Uric Acid Increases During Mania
At the 65th Annual Scientific Convention of the Society of Biological Psychiatry this year, Giacomo Salvadore reported that significantly higher levels of uric acid are found in patients with mania compared with normal controls.
Editor’s note: This study was particularly interesting because there was a highly significant difference between patients and controls, with very few values overlapping. The data suggest the possibility that uric acid may be a useful biological marker for mania, and is one that should be studied in childhood-onset bipolar illness to determine whether uric acid is a marker for mania in children as well.
Allopurinol, a widely used treatment for gout that reduces levels of uric acid in the blood, is an effective antimanic agent (based on data from two placebo-controlled studies, one by Machado-Vieira et al. and one by Akhondzadeh et al.). The new data on uric acid raise the possibility that high levels of uric acid may be a specific predictor of responsiveness to Allopurinol, although this hypothesis has not yet been explored.
In an article by Chung et al. just published in Psychiatry Research, it was reported that in a very large epidemiological study in Taiwan, patients with bipolar disorder have increased risk of gout.
Treatment Guidelines for Two Hypothetical Cases in Children
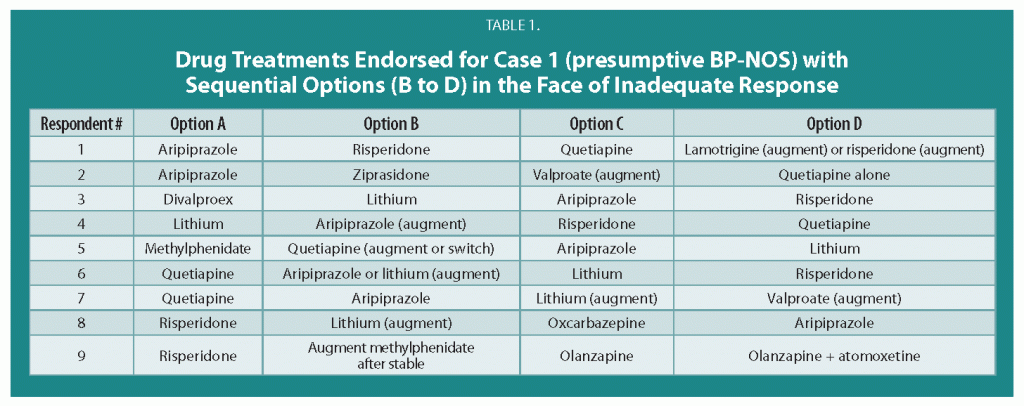
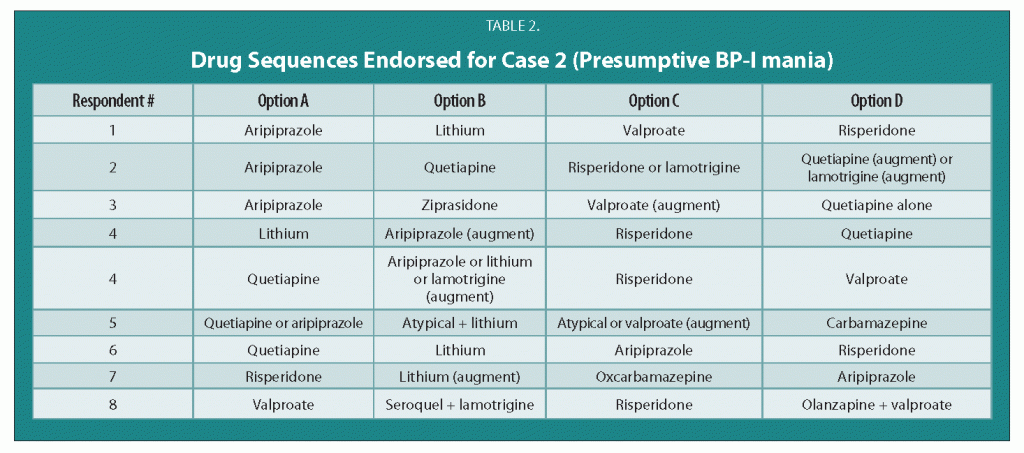
There are no FDA-approved treatments for children under age 10 with bipolar disorder. For an article in Psychiatric Annals, this editor and Janet Wozniak asked experts how they would sequence treatment of a hypothetical case of a 6-year-old with extreme mood instability consistent with a diagnosis of BP -NOS (see Table I). We also asked how the experts would treat a different case of a 9-year-old with a full-blown psychotic BP-I mania (see Table II).
