Red Meat Interacts with Bacteria in the Gut to Raise Heart Disease Risk
 A 2018 study by a group of researchers at the Cleveland Clinic have clarified the way that a diet heavy in red meat may lead to heart disease. The research centers on trimethylamine N-oxide (TMAO), a gut bacteria byproduct that is formed during digestion. When gut bacteria digest choline, lecithin, and carnitine, nutrients that are common in certain animal products and red meat, TMAO is produced.
A 2018 study by a group of researchers at the Cleveland Clinic have clarified the way that a diet heavy in red meat may lead to heart disease. The research centers on trimethylamine N-oxide (TMAO), a gut bacteria byproduct that is formed during digestion. When gut bacteria digest choline, lecithin, and carnitine, nutrients that are common in certain animal products and red meat, TMAO is produced.
In an article by Robert A. Koeth and colleagues in the European Heart Journal, the researchers show that diets that rely on red meat as the main protein source lead to more circulating TMAO than diets in which white meat or something other than meat is the primary source of protein. They found that in people who eat a lot of red meat, the kidneys are less efficient at expelling TMAO, and levels creep even higher. High levels of TMAO have been linked to hardening and narrowing of the arteries (atherosclerosis) and heart disease complications. High levels of TMAO in the blood can be a predictor of heart attack, stroke, and death.
The study of 113 participants consisted of three different diets that each participant followed in random order (with a washout period in between each diet). A month of eating a diet in which red meat was responsible for at least 25% of participants’ daily calories led to higher levels of TMAO in the blood and urine. TMAO increased threefold during the red meat diet periods compared to periods in which white meat or non-meat protein were the source of those calories, and in certain participants, TMAO increased as much as tenfold. When participants stopped eating the red meat diet, their TMAO levels fell over the following month.
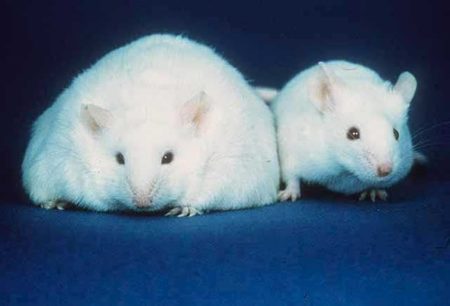
Rich Western Diet Reprograms Immune Cells in Mice
A 2018 article by Anette Christ and colleagues in the journal Cell describes the process by which a Western diet can trigger changes to the immune system in mice. The mice fed a calorically rich Western diet started to show systemic inflammation. Blood measures of inflammation returned to normal after the mice resumed their regular diet, but their immune responses remained heightened, as if the immune system had been trained to overreact.
The vast majority of deaths in Western cultures are caused by noncommunicable diseases such as type 2 diabetes and cardiovascular disease, which have been linked to lifestyle factors such as diet and exercise. The immune system has two wings: one that responds to specific pathogens, and one that mounts general protection against infection and is triggered by immune signaling receptors. However, according to Christ and colleagues, in addition to reacting when microbes are present, this second wing may also respond to “sterile” danger signs, such as consumption of a Western diet. The immune system may become trained to react this way chronically, something that the researchers believe may trigger inflammation in noncommunicable diseases.
The Western diet triggered epigenetic changes to the mice’s immune system. Epigenetic changes are ones that affect the structure of DNA, for example how tightly it is packaged. In the case of the Western diet, these changes resulted in a heightened immune system that launched strong inflammatory responses in reaction to even small stimuli. Myeloid cells from bone marrow were reprogrammed to proliferate and provide a stronger immune response.
The researchers also took human monocyte cells trained with LDL (“bad”) cholesterol and stimulated them with lipopolysaccharide (an inflammatory compound made of fat and sugar). The cells showed a heightened immune reaction similar to that seen in the mice.
Mice genetically engineered to lack the inflammasome NLRP3, which activates inflammatory responses, did not show the systemic inflammation or the enhanced myeloid activity when fed the Western diet, so Christ and colleagues believe NLRP3 may play an important role in mediating the immune response to the Western diet.
In Animals, Exposure to High Fat Diet During Pregnancy Can Affect Offspring’s Neurological Development
New research in non-human primates suggests that exposure to a high fat diet during pregnancy and in early development prior to weaning can increase the offspring’s propensity for anxiety later in life.
The new research echoes 2010 findings about rats. Researcher Staci D. Bilbo and colleagues reported in the journal of the Federation of American Societies for Experimental Biology that in rats, a high fat diet during pregnancy and lactation led to offspring with greater body weight, increased inflammation, and problems with anxiety and spatial learning. Switching to a standard diet after weaning did not eliminate these outcomes.
The recent research by Jacqueline R. Thompson and colleagues, published in the journal Frontiers in Endocrinology in July 2017, suggests that maternal nutrition in the primate during pregnancy and lactation can have long-lasting effects on offspring’s neurological development, altering the brain and endocrine system. These changes occurred even if the offspring began a normal diet after weaning.
