Lamotrigine for Bipolar Disorder in Kids
Dr. Gagin Joshi of Massachusetts General Hospital reported the results of a study using lamotrigine (Lamictal) for 12 weeks in 39 children with bipolar disorder. Average dose was 160 mg/day and was titrated very slowly because of the increased risk of rash in children treated with lamotrigine compared with adults. Thirty-eight percent of the children achieved remission in mania, and 42% in depression.
In terms of side effects, 28% of individuals experienced gastrointestinal upset; 26% headache, 18% allergy, and 18% dermatological problems which led seven patients to discontinue the trial. However, none of the rashes were severe. This article is to be published in the journal CNS Science and Therapeutics this year.
One Expert’s Personal Treatment Algorithm for Bipolar Disorder in Young Children
EDITOR’S NOTE: Dr. Gagin Joshi of Massachusetts General Hospital, who presented the work on carbamazepine and lamotrigine on page 1 provided us with his own general treatment algorithm for youngsters with bipolar disorder.

Omega-3 Fatty Acids (photo from ironmagazine.com)
Joshi typically starts with 0.5 to 2 gms of omega-3 fatty acids because of their benign side-effects profile, the many studies suggesting they are effective in adult mood disorders, and a recent article indicating that they were effective in preventing the conversion of prodromal schizophrenia into full-blown illness in a randomized double-blind controlled study in Australia.
After the omega-3 fatty acids, Joshi’s second choice is typically the atypical antipsychotic aripiprazole (Abilify) because of its lesser degree of weight gain compared to atypicals quetiapine (Seroquel) or risperidone (Risperidol). Risperidone can be a third option if aripiprazole is not effective or tolerated.
Vitamins for Treatment-Resistant Childhood Bipolar Disorder?

Update (11/1/2010): According to Dr. Charles Popper of Massachusetts General Hospital and McLean Hospital, particular caution should be used when considering the combination of EMPowerplus with psychopharmacological medications. When used alone, the vitamin compound appears to be relatively safe. However, in combination with other drugs, Empowerplus appears to enhance the medications’ effects, both positive and adverse. So use of very low doses of the vitamin compound with gradual increases should be combined with appropriate decreases in doses of other medications.
Researcher Mary Fristad from Ohio State University completed a small, uncontrolled study of a novel treatment approach, the multi-vitamin and mineral preparation labeled EMPowerplus. Initial case reports from other researchers indicated that the compound led to remarkable and sustained effectiveness in children with bipolar disorder who were unresponsive to most other psychopharmacological approaches.
Fristad’s open study included ten children. Participants were slowly titrated to a minimum of 12 capsules/day with a maximum of 15 capsules/day.
Fristad and colleagues saw 37% improvement in depression and 45% improvement in mania in the entire group of patients who began treatment, while in those who completed the study, there was 71% improvement in depression and 58% improvement in mania. Side effects were benign, but the preparation needs to be administered judiciously in conjunction with a physician’s supervision.
Dr. Fristad hopes to conduct further double-blind, placebo-controlled trials of this compound, which also showed promising open results in case studies by Kaplan et al. in 2002 and 2004 and was written about by Charles Popper, a researcher at Massachusetts General Hospital, in 2001.
The EMPowerplus preparation is available at the web site http://truehope.com and costs approximately $100-200 per month, but is not recommended for use without careful supervision by a physician.
EDITOR’S NOTE: Controlled clinical trials to demonstrate efficacy have not yet been undertaken, partly due to lack of support from funding organizations and uncertainty about which of the many ingredients is active. Studies of pharmaceutical agents for treatment-resistant children without a cogent theoretical rationale are rarely a high priority despite the great need for effective treatment approaches.
Nonetheless, given initial promising results of the Fristad group and others, systematic clinical trials of this preparation are now clearly indicated.
Inflammation in the Affective Disorders
Bipolar children exhibit more inflammation than healthy children, according to a paper presented by Pandey, Dwivedi, and Pavuluri from the University of Illinois at the American College of Neuropsychopharmacology in December 2009.
In “Pro-inflammatory cytokines in plasma of patients with pediatric bipolar disorder,” the researchers described their study in which 21 normal controls were compared with 22 children with pediatric bipolar disorder who were unmedicated for a period of at least two weeks. The level of the inflammatory cytokine interleukin-1b (IL-1b) was significantly higher in the pediatric bipolar patients compared with controls, and levels of TNF alpha, another inflammatory marker, were significantly higher as well. Not only is this evidence of increased inflammatory processes in pediatric bipolar disorder, but TNF alpha is associated with activation of transcription factors and the initiation of preprogrammed cell death, or apoptosis.
Persistence of Mild Depression Is Risk Factor for Relapse into Full-Blown Episodes
In naturalistically treated bipolar patients, depression is three times more prevalent than manic symptoms (according to studies by Judd et al., Kupka et al., and Ezquiaga et al.). The occurrence of even residual depression or subsyndromal symptoms can be highly impairing, and is a predictor of increased likelihood for subsequent relapse, according to a poster presented by Gitlin et al. at the American Psychiatric Association meeting in San Francisco in May 2009.
