Micronutrient Formulas Treat A Variety of Behavioral Disorders
At the 2015 meeting of the American Academy of Child and Adolescent Psychiatry, researcher Charles Popper reviewed the literature to date about broad-spectrum micro-nutrient treatments for psychiatric disorders in young people, concluding that these formulations of vitamins and minerals can reduce symptoms of aggressive and disordered conduct, attention deficit hyperactivity disorder, mood disorders, anxiety, and stress. Four randomized controlled trials showed that micronutrient formulas reduced violence and major misconduct in children.
Popper warned that while these micronutrients can be helpful in treating children who have never been prescribed psychiatric medication, they can interact dangerously with psychiatric medications in children who do take them.
At the same meeting, researcher Bonnie Kaplan reported that six randomized controlled trials of broad-spectrum micro-nutrients and B-complex vitamins in adults with and without psychiatric disorders showed that both of the formulas reduced anxiety and stress following natural disasters (which are associated with the development of post-traumatic stress disorder (PTSD)).
Family-Based Health Program Successful in Vermont
A statewide program to promote healthy behaviors within families has been successful in Vermont. The approach, described by researcher James J. Hudziak at the 2015 meeting of the American Academy of Child and Adolescent Psychiatry, is based on three assumptions. The first is that emotional and behavioral health is the cornerstone of all health. The second is that health behaviors are formed and sustained within families. The third is that promoting healthy behaviors, preventing illness, and intervening for better health outcomes are all important to enhancing the health of the population.
Vermont used community outreach (including town-hall public events), the media (including Twitter, blogs, radio, television, public service announcements, and a short film), and group trainings of community professionals to successfully spread health messages to families. The program targeted pediatricians’ offices, schools, community mental health centers, federally qualified health centers, and Departments of Health, Mental Health, and Child Welfare.
Hudziak has also suggested that programs of exercise, music, and mindfulness (all of which enhance brain growth and development) should be made universally available to children in school.
Children of Bipolar Parents in US More Ill than Those in the Netherlands
New research shows that bipolar disorder risk is higher in the US than in the Netherlands. At the 2015 meeting of the American Academy of Child and Adolescent Psychiatry, researchers Manon Hillegers and Esther Mesman described a study in which they compared the offspring of mothers with bipolar disorder in the US to those in the Netherlands. The offspring ranged in age from 10–18.
In the US, the mothers had, on average, an earlier age of onset, more substance abuse comorbidity, and were more likely to have been diagnosed with bipolar II disorder. Among the US offspring, 66% had been diagnosed with a psychiatric illness compared to 44% of the Dutch offspring. This included significantly higher rates of anxiety, ADHD, and disruptive behavior disorders in the US offspring. Among the offspring who had been diagnosed with a mood disorder, 80% of those in the US had other additional psychiatric disorders, but only 34% of the Dutch did. Bipolar disorder is more rare among children under the age of 12 in the Netherlands compared to the US.
Dutch children and adolescents were typically treated with lithium and with only one drug at a time. In the US, lithium is less widely used, and simultaneous treatment with several medications (usually including atypical antipsychotics) is common.
Editor’s Note: The research by Hillegers and Mesman replicates research by this editor (Robert M. Post) and colleagues that compared bipolar disorder incidence and severity in the US, Germany, and the Netherlands. Other comparisons have been made between the US and Europe. A 2014 article by Frank Bellivier and colleagues in the World Journal of Biological Psychiatry also showed that bipolar disorder onset occurs earlier in the US than in 10 different European countries, while Bruno Etain and colleagues found that bipolar disorder onset occurs earlier in the US than in France in a 2012 article in the Journal of Clinical Psychiatry.
Together this research shows that bipolar disorder is more serious in the US than in a number of European countries. Two-thirds of adults with bipolar disorder report that their illness began in childhood or adolescence. Most of these cases are not properly diagnosed or treated. A concerted effort must be made by the medical establishment and healthcare policymakers in the US to provide better and earlier treatment of bipolar illness.
Exercise Improves Cognition and Normalizes Brain Activity
Exercise isn’t just good for the body—new research suggests it can improve cognition and normalize brain activity.
At the 2015 meeting of the American Academy of Child and Adolescent Psychiatry, researcher Benjamin I. Goldstein reported that 20 minutes of vigorous exercise on a bike improved cognition and decreased hyperactivity in the medial prefrontal cortex in adolescents with and without bipolar disorder.
At the same meeting, researcher Danella M. Hafeman reported that offspring of parents with bipolar disorder who exercised more had lower levels of anxiety.
A plenary address by James J. Hudziak also suggested that exercise, practicing music, and mindfulness training all lead to improvements in brain function and should be an integral part of treatment for children at high risk for bipolar disorder and could be beneficial for all children.
Editor’s Note: Recognizing and responding to mood symptoms is key to the prevention and treatment of bipolar disorder in children and adolescents at high risk for the illness. For these young people, exercise, a nutritious diet, good sleep habits, and family psychoeducation about bipolar disorder symptoms may be a good place to start. Joining our Child Network may also be helpful.
