Lithium Increases Parathormone and Reduces Vitamin D Levels
Lithium treatment is associated with a moderate incidence of hyperparathyroidism, usually observed as an elevated concentration of calcium in the blood in addition to elevated parathormone levels, and often associated with the development of a tumor (adenoma) of the parathyroid gland.
In a recent study by Van Melick et al. published in the International Journal of Geriatric Psychiatry, among 111 patients with an average age of 75 years, 24-hour calcium excretion was elevated in only 3% of the patients, but levels of parathormone were elevated in 48%. Duration of lithium treatment was associated with lower vitamin 25OH D. Vitamin D is important for healthy bones and good cognitive functioning.
Editor’s Note: Lithium-induced hyperparathyroid should be investigated in those with elevated calcium levels, and if found, surgical removal of the parathyroid gland may be indicated. Low vitamin D is common in the US population. It is also particularly low in patients with mania and elderly patients on who have been on lithium for more than ten years. (Levels are below normal in 77% of these elderly individuals.) Assessment of vitamin D levels in those on long-term lithium is advisable, in addition to monitoring the thyroid, kidney function, and calcium metabolism.
High Level of Calcium Intake and Supplements May Be Harmful
 In a study of over 60,000 women, Swedish researcher Karl Michaëlsson et al. found that those women with the highest intakes of calcium (>1400mg/day) were at higher risk of mortality, particularly from cardiovascular causes such as cardiovascular disease and heart disease (but not stroke), than women with calcium intakes of between 600 and 1000mg/day. The research was published in the journal BMJ in 2013.
In a study of over 60,000 women, Swedish researcher Karl Michaëlsson et al. found that those women with the highest intakes of calcium (>1400mg/day) were at higher risk of mortality, particularly from cardiovascular causes such as cardiovascular disease and heart disease (but not stroke), than women with calcium intakes of between 600 and 1000mg/day. The research was published in the journal BMJ in 2013.
While calcium dietary supplements were not associated with elevated risk per se, those women with the highest calcium intake levels who also took supplements had a risk of mortality from all causes that was more than 2.5 times that of women with similar total calcium intake who did not take supplements.
Calcium levels in blood are tightly controlled by the body, but very low or very high calcium intake levels can override this control, causing imbalances.
The efficacy of calcium supplements for conditions such as osteoporosis or chronic kidney disease has not been established, and a healthy balanced diet and avoidance of water filters that remove calcium from drinking water may be best.
Lithium-Induced Hypercalcemia
In a poster at the 5th Biennial Conference of the International Society for Bipolar Disorders, researchers from the Netherlands including E.J. Regeer described the prevalence of hypercalcemia (high calcium levels) in patients with bipolar disorder who are treated with lithium. In a study of 314 patients taking lithium, Regeer and colleagues found that calcium levels were elevated in 15.6% of the patients, and the length of time patients had been treated with lithium was significantly related to the degree of hypercalcemia. It is recommended that blood levels of calcium be monitored in patients on lithium.
The researchers recommended testing for parathyroid hormone in blood in order to exclude other causes of hypercalcemia. They also suggested that when lithium cannot safely be discontinued or when its discontinuation does not resolve the hypercalcemia, other treatment for high blood calcium, including removal of the parathyroid, may be necessary.
The Role of Calcium in Genetic Vulnerability, Pathophysiology, and Treatment Of Bipolar Illness
One of the most consistent findings in biological psychiatry is that levels of intracellular calcium in blood elements (platelets and white cells) are higher than normal in patients with mood disorders, particularly bipolar disorder. These data are now supported by genome-wide association studies that have identified a relationship between alterations in a calcium channel and vulnerability to bipolar illness. The specific alteration is in the alpha-IC subunit of the L-type calcium channels, otherwise referred to as CACNA1C. These findings were initially reported by one group funded by the Welcome Trust, a charitable organization that funds health research, in a series of studies that included thousands of patients and controls. Investigator Pamela Sklar later replicated these findings in another large independent sample.
At the 65th Annual Scientific Convention of the Society of Biological Psychiatry, investigator Tyson Tragon reported that there were higher levels of CACNA1C in the cingulate cortex in autopsy specimens of those with bipolar illness than in controls. In a study of mice, some of which had the gene for the glutamate receptor subunit GLuR6 knocked out (i.e. production of the gene was artificially limited), the researchers found that the L-type dihydropyridine calcium channel blocker nimodipine decreased hyperactivity, amphetamine super-sensitivity, risk-taking behavior, and aggression in those with the gene removed. The dihydropyridine-type drugs like nimodipine also decreased stress-related immobilization in the wild type (the animal with normal genes) but not the knockout animals (the ones lacking GLuR6). These data suggest that alterations in a subunit of the dihydropyridine-responsive L-type calcium channel are a risk factor for bipolar illness, a brain abnormality in those who have the illness, and relevant to behavioral/pharmacological models.
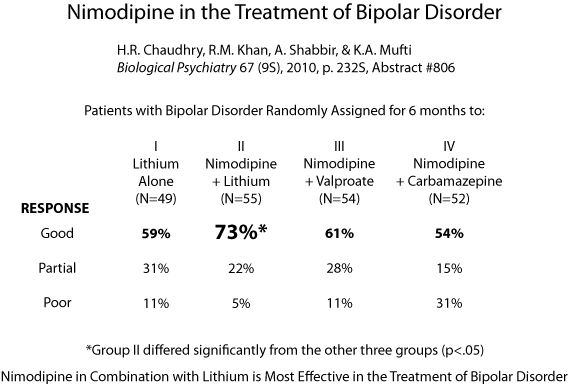
Several research groups have noted that treatment with the L-type calcium channel blocker nimodipine (Nimotop) can sometimes have positive effects in mania and depression in those poorly responsive to lithium carbonate. This has been documented by Pazzaglia and Post in double blind off-on-off-on clinical trials (i.e. during off trials patients received placebo and during on trials patients received nimodipine, but the raters were unaware which pill the patient had received). In several instances, a positive response continued when the patient was switched from nimodipine to another dihydropyridine, isradapine (DynaCirc), but not when patients were switched to a different L-type calcium channel blocker, the phenylalkylamine verapamil (sold under the names Calan, Covera, Isoptin, and Verelan), which acts at a slightly different site on the channel. Read more