The New News About Lithium
Robert M. Post, Editor-in-Chief of the BNN, recently published an open access article in the journal Neuropsychopharmacology, “The New News About Lithium: An Underutilized Treatment in the United States.” Here we summarize the main points of the publication, including: the multiple benefits of lithium, its relative safety, predictors of lithium responsiveness, and principles for treatment.
Benefits of lithium
Lithium prevents both depressions and manias in bipolar disorder, and also prevents depressions in unipolar disorder and can augment antidepressant effects acutely. In addition to these mood benefits, lithium has anti-suicide effects. Lithium also enhances the efficacy of atypical antipsychotics and other mood stabilizers when used in combination with them.
Lithium is good for the brain. It has been shown to reduce the incidence of dementia. Lithium increases the volume of the hippocampus and cortex, and can increase the production of new neurons and glia. It also protects neurons. In animals, lithium has been shown to reduce lesion size in neurological syndromes that are models for human disorders such as AIDS-related neurotoxicity, ischemic/hemorrhagic stroke, traumatic brain/spinal cord injury, Huntington’s disease, Alzheimer’s disease, amyotrophic lateral sclerosis (ALS or Lou Gehrig’s disease), fragile X syndrome, Parkinson’s disease, retinal degeneration, multiple sclerosis, alcohol-induced degeneration, Down’s syndrome, spinocerebellar ataxia-1, and irradiation.
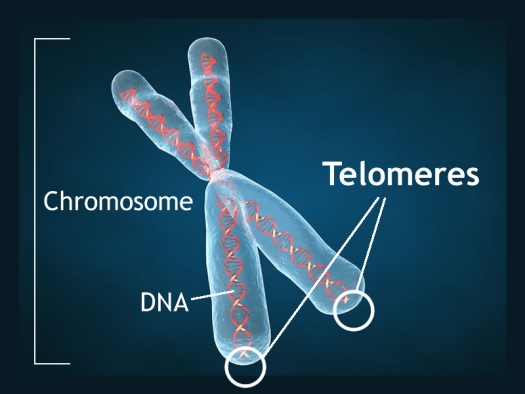
Lithium’s benefits include more general ones as well. It can increase the length of telomeres, bits of DNA on the ends of chromosomes that protect them during replication. Short telomeres have been linked to various illnesses and the aging process. Lithium also decreases the incidence of several medical illnesses and enhances survival.
Side Effects Are Often Benign, Treatable
Lithium side effects are more benign than many people think. Even low levels of lithium may be therapeutically sufficient. Read more
Deep TMS May Improve Treatment-Resistant Bipolar Depression
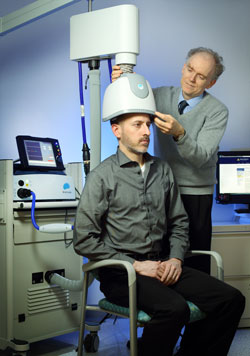 Deep transcranial magnetic stimulation (dTMS) is a non-invasive treatment that has been shown to be effective in unipolar depression. It consists of a helmet fitted to the head, which uses magnetic coils to create an electric field in a desired brain region.
Deep transcranial magnetic stimulation (dTMS) is a non-invasive treatment that has been shown to be effective in unipolar depression. It consists of a helmet fitted to the head, which uses magnetic coils to create an electric field in a desired brain region.
A 2017 double-blind randomized study by Diego F. Taveres and colleagues in the journal Neuropsychopharmacology found that 20 sessions of dTMS targeting the left dorsolateral prefrontal cortex produced greater improvement in bipolar depression over 4 weeks of treatment than the same number of sham sessions in which participants wore a helmet that delivered similar sounds and scalp sensations without the electrical effects to the brain. The participants had treatment-resistant bipolar depression that was being treated with medication.
However, dTMS’ effects were not significantly different from those of the sham over four additional weeks of follow-up, nor were remission rates significantly different across the two groups. Out of 50 participants, seven dropped out of the study—two from the sham group, and five from the active dTMS group. But there were no occasions on which a participant switched into mania following treatment.
This study suggests that dTMS has the potential to more rapidly improve treatment-resistant bipolar depression as well as unipolar depression.