65 female Japanese macaques were divided into two groups, one that received a high-fat diet and one that received a normal diet. In the offspring of mothers who ate a high-fat diet, the researchers found impaired development of neurons containing serotonin. The offspring of the high-fat diet group also showed behavioral alterations such as increased anxiety.
The high rates of obesity in the US and other developed nations make these findings particularly important. The researchers suggest that 64% of women in the US who are of reproductive age are overweight, and 35% are obese. Co-author Elinor Sullivan suggested that the findings from the study could motivate mothers to make healthy nutritional decisions, not only for themselves but for their children as well.
Vegan Diet Can Lead to Vitamin B12 Deficiency
Vitamin B12 deficiency is a risk associated with a vegan diet. B12 deficiency can lead to depression, anemia, and even irreversible neuron damage, according to researcher Drew Ramsey, who spoke on the topic at the 2016 meeting of the American Psychiatric Association.
A study of vegans showed that 52% were deficient in vitamin B12, while another 23% had insufficient levels of the vitamin. B12 is found in the highest concentrations in certain seafoods and liver. It is also found in dairy products, eggs, fortified breakfast cereals, and is available in supplement form.
Women who eat a vegan diet while pregnant may not be providing their offspring with enough nutrients, according to researcher Emily Deans, who also spoke at the meeting. A case report on 30 vegan mothers found that 60% of their offspring had developmental delays and 37% showed cerebral atrophy.
Deans said that eating no meat is associated with higher rates of depression, anxiety, and worse quality of life.
Ramsey believes that while the North American diet is probably weighted too heavily toward animal products, seafood remains an important source of B12.
Eat More Plants for Health
A long-term study of 130,000 nurses and other health professionals found that eating more plants lowered risk of death over several decades. A 3% increase in calories from plant protein was associated with a 10% lower risk of death during the study period.
The research, by Mingyang Song and colleagues in the journal JAMA Internal Medicine, found that the more animal protein consumed, the higher the risk of death from cardiovascular disease during the study. A 10% increase in the proportion of calories from animal protein was associated with a 2% increase in deaths. This association was worse for people who were obese or heavy drinkers.
Song and colleagues suggest that plants are a better source of calories than are animal products, and that fish or chicken are better choices than processed red meat.
Researcher Dariush Mozaffarian recommends eating plant-based foods like fruits, nuts, seeds, beans, and non-starchy vegetables, but avoiding those like French fries or white bread that have little nutritional value.
Benefits of a Healthy Lifestyle
 In a talk at the 2015 meeting of the International Society for Bipolar Disorder, researcher Michael Berk suggested that a healthy lifestyle may improve mood disorder symptoms.
In a talk at the 2015 meeting of the International Society for Bipolar Disorder, researcher Michael Berk suggested that a healthy lifestyle may improve mood disorder symptoms.
Diet is important. A study of more than 20,000 mothers revealed that those with unhealthy diets had children with more externalizing disorders, such as attention deficit hyperactivity disorder (ADHD), oppositional defiant disorder, and mania. Diets high in fat and sugar were linked to depression. The Nurses’ Health Study, a long-term epidemiological study of 50,000 women, showed that people who exercised more were less likely to be depressed, while lower muscle mass was associated with greater depression. Exercise also has anti-inflammatory effects.
Avoiding smoking has benefits, too. A study by Pasco and colleagues showed that people who smoke are at increased risk for a new onset of a mood disorder. Smoking is associated with onset of a more severe mood disorder earlier in life, suicide attempts, alcohol and substance abuse, and decreased response to treatment. Fortunately, quitting smoking can reverse some of these risks.
Digestion of Wheat and Milk Releases Peptides that Might Cause Inflammation
Some people have found that gluten-free or casein-free diets have improved their intestinal, autoimmune, or neurological symptoms. (Casein is a protein found in mammals’ milk. Cow milk is high in casein while human milk proteins are 20–45% casein.) One explanation for the good effects of these diets is that peptides that are released during digestion of these foods can create epigenetic changes in gene expression, adding methyl groups to DNA strands that increase inflammation.
As infants transition from getting all of their nutrition from the placenta to using their gastrointestinal tract, their diet may lead to epigenetic modifications that affect their health later in life. Epigenetics refers to changes in genes that do not affect the inherited sequence of DNA, but affect how easily the DNA is transcribed to produce proteins. Methyl or acetyl groups can be added to DNA or the histones around which it is wound.
When a person digests casein (from either human or animal milk) or gliaden (a protein derived from wheat), peptides are released that activate opioid receptors, modulating the uptake of the amino acid cysteine in neurons and in the gastrointestinal tract. This decrease in cysteine uptake is associated with drop in the antioxidant glutathione and a methyl donor (a molecule with a reactive methyl group that can easily become part of another molecule) called S-Adenosyl methionine.
