Collaborative Care and Education Reduces Bipolar Depression
There is increasing evidence that patients with bipolar disorder benefit from special programs or clinics designed to teach them skills to cope with their illness. A 2015 article by Trijntje Y.G. van der Voort and colleagues in the British Journal of Psychiatry evaluated the effectiveness of a Dutch program that provided collaborative care to people with bipolar disorder.
One hundred thirty-eight patients in an outpatient clinic were randomized to receive either treatment as usual or a program of nurse-provided collaborative care that included psychoeducation, problem-solving treatment, systematic relapse prevention contracts, and monitoring of outcomes. These services were managed by mental health nurses. Those patients who received collaborative care had significantly less time with depressive symptoms at the 6-month and 12-month marks, and less severe depressive symptoms at 12 months (all findings with p values less than .01).
There was no significant difference in manic symptoms or treatment adherence. The authors suggest that collaborative care improves treatment for people with bipolar disorder, especially depression, which is most closely linked to impaired quality of life and disability.
Editor’s Note: Given this study and about a dozen others like it, it is time to conclude that psychoeducation and other components of collaborative care noted here are critical to the long-term management of bipolar disorder. Patients and their family members should insist that this be a part of routine care.
More Evidence for Cariprazine’s Efficacy in Bipolar Depression
In an eight-week study of the drug cariprazine for bipolar depression by Joe Calabrese and colleagues, patients who received 1.5mg/day doses of the drug showed more improvement in their illness and higher remission rates after six weeks than patients who received placebo. Side effects were rare, with mild or moderate akithisia (restless legs) being most common. Cariprazine is a dopamine D3 and D2 receptor partial agonist with preferential binding to D3 receptors.
Omega-3 Fatty Acids Improve Mood and Limbic Hyperactivity in Youth with Bipolar Depression
Children who have a parent with bipolar disorder are at risk for bipolar illness, but it may first present as depression. Treating these children with antidepressants has the risk of bringing on manic episodes. Researchers are looking for treatment options for youth at risk for bipolar disorder.
Robert McNamara and colleagues found that 12 weeks of omega-3 fatty acids (2,100 mg/day) significantly improved response rates in medication-free youth ages 9–20 years compared to placebo (64% versus 36%). Omega-3 fatty acids but not placebo also reduced the activation of limbic structures in the brain (the left parahippocampal gyrus) in response to emotional stimuli.
Editor’s Note: These data add to the literature on the positive effects of 1–2 grams of omega-3 fatty acids in depression. Given the safety of omega-3 fatty acids and the ambiguous effects of antidepressants in bipolar depression, omega-3 fatty acids would appear to a good alternative, especially since the FDA-approved atypical antipsychotics (quetiapine and lurasidone) are not approved for bipolar depression in people under age 18.
ECT versus Drug Therapy for Bipolar Depression
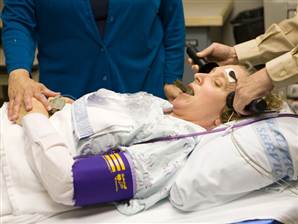 Electroconvulsive therapy is often considered a primary treatment option for patients with severe bipolar disorder that has resisted pharmacological treatment. Researcher Helle K. Schoeyen and colleagues recently published the first randomized controlled trial comparing ECT (in this case right unilateral brief pulse ECT) with algorithm-based pharmacological treatment in 76 patients with treatment-resistant bipolar depression.
Electroconvulsive therapy is often considered a primary treatment option for patients with severe bipolar disorder that has resisted pharmacological treatment. Researcher Helle K. Schoeyen and colleagues recently published the first randomized controlled trial comparing ECT (in this case right unilateral brief pulse ECT) with algorithm-based pharmacological treatment in 76 patients with treatment-resistant bipolar depression.
The response rate was significantly higher in the ECT group than in the patients who received drug treatment (73.9% versus 35.0%). However, the two treatment groups had similarly low remission rates (34.8% for ECT and 30.0% for pharmacological treatment).
The algorithm-based pharmacological treatment used in the study was based on a sequence of treatments endorsed by researchers Frederick K. Goodwin and Kay Redfield Jamison in their 2007 book Manic-Depressive Illness. A selected treatment was chosen for each participant based on his or her medical history. If the first treatment was ineffective or intolerable, the patient would be switched to the next treatment option. Antipsychotics, antidepressants, anxiety-reducing drugs, and hypnotics were some of the other treatments included in the algorithms.