Brain Scans Differentiate Suicidal from Non-Suicidal Patients with Bipolar Disorder
 People with bipolar disorder are at high risk for suicidal behavior beginning in adolescence and young adulthood. A 2017 study by Jennifer A. Y. Johnston and colleagues in the American Journal of Psychiatry uses several brain-scanning techniques to identify neurobiological features associated with suicidal behavior in people with bipolar disorder compared to people with bipolar disorder who have never attempted suicide. Clarifying which neural systems are involved in suicidal behavior may allow for better prevention efforts.
People with bipolar disorder are at high risk for suicidal behavior beginning in adolescence and young adulthood. A 2017 study by Jennifer A. Y. Johnston and colleagues in the American Journal of Psychiatry uses several brain-scanning techniques to identify neurobiological features associated with suicidal behavior in people with bipolar disorder compared to people with bipolar disorder who have never attempted suicide. Clarifying which neural systems are involved in suicidal behavior may allow for better prevention efforts.
The study included 26 participants who had attempted suicide and 42 who had not. Johnston and colleagues used structural, diffusion tensor, and functional magnetic resonance imaging (MRI) techniques to identify differences in the brains of attempters and non-attempters.
Compared to those who had never attempted suicide, those who had exhibited reductions in gray matter volume in the orbitofrontal cortex, hippocampus, and cerebellum. They also had reduced white matter integrity in the uncinate fasciculus, ventral frontal, and right cerebellum regions. In addition, attempters had reduced functional connectivity between the amygdala and the left ventral and right rostral prefrontal cortex. Better right rostral prefrontal connectivity was associated with less suicidal ideation, while better connectivity of the left ventral prefrontal area was linked to less lethal suicide attempts.
Offspring of Bipolar Parents Have More Psychiatric Illness
 A 2017 study from the Czech Republic found that children and adolescents with at least one parent with bipolar disorder had much higher lifetime rates of mood and anxiety disorders than their peers who did not have a parent with bipolar disorder. The offspring of bipolar parents also had lower quality of life, less social support, poorer self-perception, poorer relationships with their peers and parents, and more difficult home lives than those whose parents did not have bipolar disorder.
A 2017 study from the Czech Republic found that children and adolescents with at least one parent with bipolar disorder had much higher lifetime rates of mood and anxiety disorders than their peers who did not have a parent with bipolar disorder. The offspring of bipolar parents also had lower quality of life, less social support, poorer self-perception, poorer relationships with their peers and parents, and more difficult home lives than those whose parents did not have bipolar disorder.
The study by Michal Goetz and colleagues in the Journal of Child and Adolescent Psychopharmacology reported that 86% of the children of bipolar parents would be diagnosed with a psychiatric disorder in their lifetime. Similarly, David Axelson and colleagues from the Pittsburgh Bipolar Offspring Study reported in the American Journal of Psychiatry in 2015 that 74.2% of children with a parent with bipolar disorder would receive a lifetime psychiatric diagnosis, and a 2006 study by Myrna M. Weissman in the American Journal of Psychiatry found that the offspring of a unipolar depressed parent were three times more likely to have a psychiatric illness than offspring of nondepressed parents over 20 years of follow-up. Another study by this editor (Robert M. Post) and colleagues in the Bipolar Collaborative Network published in the Journal of Affective Disorders in 2016 found that a third of children at high risk due to a parent’s bipolar diagnosis would go on to have a psychiatric illness.
The Goetz study included a total of 86 participants between the ages of 7 and 18. Half had a parent with bipolar disorder and half did not. One limitation of the study was its recruitment procedure. Parents with bipolar disorder who enrolled their children in the study may have done so out of concern for their offspring’s mental health, increasing illness rates in the group with bipolar parents. Researchers were also aware of parents’ diagnoses, which may have affected their ratings of the young people’s symptoms. Despite these limitations, the study and its predecessors still suggest that psychiatric illness in a parent puts children at very high risk for a psychiatric illness themselves and can affect their wellbeing in a variety of ways.
Goetz and colleagues suggest that there is a need for proactive and complex care of families with psychiatric illness. They suggest that good communication is needed between adult and youth psychiatric services, with physicians who treat adults with bipolar disorder inquiring about those patients’ children and referring them to specialized psychiatric services for youth.
Editor’s Note: I not only endorse the conclusions of Goetz and colleagues, but would further recommend that parents with a diagnosis of bipolar disorder or unipolar depression discuss their children’s mood and behavior with their own psychiatrists and the children’s primary care physicians.
