Cannabis and Cannabinoids Don’t Work for Pain or Posttraumatic Stress Disorder
Aaron S. Wolfgang, MD and Charles W. Hoge, MD reviewed data on cannabis in JAMA Psychiatry and found that there were big placebo effects and no evidence for effectiveness of cannabis in military personal.
This negative data, along will all the liability of cannabis potentially causing or triggering psychosis, bipolar disorder, and schizophrenia (as well as possibly contributing to cognitive dysfunction, worsening anxiety and depression in patients with mood disorders) makes the use of pot for medical purposes an entirely foolhardy proposition, as well as a waste of money.
Legalization of pot has helped people avoid jail but precipitated a rash of use and over use.
So the bottom line from this editor is: Get Your Priorities Straight. Cannabis and Cannabinoids Don’t Work for Pain or Posttraumatic Stress Disorder and they Worsen Most Everything Else. Save your Money and Do Something Nice for Yourself and Others Instead.
MDMA Superior to Placebo in Treatment of Severe PTSD

An article by researcher Jennifer M. Mitchell and colleagues published in the journal Nature in 2021 reported that MDMA was more effective than placebo at treating severe post-traumatic stress disorder in an 18-week phase 3 clinical trial.
The article reported on a randomized, double-blind, placebo-controlled, multi-site trial that took place in the US, Canada, and Israel. Participants in the trial had severe PTSD, and in some cases also had dissociation, depression, a history of alcohol or substance use disorders, or childhood trauma. In the trial, 91 participants were required to stop any current psychiatric medications for a “washout” period, and then were randomized to either a group that received 12 therapy sessions plus placebo or a group that received 12 therapy sessions and 3 doses of MDMA, which were administered in a clinical setting.
Two months after the last therapy session, participants who had received MDMA during the trial showed greater reductions in PTSD symptoms and less functional impairment than those who were assigned to the placebo group during the trial. At the endpoint of the study, 67% of participants in the MDMA group no longer met the criteria for a PTSD diagnosis, compared to 32% of the placebo group.
Side effects that were more prevalent among the MDMA group were typically transient and mild to moderate in severity. These included muscle tightness, decreased appetite, nausea, sweating, feeling cold, and increased blood pressure and heartrate. The MDMA group did not show any increases in drug abuse or suicidality compared with the placebo group, and MDMA had similar effects among those participants with and without comorbid conditions. The authors concluded that MDMA was highly efficacious, safe, and well-tolerated as a treatment for PTSD and urged that further study of the treatment be done without delay.
Currently, US Food and Drug Administration (FDA)–approved treatments for PTSD include the selective serotonin reuptake inhibitors (SSRIs) sertraline and paroxetine, but approximately half of PTSD patients do not respond to these drugs or to evidence-based trauma-specific psychotherapy or cognitive-behavioral therapies. The FDA has designated MDMA-assisted therapy for PTSD a “Breakthrough Therapy.” This designation indicates that the therapy may be a substantial improvement over existing therapies for a serious condition, and is intended to speed up the drug development and review process.
MDMA (or 3,4-methylenedioxymethamphetamine) is the same chemical used recreationally under the name ecstasy or molly. However, the positive effects in the trial followed careful dosing (which is impossible with street drugs) and targeted therapy sessions.