Patients in the study had previously showed a lack of response to at least two different antidepressants and/or mood stabilizers with documented efficacy in bipolar disorder (lithium, lamotrigine, quetiapine, or olanzapine) in adequate doses for a period of 6 weeks (or until they quit because of side effects).
Editor’s Note: Even when ECT is effective, there is the issue of how to maintain that good response. We previously reported that in a 2013 study by Axel Nordenskjöld et al. in the Journal of ECT, intensive followup treatment with right unilateral brief pulse ECT combined with pharmacotherapy was more effective than pharmacology alone at preventing relapses. Patients who improved after an acute series of ECT (three times/week) then received weekly ECT for six weeks and every two weeks thereafter, totaling 29 ECT treatments in one year.
Other studies of more intermittent continuation ECT have not proved more effective than medication. Thus high intensity right unilateral brief pulse ECT is one option for extending the effects of successful ECT.
Atypical Antipsychotics in Bipolar Depression
A limited number of atypical antipsychotics are approved by the Federal Drug Administration for the treatment of depression in patients with bipolar disorder. This is important to note, because the widely used traditional antidepressants that are highly effective in unipolar depression are not effective in bipolar depression. Here we review the status of the only three approved drug treatments for bipolar depression (olanzapine, quetiapine, and lurasidone) and highlight data on a promising new atypical antipsychotic, cariprazine.
Lurasidone (Latuda)
At the 2014 meeting of the International College of Psychopharmacology, researcher Joseph Calabrese reviewed the efficacy of the latest atypical antipsychotic to receive FDA approval for bipolar depression, lurasidone. In monotherapy, both low (20–60mg/day) and high doses (80–120mg/day) showed higher response rates (53% and 51%, respectively) than placebo (30%). When added to either lithium or valproate, lurasidone response (57%) again exceeded that of placebo (42%). Calabrese also indicated that all of the other secondary outcome measures were also statistically significant, including score on the Clinical Global Impressions scale for bipolar disorder, time to response, percentage of remitters, time to remit, score on the Hamilton Anxiety scale, and a patient rated depression scale (QIDS).
Lurasidone is also approved for schizophrenia at higher doses (up to 160mg/day). At least twice as much of the drug is absorbed when food is in the stomach, so it is recommended that patients take it one to two hours after dinner or after a snack of 350 calories or more. The drug has an excellent side effects profile, as it is weight- and metabolically- neutral (i.e. it does not increase blood glucose, cholesterol, or triglycerides).
Quetiapine (Seroquel)
The atypical antipsychotic quetiapine has been FDA-approved for bipolar depression for a number of years. It consistently performs better than placebo in bipolar depression, and unlike lurasidone, quetiapine is also FDA-approved for mania, as well as for long-term prevention of both manic and depressive episodes as an adjunct to either lithium or valproate. Quetiapine is also superior to placebo for prevention of both manic and depressive episodes as a monotherapy, but is not FDA-approved for this indication. A good target dose for bipolar depression is 300mg/day of the extended release preparation taken several hours prior to bed time. Higher doses of 400 to 800mg/night are used for mania and schizophrenia. Quetiapine is also FDA-approved as an adjunct to antidepressants in unipolar depression. The drug has sedative side effects, perhaps because of its potent antihistamine effects. It can also increase weight, glucose, and cholesterol slightly more than placebo.
Olanzapine and Fluoxetine
Olanzapine (Zyprexa) and a combined preparation of olanzapine and fluoxetine (Symbyax) are also approved for bipolar depression, but many guidelines suggest that these be considered secondary treatments because they are associated with weight gain and adverse metabolic effects.
Cariprazine Effective in Bipolar Depression and Mania
At the 2014 meeting of the International College of Neuropsychopharmacology, researcher Suresh Durgam presented a poster on the first study of the atypical antipsychotic cariprazine in bipolar depression. There have also been three positive placebo-controlled studies of the drug in mania. It is a dopamine D2 and D3 partial agonist, with greater potency at the D3 receptor than the atypical antipsychotic aripiprazole (Abilify). In the large placebo-controlled eight-week study, doses of 1.5mg/day were superior to placebo, but higher (3mg) and lower doses (0.75mg) were not.
Another poster presented by the same research group also reported that augmentation of antidepressants with cariprazine in unipolar depression had results that were significantly better than placebo.
Editor’s Note: While all atypical antipsychotics that have been tested for mania have antimanic efficacy (lurasidone has not been studied in mania), their antidepressant profiles differ considerably. Only the three atypical antipsychotics noted above (olanzapine/fluoxetine, quetiapine, and lurasidone) are FDA-approved for bipolar depression, and in light of recent findings, cariprazine is likely to follow soon.
