from a total of 167 participants.
Wilkinson and colleagues found that ketamine reduced suicidal ideation within 24 hours, and these effects lasted for up to seven days. Mood also improved, but the reduction in suicidal ideation was independent of the degree of improvement in depression.
Among the participants, 54.9% were free of suicidal ideation at 24 hours after the infusion, 60.0% were free of suicidal ideation one week after the infusion, and 61.1% were free of suicidal ideation at two weeks.
Editor’s Note: The authors report that there is much to clarify about ketamine treatment before it can be used clinically to treat patients at risk for suicide. However, ketamine’s powerful and rapid effects offer an interesting alternative to other slow-acting treatment options, and could be an ideal acute treatment for patients arriving in an emergency room because of high suicide risk. A ketamine injection could be especially useful for those who are not admitted to the hospital, as it could produce anti-suicidal effects that could help carry a patient over until their next psychiatric appointment.
Lithium Treatment Lowers Suicide Rate in People with Bipolar Disorder
A large study that made use of a Swedish health database has shown that lithium reduces suicide rates in bipolar disorder. The study by researcher Jie Song and colleagues was published in the American Journal of Psychiatry in 2017.
The study included eight years of data from 51,535 people with bipolar disorder. During that time, there were 10,648 suicide-related events recorded, such as suicide attempts or completed suicides. The researchers compared suicide rates when patients were taking lithium to rates when they were off the drug, and found that lithium reduced attempted or completed suicide by 14%. Song and colleagues also looked at suicide rates for people taking valproate, and found that these were no better than when patients were off valproate, implying that treatment alone is not enough to reduce the suicide rate and the benefit is specific to lithium use.
Song and colleagues estimate that 12% of the suicide-related events among the patients included in the study might have been avoided if the patients had taken lithium for the entire study period. While there are other clinical considerations to make when selecting an appropriate treatment for a given patient, the researchers suggest that lithium treatment should be considered for patients with bipolar disorder who have expressed suicidal intentions or who are otherwise at risk for suicide.
Brain Scans Differentiate Suicidal from Non-Suicidal Patients with Bipolar Disorder
 People with bipolar disorder are at high risk for suicidal behavior beginning in adolescence and young adulthood. A 2017 study by Jennifer A. Y. Johnston and colleagues in the American Journal of Psychiatry uses several brain-scanning techniques to identify neurobiological features associated with suicidal behavior in people with bipolar disorder compared to people with bipolar disorder who have never attempted suicide. Clarifying which neural systems are involved in suicidal behavior may allow for better prevention efforts.
People with bipolar disorder are at high risk for suicidal behavior beginning in adolescence and young adulthood. A 2017 study by Jennifer A. Y. Johnston and colleagues in the American Journal of Psychiatry uses several brain-scanning techniques to identify neurobiological features associated with suicidal behavior in people with bipolar disorder compared to people with bipolar disorder who have never attempted suicide. Clarifying which neural systems are involved in suicidal behavior may allow for better prevention efforts.
The study included 26 participants who had attempted suicide and 42 who had not. Johnston and colleagues used structural, diffusion tensor, and functional magnetic resonance imaging (MRI) techniques to identify differences in the brains of attempters and non-attempters.
Compared to those who had never attempted suicide, those who had exhibited reductions in gray matter volume in the orbitofrontal cortex, hippocampus, and cerebellum. They also had reduced white matter integrity in the uncinate fasciculus, ventral frontal, and right cerebellum regions. In addition, attempters had reduced functional connectivity between the amygdala and the left ventral and right rostral prefrontal cortex. Better right rostral prefrontal connectivity was associated with less suicidal ideation, while better connectivity of the left ventral prefrontal area was linked to less lethal suicide attempts.