Better One-Year Clinical Outcomes After Four Weeks of Theta Burst Stimulation for PTSD Than After Two Weeks
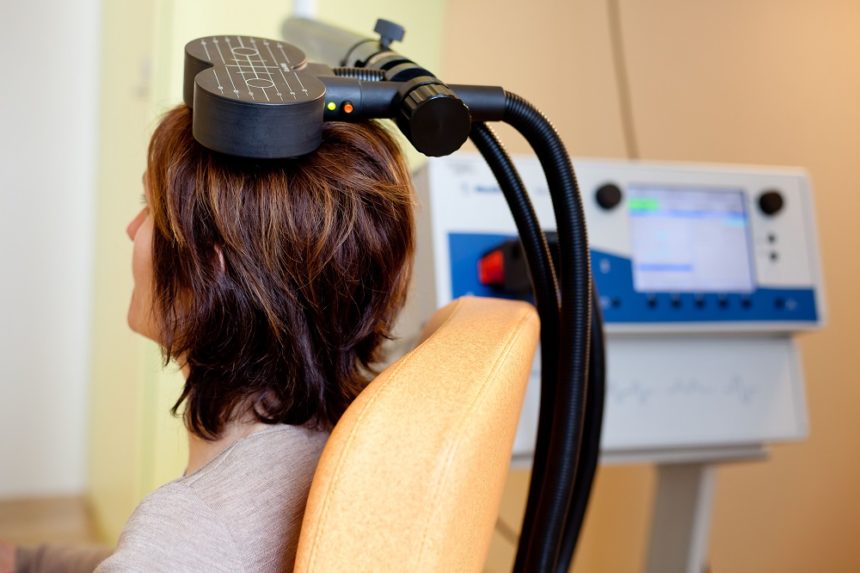
In a 2019 article in the journal Neuropsychopharmacology, Nicholas J. Petrosino and colleagues described findings from one year of follow-up with veterans suffering from post-traumatic stress disorder (PTSD) who received intermittent theta burst transcranial magnetic stimulation (iTBS) in a four-week crossover study.
In the first two weeks of the study, half of the 50 participants (who were mostly male and had an average age of 51) received iTBS while the others were given a sham procedure. Then all the participants received iTBS on an open (non-blind) basis for two more weeks.
At one month, those who had received four total weeks of iTBS had better outcomes than those who had received only two weeks of active iTBS. These results were published in the American Journal of Psychiatry in 2019 in an article by Noah S. Philip and colleagues.
The researchers went on to look at longer-term outcomes, namely time until relapse (a major event such as a re-hospitalization or suicide). After one year, those who received four weeks of iTBS went 9 to 11 months without relapsing (296.0 days ± 22.1), while those who received only two weeks of iTBS went 5 to 7 months before relapsing (182.0 days ± 31.9).
It seems that more iTBS may be better than less iTBS for PTSD in both the short and long term.
Prazosin Effective and Well-Tolerated for PTSD in Young People
In a poster session at the 2019 meeting of the American Academy of Child and Adolescent Psychiatry (AACAP), three posters highlighted the efficacy and tolerability of prazosin, a drug typically used to treat high blood pressure, for the treatment of childhood-onset post-traumatic stress disorder (PTSD).
Researchers Samira Khan and Taniya Pradhan of West Virginia University reviewed cases in which 39 patients aged 8–19 received 1–5 mg of prazosin at bedtime. The mean dose was 1.72 mg. Sleep (including nightmares) improved in 92.3% of the youths, and mood improved in 33.3%. Sleep improved more in patients who received lower doses (1–2 mg) than those who received higher doses. About 70% of the patients whose data were included in the case series were also receiving psychotherapy while being treated with prazosin.
In another poster, researcher Vladimir Ferrafiat and colleagues from University Hospital of Rouen in France reported on a prospective study of 18 participants under age 15 with severe PTSD who were unresponsive to other medications. The participants were given 1 mg of prazosin at bedtime, which was increased to 3 mg in 20% of the participants. The youth were assessed weekly over a one-month period. Improvement was seen in all domains, including sleep, nightmares and daytime intrusive symptoms. Prazosin was well tolerated, with only one patient experiencing low blood pressure, which did not necessitate withdrawal from the study.
In the final poster, researcher Fatima Motiwala and colleagues reviewed the literature on the treatment of PTSD in children. Motiwala indicated that among the options, prazosin was widely used in her hospital, at doses starting at 1 mg given at bedtime and increasing to a mean of 4 mg at bedtime with excellent results and tolerability.
Editor’s Note: Although these were not double-blind controlled studies, the findings are noteworthy in that they provide consistent data on the effectiveness and tolerability of prazosin in low doses in children with PTSD, essentially mirroring controlled data in adults, where higher doses are typically required.
Newly Identified Effects of N-Acetylcysteine
 In a talk at the 2019 meeting of the International Society for Bipolar Disorders, researcher Michael Berk, who was responsible for some of the initial findings on the effects of the antioxidant N-acetylcysteine (NAC), summarized some of the newer findings about the treatment.
In a talk at the 2019 meeting of the International Society for Bipolar Disorders, researcher Michael Berk, who was responsible for some of the initial findings on the effects of the antioxidant N-acetylcysteine (NAC), summarized some of the newer findings about the treatment.