The atypical antipsychotics NOT approved for bipolar depression include: aripiprazole (Abilify), risperidone (Risperidol), and ziprasidone (Geodon), with the first atypical antipsychotic clozapine and the most recent ones not yet formally tested as far as this editor is aware, including asenapine (Saphris), iloperidone (Fanapt), and paliperidone (Invega).
Only the atypical antipsychotics aripiprazole and quetiapine are FDA-approved as adjunctive treatments to antidepressants in unipolar depression, and cariprazine may soon be added to this list.
Another promising open study of minocycline in bipolar depression
Joanna Soczynska in Roger McIntyre’s lab at the University of Toronto presented a poster at the 2014 meeting of the International College of Neuropsychopharmacology (CINP) on the anti-inflammatory and neuroprotective antibiotic minocycline.
Twenty-seven patients with a major depression received minocycline in addition to the medications they were already being prescribed. Dosage was 100mg twice a day. Treatment with adjunctive minocycline was associated with significant improvement on several scales that measure depression severity.
Editor’s Note: What was particularly interesting was that a subset of patients achieved complete remission, raising the question whether these patients might have markers of inflammation that would predict this excellent response. The authors concluded that the “results provide a rationale for testing minocycline’s efficacy in a larger randomized, placebo-controlled trial.”
Exactly this type of study was proposed a year ago by researcher Andy Nierenberg and given the best marks by a National Institute of Mental Health review committee but was turned down for funding because the National Institute of Mental Health has implemented a new initiative, Research Domain Criteria (RDoC), that lays out new criteria for research, limiting funding to those studies that focus on a molecular target that spans several diagnoses.)
Traditional Antidepressants Are Not Effective in Bipolar Depression
 Bipolar illness affects 4.5% of the US population. According to researcher Kathleen Merikangas, 1.0% have bipolar I disorder, 1.1% have bipolar II disorder, and the remainder have subthreshold symptoms. Mark Frye, Chairman of the Department of Psychiatry at the Mayo Clinic, gave a lecture on antidepressants in bipolar illness at the 2014 meeting of the American Psychiatric Association.
Bipolar illness affects 4.5% of the US population. According to researcher Kathleen Merikangas, 1.0% have bipolar I disorder, 1.1% have bipolar II disorder, and the remainder have subthreshold symptoms. Mark Frye, Chairman of the Department of Psychiatry at the Mayo Clinic, gave a lecture on antidepressants in bipolar illness at the 2014 meeting of the American Psychiatric Association.
The newest data from meta-analyses indicate that traditional antidepressants that are effective in unipolar depression are not effective in bipolar depression. Some patient groups, especially those with very early onset depression and mixed depression, are at increased risk of switching into mania and making a suicide attempt while taking antidepressants.
Unipolar depressed patients with a genetic variation that produces a short form of the serotonin transporter (5HT-LPRs/s) are at increased risk for depression in adulthood following a history of childhood adversity, and tend to respond less well to antidepressants. Frye found that 5HT-LPRs/s is weakly associated with switching into mania when antidepressants are given to patients with bipolar depression.
At the same symposium, researcher Mike Gitlin reviewed data on combination therapy, which is rapidly becoming the norm, indicating that in most circumstances, it is superior to monotherapy.
Researcher David Miklowitz reviewed the impressive data on the superiority of most forms of targeted psychotherapy or psychoeducation compared to treatment as usual for bipolar depression. He noted his own finding that Family Focused Therapy (FFT) not only is effective in adolescents and adults with bipolar disorder, but also in reducing illness and dysfunction in those with prodromal disorders (such as depression, cyclothymia, and bipolar not otherwise specified) in situations where there is a family history of bipolar disorder.
Eight components of FFT are:
- Recognition of prodromal symptoms and development of treatment strategies for them.
- Recognition and management of stress and triggers using cognitive restructuring.
- Development of a relapse prevention plan and rehearsal of what to do.
- Regularization of sleep.
- Encouragement of treatment adherence with an eye to a good future.
- Enhancement of emotional self-regulation skills, including cognitive restructuring.
- Improvement of family relationships and communication.
- Education about substance abuse avoidance and treatment for that and other comorbidities.
Many of these are also key components of group psychoeducation, cognitive-behavioral therapy, and interpersonal and social rhythms therapy, and all of these are effective in treating and preventing bipolar depression compared to treatment as usual. It is noteworthy that in the research of Francesc Colom, 90% of patients randomized to treatment as usual relapsed within 24 months, while psychoeducation was highly effective in preventing relapses over the next five years.