These new data support that of a large number of other investigators who have made similar observations, all indicating the importance of attempting to achieve full remission as a major goal of clinical therapeutics in order to decrease likelihood of relapse. Gitlin’s study further indicated that impairment of quality of life in bipolar patients was closely related to the degree of their subsyndromal symptomatology.
Aripiprazole (Abilify), the Atypical Atypical Antipsychotic
This is an overview of the drug aripiprazole.
Spectrum of Efficacy
Aripiprazole has now been approved for acute and maintenance treatment of pediatric patients with bipolar disorder from ages 10 to 17. It had already been approved for adult bipolar disorder, schizophrenia, and as an adjunctive treatment for acute unipolar depression inadequately responsive to antidepressants of the serotonin-selective class or the serotonin-norepinephrine reuptake inhibitor venlafaxine. Aripiprazole, along with risperidone, is one of only two drugs FDA-approved for the treatment of irritability in autism.
Read more
Reconsidering Ziprasidone (Geodon) for Kids with Bipolar Disorder
Ziprasidone has shown efficacy in pediatric BP I disorder (ages 10 to 17). Its metabolic profile is the most benign of the atypical antipsychotics, including being the only one that does not produce weight gain in children. None of the other metabolic indices increased either.
This drug is currently rarely used in children because of concerns about its effects on electrocardiogram (EKG), which have rarely been seen in clinical practice. Perhaps the overall assessment of its risk/benefit ratio should be re-evaluated.
We’ve posted before about ziprasidone’s benign side effects profile.
Lamotrigine plus Valproate: Better than Lamotrigine Alone for Bipolar Depression
In a study comparing valproate monotherapy with the combination of lamotrigine and divalproex (Valproate) extended release (ER), the combination appeared more effective in bipolar depression. At the American College of Neuropsychopharmacology meeting in December 2009, Vivek Singh, Charles Bowen, Richard Weisler, and colleagues from The University of California, San Diego reported on the randomized, double-blind, eight-month maintenance study of bipolar depressed patients.
Patients who could be stabilized for two consecutive weeks on the combination treatment of both lamotrigine and divalproex were then randomized to either lamotrigine alone or the combination for the duration of the study. Most of the data collected about these 87 subjects favored the treatment with the combination (lamotrigine plus divalproex) compared with lamotrigine alone. Combination therapy was superior for manic symptomatology and resulted in lower rates of unanticipated worsening of depression (greater than 20 points on the Montgomery-Asberg depression rating scale (MADRS)) that led to termination from the study than lamotrigine monotherapy did.
Read more
The N-acetylcysteine Story: A New Potential Therapy for Bipolar Illness and Substance Abuse
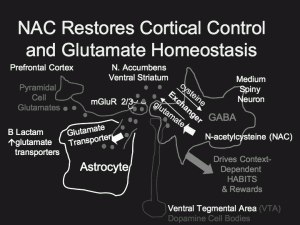
N-acetylcysteine (NAC), a readily available substance from health food stores, is able to reestablish glutamate homeostasis (regulation and balance) in the reward area of brain (the nucleus accumbens), reported Peter Kalivas of the University of South Carolina at the “Staging neuropsychiatric disorders: Implications for idiopathogenesis and treatment” meeting in Mojacar, Spain this past November. Kalivas reported that NAC appears to be effective across a spectrum of addictions, including cocaine, heroin, alcohol, cigarette smoking, and gambling.
Even more remarkably, NAC also appears to have positive effects in placebo-controlled studies in the treatment of patients with bipolar illness, report Mike Berk and colleagues, who are studying the same substance in Australia. Compared with placebo, patients taking adjunctive NAC showed improvement in all outcome measures, especially depression, after 3 and 6 months. In another article, also published in Biological Psychiatry in 2008, Berk’s research group demonstrated that NAC improved some negative symptoms of schizophrenia. NAC has also shown positive effects in trichotillomania and on nail-biting, suggesting that it has a variety of potential clinical uses in conditions associated with pathological compulsive behavioral patterns.
More Medical Comorbidities Among Bipolar Population
Goldstein and colleagues interpreted data from the National Epidemiological Survey in 2001-2002 that included 41,682 representative adults in the U.S. population sampled compared with 1,411 found in the community with a diagnosis of bipolar disorder.
Those with bipolar disorder had a 3.86 times higher odds of having coronary heart disease compared with those in the general population. They were also 2.15 times more likely to have hypertension. Most disturbingly, the mean age of those with coronary heart disease in the general population was 62.1 years of age, but in those with bipolar illness, it was 50.4 years of age. This indicates that the markedly increased risk and incidence of coronary artery disease occurred approximately 11 years earlier in those with bipolar illness compared with those without. Most interestingly, the number of prior depressive episodes correlated with the presence of either coronary heart disease or hypertension.