NAC has been found to be effective in bipolar depression and in the treatment of both positive and negative symptoms of schizophrenia. It also helps in the avoidance of cocaine, alcohol, tobacco, and marijuana. It can reduce habitual behaviors such as gambling, obsessive compulsive disorder (OCD), and trichotillomania (compulsive hair-pulling) and irritability and motor stereotypy (repeated movements) in autism.
A 2016 study by researcher Sudie E. Back and colleagues in the Journal of Clinical Psychiatry found that NAC improved symptoms of post-traumatic stress disorder (PTSD) in veterans who also had depression and substance use disorders at a dosage of 2.4 grams/day.
According to Berk, NAC also reduces the incidence of lithium-related renal failure and reduces mitochrondrial toxicity. One study reported that it improved working memory in patients with schizophrenia.
In his talk, Berk also noted that statins offer an interesting new avenue for treatment. Several studies have suggested statins can improve mood or reduce the likelihood of a depressive recurrence. Angiotension-active drugs (inhibitors) have also been reported to decrease the incidence of depression and to improve cognition.
Recent Cannabis Use Linked to Greater Symptoms of Anxiety and Mood Disorders and Less Response to Treatment
 In a 2018 systematic literature review published in the Journal of Clinical Psychiatry, researcher George Mamman and colleagues reported that across 12 studies of people with anxiety and mood disorders, participants who had used cannabis in the previous six months had more symptoms than those who had used less cannabis or no cannabis during that period.
In a 2018 systematic literature review published in the Journal of Clinical Psychiatry, researcher George Mamman and colleagues reported that across 12 studies of people with anxiety and mood disorders, participants who had used cannabis in the previous six months had more symptoms than those who had used less cannabis or no cannabis during that period.
The 12 studies reviewed included a total of 11,959 participants. Four studies looked at post-traumatic stress disorder (PTSD), one at panic disorder, five at bipolar disorder, and 2 at depressive disorder. In addition to finding that recent cannabis use was associated with greater symptoms, the authors of the review also found that in 10 of the 12 studies, recent cannabis use was associated with less symptom improvement in response to treatment for bipolar disorder, depression, and PTSD; including both medication and psychotherapy.
In bipolar disorder, cannabis use was associated with greater symptom severity. Cannabis use for more than one year was linked to more recurrences of mania and shortened time to a recurrence. Compared to participants with no prior use of cannabis, those with a cannabis use disorder had more depressive symptoms, including sleep troubles and loss of interest in activities one had previously enjoyed.
In PTSD, any cannabis use at the beginning of the analysis period and sustained use of cannabis over time were both linked to greater symptom severity in the four months following the beginning of the analysis.
Mammen and colleagues cautioned that these results are limited based on the differences in measurements across the 12 studies, the inpatient populations under study, and the uncontrolled nature of the cannabis the participants accessed on their own time. However, the authors suggest that the findings may inform patients’ and doctors’ conversations about whether or not to use cannabis.
Repeated Ketamine Reduces PTSD and Depression in the Short Term
In a 2018 open study by C. Sophia Albott and colleagues in the Journal of Clinical Psychiatry, veterans with post-traumatic stress disorder (PTSD) and a simultaneous diagnosis of major depression were treated with six infusions of intravenous ketamine over a 12-day period (Mondays, Wednesdays, and Fridays for two weeks).
Ketamine produced large improvements in both conditions. The remission rate was 80.0% for PTSD and 93.3% for depression. The median time to first relapse after the treatment was 41 days for PTSD and 20 days for depression.
One side effect of ketamine was that dissociative symptoms increased temporarily with repeated infusions. PTSD symptoms did not worsen among those participants taking ketamine.
The study was intended to evaluate the efficacy, safety, and durability of repeated ketamine infusions. Ketamine has been used in emergency rooms to rapidly treat depression and suicidality, but the effects of a single infusion fade within days. Albott and colleagues reported that this treatment scenario with multiple ketamine infusions produced rapid results that lasted longer than single ketamine infusions.