This editor (Robert M. Post), the discussant for the symposium, emphasized that the main take-away messages of the speakers were: use more lithium, use more caution and fewer antidepressants in treating bipolar depression, use more combination therapy for acute illness and for maintenance, and definitely use more psychotherapy. Read more
Psychotherapy More Effective Than Collaborative Care in Bipolar Depression with Anxiety Disorder Comorbidity
The Systematic Treatment Enhancement Program for Bipolar Disorder (STEP-BD), a long-term study of treatments for bipolar disorder, recently found that psychotherapy was more effective than their normal collaborative care model (consisting of regular illness evaluation and treatment) for patients with bipolar disorder and a current or lifetime presence of an anxiety disorder.
An anxiety disorder comorbidity is consistently associated with a poor outcome in patients with bipolar disorder. In a 2014 article by Deckersbach et al. in the American Journal of Psychiatry, the STEP-BD research group reported that the effect of psychotherapy was particularly strong in those with comorbid post-traumatic stress disorder (PTSD) or generalized anxiety disorder.
While antidepressants are typically used to treat anxiety disorders in unipolar depression, this has not been proven effective in bipolar disorder. Not only do patients with bipolar disorder tend to respond poorly to antidepressants, but in research collected by this editor Robert Post and colleagues in the Bipolar Collaborative Network, patients with bipolar disorder who had an anxiety disorder fared even more poorly on antidepressants as adjuncts to mood stabilizers than those with bipolar disorder without an accompanying anxiety disorder.
The poor response to antidepressants in bipolar depression in general, and particularly in those with a comorbid anxiety disorder, together with the finding that psychotherapy is highly effective, suggest that adjunctive psychotherapy is a more appropriate choice for patients with bipolar depression and a comorbid anxiety disorder.
The choice of the best pharmacological treatment of this comorbid anxiety disorder deserves specific comparative study. Candidates would include the mood stabilizing anticonvulsants valproate, lamotrigine, and carbamazepine; the atypical antipsychotics with efficacy in bipolar depression (quetiapine, lurasidone, and olanzapine combined with fluoxetine); and those used as an adjunct in unipolar depression (quetiapine again and aripiprazole).
Erythropoietin Improves Cognitive Function in Bipolar Depression
 Bipolar disorder is associated with cognitive dysfunction, and no definitive treatment has yet been found to reverse these problems with memory and attention. A new study by Kamilla W. Miskowiak presented at the 2014 meeting of the International Society of Bipolar Disorders explored the use of erythropoietin, a hormone that induces the production of red blood cells, as a treatment for cognitive dysfunction in bipolar disorder.
Bipolar disorder is associated with cognitive dysfunction, and no definitive treatment has yet been found to reverse these problems with memory and attention. A new study by Kamilla W. Miskowiak presented at the 2014 meeting of the International Society of Bipolar Disorders explored the use of erythropoietin, a hormone that induces the production of red blood cells, as a treatment for cognitive dysfunction in bipolar disorder.
Participants in the double-blind study were randomized to receive either eight weekly erythropoietin infusions (40,000 IU) or eight weekly saline infusions. While there was only a trend toward improvement in verbal memory, there were other statistically significant outcomes: erythropoietin improved sustained attention, recognition of happy faces, and speed of complex information processing across learning, attention, and executive function. These outcomes were not related to changes in reaction time or mood, and lasted as long as six weeks after the eighth erythropoietin infusion, by which time red blood cell production had normalized.
Methylene Blue Treats Bipolar Depression in Adults
Methylene blue is a chemical compound that has been used to treat a variety of medical conditions. This drug has some actions that resemble lithium’s: it inhibits guanylate cyclase, which generates second messenger cyclic GMP, and decreases nitric oxide. New evidence shows it may help depression and anxiety in bipolar disorder when added to lamotrigine.
In patients with bipolar disorder who were all treated with lamotrigine, an active 65mg dose of methylene blue three times per day (for a daily total of 195mg) versus 15mg/day (an inactive dose that produces the same side effect of blue urine) was more effective at treating depression and anxiety in a 12-week crossover study. Side effects, in addition to blue urine, included infrequent nausea, diarrhea, headache, and a burning sensation in the urinary tract. Of the 37 randomized study participants, 27 completed both phases of the entire six-month study. Martin Alda, a researcher who presented the double-blind randomized crossover data at the 2014 meeting of the International Society for Bipolar Disorders, indicated that he has also used this preparation clinically with success, although the pharmacy staff who prepared the capsules were not too happy, because everything the drug touches turns blue.