The results are presented and discussed in detail in the article, and are presented here to reinforce several points. The recommendations for children under 10 and for BP NOS are highly similar to consensus guidelines for older BP I children compiled by Kowatch et al.
Treatments in the face of non-response to option A or others are sequenced differently by different experts, but almost always involve an atypical antipsychotic (AA) or a mood stabilizer (MS) such as lithium, valproate, carbamazepine/oxcarbazepine, or rarely, lamotrigine. Revisions of atypical antipsychotics and mood stabilizers and use of combinations are the common next strategies.
Oxcarbazepine May Be Helpful In Pediatric Mania
Oxcarbazepine (OXC; Trileptal) is a close structural relative of carbamazepine (CBZ; Tegretol; Equetro), but unlike CBZ, OXC is not an enzyme inducer, nor does it have CBZ’s risks of rare agranulocytosis or aplastic anemia.
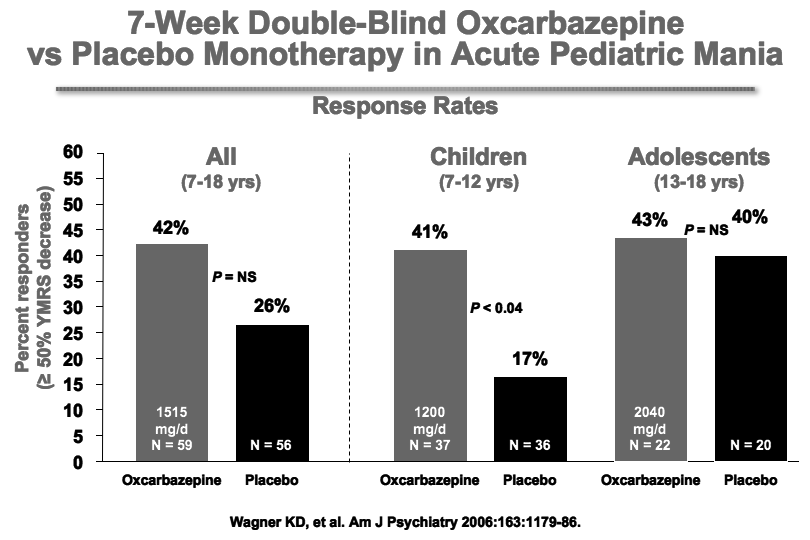
Wagner et al.’s report on OXC in the American Journal of Psychiatry in 2006 is typically cited as evidence the drug is ineffective for pediatric mania. But observe the figure:
While this was true of OXC’s efficacy in adolescents (due to a large placebo response—see rightmost column), OXC worked significantly better than placebo in children ages 7-12. These younger children often have more chronic presentations and BP-NOS. This may explain the low placebo response rate in the younger children.
Oxcarbazepine is considered helpful by many clinicians (See Post and Wozniak’s survey of expert treatment approaches to childhood illness, published in Psychiatric Annals in 2009) and should not be dismissed altogether.
Quetiapine is Effective Across a Spectrum of Illnesses
The atypical antipsychotic quetiapine (Seroquel or Seroquel XR) has a range of efficacy in a number of illnesses, depending on the size of the dose given. Read about some of its uses below, including as an adjunct to antidepressants in unipolar depression; as a treatment for generalized anxiety disorder (GAD) and post-traumatic stress disorder (PTSD); and, at higher doses, as a treatment for mania and depression. Some of its potential mechanisms of action are described as well.