Editor’s Note: While this study found that repeated ketamine infusions were safe, it is possible that long-term use may lead to addiction. Researcher Nolan R. Williams and colleagues reported in a 2018 article in the American Journal of Psychiatry that ketamine works via activation of the opiate receptor. The drug naloxone, which rapidly reverses opiate overdose, completely blocked ketamine’s antidepressant effects.
PTSD Increases Risk of Lupus
 A new large 2017 study in the journal Arthritis and Rheumatology reports that post-traumatic stress disorder (PTSD) in women triples their risk of developing the autoimmune disease lupus. The study included 54,763 civilian women whose health data was tracked over a period of 24 years.
A new large 2017 study in the journal Arthritis and Rheumatology reports that post-traumatic stress disorder (PTSD) in women triples their risk of developing the autoimmune disease lupus. The study included 54,763 civilian women whose health data was tracked over a period of 24 years.
Not only did PTSD increase lupus risk, but any traumatic event doubled lupus risk compared to women who were not exposed to trauma.
The researchers, led by Andrea L. Roberts, were taken by surprise at the strong links between trauma and lupus. Trauma was more of a risk factor for lupus than smoking.
Type of Trauma Affects Gene Transcription Effects in PTSD
 In a 2017 article in the journal Neuropsychopharmacology, researcher Michael S. Breen and colleagues analyzed five separate studies of post-traumatic stress disorder (PTSD) and found that sex and type of trauma affected the immunological pathways that changed with PTSD. People with PTSD showed disruptions in gene expression in specific immunological pathways depending on what type of trauma they had experienced.
In a 2017 article in the journal Neuropsychopharmacology, researcher Michael S. Breen and colleagues analyzed five separate studies of post-traumatic stress disorder (PTSD) and found that sex and type of trauma affected the immunological pathways that changed with PTSD. People with PTSD showed disruptions in gene expression in specific immunological pathways depending on what type of trauma they had experienced.
Men exposed to combat traumas showed downregulation in a pathway related to wound healing, while men who were exposed to interpersonal traumas had upregulation in a signaling pathway mediated by the inflammatory marker IL-12. Women exposed to interpersonal traumas showed upregulation of two pathways—one related to lipid metabolism and the other related to MAPK (or mitogen-activated protein kinase) activity.
The participants with PTSD also showed a lot of the same disruptions across all types of trauma, including disruptions that affected cytokine, innate immune, and type 1 interferon pathways.
These data show that immune dysregulation and inflammatory pathways play a role in the pathophysiology of PTSD.
Eye Movement Desensitization and Reprocessing Can Improve PTSD
A 2014 meta-analysis of clinical trials showed that the therapeutic technique known as eye movement desensitization and reprocessing (EMDR) can reduce symptoms of post-traumatic stress disorder (PTSD). The meta-analysis also established that longer durations of EMDR treatment correlated with better outcomes.
The meta-analysis by Ying-Ren Chen and colleagues in the journal PLOS One evaluated 26 randomized controlled trials of EMDR in people with PTSD. Chen and colleagues found that EMDR reduced PTSD symptoms, depression, anxiety, and subjective distress.
EMDR is a psychotherapeutic technique intended to reduce the distress that a patient feels about a traumatic memory. The patient is encouraged to recall the traumatic event while focusing on an external stimulus. Typically this would mean using their eyes to track the therapist’s hand moving back and forth from left to right. This process can help patients reprocess the trauma and alleviate the stress that they feel upon recalling the traumatic memory.
Chen and colleagues found that EMDR sessions that lasted longer than one hour were more effective than those that lasted less than an hour. Another finding that was that groups led by therapists who were experienced in PTSD group therapy were more effective than groups led by therapists without that experience.
Other more recent research has established that traumatic memories can be reprocessed or even extinguished by making use of the memory reconsolidation window. Five minutes to one hour after a patient engages in active emotional recall of a traumatic memory, a window of time opens in which that memory is subject to reinterpretation and revision.
An experienced therapist can create a safe environment for a patient to recall traumatic events and find alternative ways of interpreting the experience—for example, by focusing on their strength in surviving the experience. This process resembles EMDR in many ways, but without the eye movements.
In a 2017 article in the journal Psychiatry Research, BNN Editor-in-Chief Robert M. Post and colleague Robert Kegan discuss the possibility of using the reconsolidation window to reprocess stressors that led to a depressive episode.