In addition to decreasing cysteine uptake, the peptides also increase DNA methylation and create epigenetic changes in genes involved in redox (changes in oxidation) and methylation homeostasis.
These processes are described in a 2014 article by Malav S.Trivedi et al. in the Journal of Nutritional Biology. Trivedi et al. conclude that milk and wheat can change antioxidant activity and gene expression. Differences in the peptides in human and cow milk may explain developmental differences between children who are breastfed and those who receive formula.
The decrease in antioxidants caused by peptides from wheat and milk can predispose people to inflammation and oxidation, explaining why wheat- or casein-free diets might be useful.
Information from Environmental Experiences Can Be Passed on in Dad’s Sperm
Contrary to all common sense, researcher Brian Dias showed that when rats that were future fathers learned to associate an odor with a shock, this learning could be passed on to the next generation when the father mated with a female rat that had not learned the same association.
It turns out that the next generation of rat pups shows increased behavioral reactivity to the odor in a process different from the fear conditioning they might exhibit if they learned to avoid the odor through their own experiences.
Presumably, the pup is somehow programmed through an epigenetic modification of the father’s sperm to grow more neurons from the nose to the olfactory bulb that specifically react to the odor its father feared, and not to other odors. Miraculously, when the second generation pup grows up and fathers a third generation pup, the new pup also shows increased behavioral sensitivity to that specific odor. How the odor information from the first generation is represented in the fathers’ sperm and passed on to their descendants is still a complete mystery.
There are also new data that a father rat fed a diet deficient in folic acid (vitamin B9) will sire offspring with more congenital malformations. Additionally, an obese father rat fed a diet that includes extra fat calories will sire pups that become obese as adults even when fed a normal milk diet from a svelte mother before weaning and then fed a normal diet after weaning.
Mothers’ behavior usually gets most of the credit and/or blame for her children’s behavior, but now it looks like fathers’ diet or behavior (even before they have children) may have lasting consequences for their offspring.
Trans-Fats Linked to Depression Risk
 Research published last year showed that people with diets that contain high amounts of trans-fats are at greater risk for depression than people with diets higher in monounsaturated fatty acids (MUFAs) and polyunsaturated fatty acids (PUFAs).
Research published last year showed that people with diets that contain high amounts of trans-fats are at greater risk for depression than people with diets higher in monounsaturated fatty acids (MUFAs) and polyunsaturated fatty acids (PUFAs).
Medscape Medical News reported some tips from lead author of the study, Almudena Sánchez-Villegas, PhD: “The results were not surprising [and] I think the message is clear: ‘try to eat healthy.'”
“Avoid some types of fats, such as trans and saturated fatty acids, and increase the intake of polyunsaturated and monounsaturated fat; it’s better to consume olive oil than margarine or butter, better to use low-fat dairy than high-fat dairy, and better to eat fish than to consume meat or meat products; avoid fast and processed foods and commercial bakery; and try to increase your consumption of fruits, vegetables, and nuts,” she said.
We’ve written before about diet.
Diet, Depression, Inflammation and the Brain
We’ve been posting recently about diet and about treatments that are weight-neutral. There is evidence that diet, inflammation and depression are all linked. Epidemiological studies by Joe Hiblen have shown that in countries whose populations eat more fish and thus have high levels of omega-3 fatty acids in their diet, there is lower incidence of depression, suicide, and cardiovascular disease such as heart attacks and strokes. This may be because the major omega-3 fatty acids, EPA and DHA, are anti-inflammatory, and inflammation has been linked to depression. EPA inhibits the enzymes phospholipase A2 and cyclo-oxygenase-2 (COX-2), and their subsequent inflammatory effects on cytokines. DHA inhibits the pro-inflammatory cytokine IL6.
Researcher John Davis recently reviewed relevant literature and found that diets high in anti-inflammatory omega-3 fatty acids are associated with lower incidence of depression, cardiovascular disease, and markers of inflammatory processes. Conversely, diets high in fat and in inflammatory omega-6 fatty acids are associated with obesity, depression, and cardiovascular disease.
Various studies have shown the links between inflammation and depression. For example, when patients are given alpha-interferon to treat viral hepatitis, there is a subsequent increase in inflammatory cytokines IL-1 and IL-6, and depression often follows. Also, depressed patients have an increased ratio of pro-inflammatory to anti-inflammatory cytokines in their blood.
Another sign of a link between bipolar illness and inflammation can be seen in biochemical analysis of brain specimens obtained at autopsy. Researcher Rapaka Rao in the laboratory of Stanley Rapoport at the National Institute on Aging at the National Institutes of Health in Bethesda, Maryland, has reported that increased markers of neuronal inflammation and excitotoxicity were found in the brains of people who had had bipolar disorder. Phospholipase A2 and COX-2 were significantly elevated in the brains of those with bipolar illness and those with schizophrenia compared with controls. Pro-inflammatory interleukin I was also significantly increased in the brains of those who had had either illness. Read more