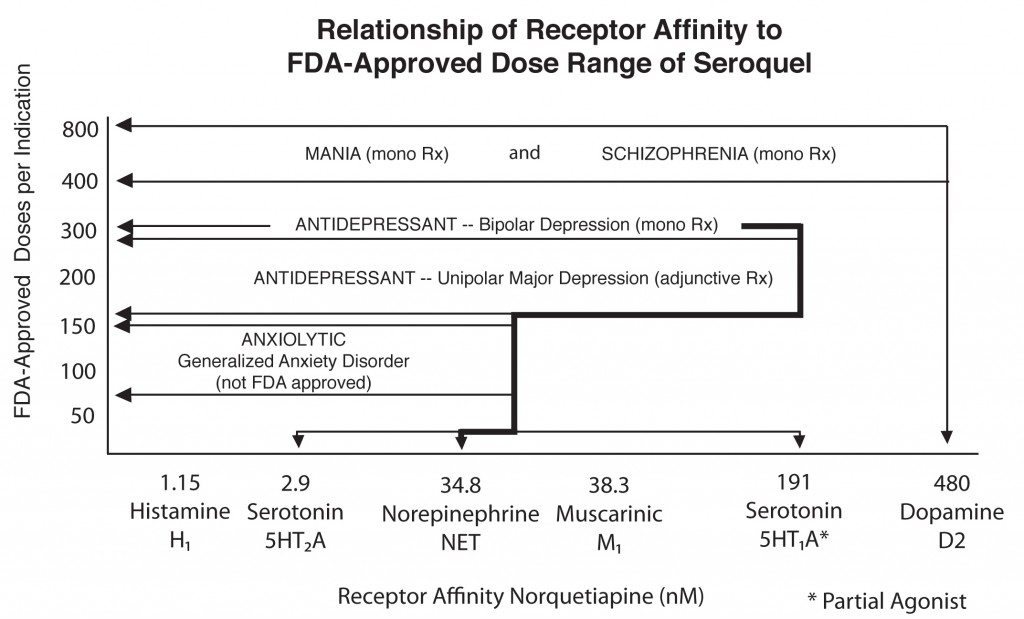
Quetiapine's actions on various receptors in the brain (bottom axis) are responsible for its effects in different illnesses
Quetiapine as an adjunct to antidepressants in unipolar depression
Posters at the American Psychiatric Association meeting in San Francisco in May 2009 showed new data from a series of studies of quetiapine in unipolar depression that showed the drug in monotherapy (at 150mg & 300mg) was significantly more effective than placebo. Studies were also positive when quetiapine was used as an adjunct compared with placebo for patients showing inadequate or incomplete responses to antidepressants such as selective serotonin reuptake inhibitors (SSRIs).
Read more
Lamotrigine plus Valproate: Better than Lamotrigine Alone for Bipolar Depression
In a study comparing valproate monotherapy with the combination of lamotrigine and divalproex (Valproate) extended release (ER), the combination appeared more effective in bipolar depression. At the American College of Neuropsychopharmacology meeting in December 2009, Vivek Singh, Charles Bowen, Richard Weisler, and colleagues from The University of California, San Diego reported on the randomized, double-blind, eight-month maintenance study of bipolar depressed patients.
Patients who could be stabilized for two consecutive weeks on the combination treatment of both lamotrigine and divalproex were then randomized to either lamotrigine alone or the combination for the duration of the study. Most of the data collected about these 87 subjects favored the treatment with the combination (lamotrigine plus divalproex) compared with lamotrigine alone. Combination therapy was superior for manic symptomatology and resulted in lower rates of unanticipated worsening of depression (greater than 20 points on the Montgomery-Asberg depression rating scale (MADRS)) that led to termination from the study than lamotrigine monotherapy did.
Read more