Children at Risk for Bipolar Disorder May Have Adverse Reactions to Antidepressants
 At the 2015 meeting of the American Academy of Child and Adolescent Psychiatry, researcher Jeffrey R. Strawn reported that among children at high risk for bipolar disorder (because of a family history of the disorder) who are prescribed antidepressants for depression and anxiety, adverse reactions are common. These reactions include irritability, aggression, impulsivity, and hyperactivity, and often lead to discontinuation of the antidepressant treatment.
At the 2015 meeting of the American Academy of Child and Adolescent Psychiatry, researcher Jeffrey R. Strawn reported that among children at high risk for bipolar disorder (because of a family history of the disorder) who are prescribed antidepressants for depression and anxiety, adverse reactions are common. These reactions include irritability, aggression, impulsivity, and hyperactivity, and often lead to discontinuation of the antidepressant treatment.
Younger patients at risk for bipolar disorder were more likely to have an adverse reaction to antidepressants. Risk of an adverse reaction decreased 27% with each year of age.
Topiramate Added to Quetiapine Can Reduce Marijuana Craving in Young People
At the 2015 meeting of the American Academy of Child and Adolescent Psychiatry, researcher Melissa P. DelBello reported that compared to placebo, the anticonvulsant topiramate reduced marijuana craving in young people aged 12–21 who were already taking the antipsychotic quetiapine. Functional magnetic resonance imaging (fMRI) revealed that topiramate altered the activation of brain regions common to both drug craving and mood dysregulation. Topiramate could be a good treatment to reduce marijuana abuse. The antioxidant n-acetylcysteine (NAC) is another option.
RTMS Improves Executive Function in Kids with Schizophrenia and Autism
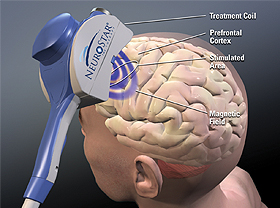 Researcher Stephanie Ameis reported at the 2015 meeting of the American Academy of Child and Adolescent Psychiatry that following repeated transcranial magnetic stimulation (rTMS), a treatment in which a magnetic coil placed over the scalp delivers electric pulses to the brain, children with schizophrenia and autism spectrum disorders showed improvements in executive function, including working memory. The rTMS treatment targeted the left dorsolateral prefrontal cortex.
Researcher Stephanie Ameis reported at the 2015 meeting of the American Academy of Child and Adolescent Psychiatry that following repeated transcranial magnetic stimulation (rTMS), a treatment in which a magnetic coil placed over the scalp delivers electric pulses to the brain, children with schizophrenia and autism spectrum disorders showed improvements in executive function, including working memory. The rTMS treatment targeted the left dorsolateral prefrontal cortex.
Offspring of Bipolar Parents at High Risk for Psychiatric Disorders
Researcher Juan David Palacio reported at the 2015 meeting of the American Academy of Child and Adolescent Psychiatry that compared to offspring of non-ill parents, children of parents with bipolar I disorder are at high risk for psychiatric disorders, particularly bipolar spectrum disorders and substance use disorders. They were also at risk for symptoms of anxiety disorders and conduct disorder. Palacio’s findings from Colombia mirror those from other studies of familial risk and suggest the importance of vigilance to detect these disorders early and provide appropriate treatment. Our Child Network may help.
Dopamine Partial Agonists: An Overview
 Several atypical antipsychotic drugs are partial agonists of dopamine. They provide weak stimulation of dopamine receptors in the brain and prevent dopamine from overstimulating the receptors by binding to them in its place.
Several atypical antipsychotic drugs are partial agonists of dopamine. They provide weak stimulation of dopamine receptors in the brain and prevent dopamine from overstimulating the receptors by binding to them in its place.
In contrast, most antipsychotic and antimanic drugs are dopamine antagonists, which also bind to dopamine receptors but prevent any stimulation from occurring there.
A. Aripiprazole (Abilify) was the first partial dopamine agonist approved by the Food and Drug Administration for the treatment of schizophrenia, and mania, and as an add-on treatment to antidepressants for the treatment of unipolar depression, but not bipolar depression.
B. Brexpiprazole (Rexulti) received FDA approval for the treatment of schizophrenia and as an add-on treatment to antidepressants for the treatment of unipolar depression in 2015. It is similar to aripiprazole but has weaker activity at the dopamine D2 receptor. Brexpiprazole is associated with small increases in the hormone prolactin, as opposed to the small decreases in prolactin seen with aripiprazole.
C. Cariprazine (Vraylar) is FDA-approved for schizophrenia and mania, and it also has positive placebo-controlled data in bipolar depression and as an adjunct to antidepressants in unipolar depression. It differs from the others in that it is more potent at dopamine D3 receptors than at D2 receptors. It is thought that effects on D3 receptors may provide better antidepressant effects, but this proposition has not yet been tested.
New Drug Cariprazine Approved for Schizophrenia and Bipolar Disorder
 In late 2015, the Food and Drug Administration approved the new atypical antipsychotic drug cariprazine for the treatment of schizophrenia and mania in adults. The approval followed a series of clinical trials that showed that the drug reduced symptoms of each illness compared to placebo.
In late 2015, the Food and Drug Administration approved the new atypical antipsychotic drug cariprazine for the treatment of schizophrenia and mania in adults. The approval followed a series of clinical trials that showed that the drug reduced symptoms of each illness compared to placebo.
The most common side effects of cariprazine reported in the trials included tremor, slurred speech, and involuntary muscle movements.