Parents of children aged 2 to 12 may enroll in our own Child Network, a secure online portal where they can record weekly ratings of their children’s symptoms and share these with their physicians.
There are many effective psychotherapeutic interventions for children with anxiety and mood disorders that should be sought for a child with symptoms that impair his or her functioning. Two evidence-based treatments are Family Focused Therapy, which incorporates family members into treatment so that they better understand the illness and can be supportive of the affected child, and cognitive behavioral therapy, in which negative patterns of thoughts and behaviors are challenged and patients are taught more effective problem-solving skills. When childhood psychiatric illness is recognized and treated appropriately, the results are often excellent, and it is possible that heading off the illness early may even prevent the development of more severe illness later in the child’s life.
Untreated Episodes of Bipolar Disorder Worsen Over Time, But Prevention is Possible
A 2017 literature review by researcher Lars V. Kessing and Per K. Andersen in the journal Acta Psychiatrica Scandinavica reports that the greater a patient’s number of previous episodes of bipolar disorder, the more likely that patient is to have a more difficult course of illness and poorer outcomes. The number of episodes was associated with more rapid recurrences, duration and severity of episodes, more automatic episodes (i.e. not triggered by stress), risk of dementia, treatment resistance, lack of recovery between episodes, and brain volume losses.
In an article in the journal Bipolar Disorders in 2016, BNN Editor-in-Chief Robert M. Post described the value of preventive treatment in reducing episodes and protecting the brain from the damage that accompanies them.
Given that episodes, stressors, and bouts of substance abuse can affect the way genes are transcribed via a phenomenon known as epigenetics, preventing these occurrences could lead to an easier course of illness and improved outcomes. Patients should provide their physicians with feedback about their response to prior medications and any side effects they experience over time so that their medication regime can be adjusted until it is maximally effective.
Patients with severe illness and multiple previous episodes may need a complex medication regimen that includes multiple types of medications that target different systems of neurotransmitters.
This philosophy of treatment is presented in several publications, including the 2008 book Treatment of Bipolar Illness: A Casebook for Clinicians and Patients by Post and Gabrielle Leverich, and more recently in the article “Treatment of Bipolar Depression: Evolving Recommendations” in the journal Psychiatric Clinics of North America. An open access article by Post, “New Perspectives on the Course and Treatment of Bipolar Disorders,” published in the journal Edizioni Minerva Medica S.p.A. in 2017, describes the need for early and sometimes complex combination therapy, including the non-intuitive idea that more medications (carefully prescribed) can actually produce fewer side effects than large doses of a single medication.
Another good resource for patients is a daily personal calendar that can be used to track ongoing symptoms, side effects, and response to medications. We offer several types of these calendars free here. My Mood Monitor, or What’s My M3, is a validated screening instrument that can detect depression, anxiety disorders, and mania in response to weekly self-reports. It is available online and as an app, and can be used to track illness course and response to treatment.
Short Telomeres Associated with Family Risk of Bipolar Disorder
Telomeres are bits of genetic material at the end of each strand of DNA that protect chromosomes as they replicate. Short telomeres have been linked to aging and a variety of medical and psychiatric diseases. Stress and depressive episodes can shorten telomeres, while treatment with lithium can lengthen them.
Telomere length is a heritable trait, and a 2017 study by researcher Timothy R. Powell and colleagues suggests that shorter telomeres are a familial risk factor for bipolar disorder.
The study, published in the journal Neuropsychopharmacology, compared the telomere lengths of 63 people with bipolar disorder, 74 of their immediate relatives (49 of whom had no lifetime psychiatric illness, while the other 25 had a different mood disorder), and 80 unrelated people with no psychiatric illness. The well relatives of the people with bipolar disorder had shorter telomeres than the unrelated healthy volunteers.
Relatives (both well and not) and people with bipolar disorder who were not being treated with lithium both had shorter telomeres than people with bipolar disorder who were being treated with lithium.
Another finding was that longer telomeres were linked to greater volume of the left and right hippocampus, and improved verbal memory on a test of delayed recall. This study provides more evidence that taking lithium increases the volume of the hippocampus and has neuroprotective benefits for people with bipolar disorder.
Methylphenidate Does Not Cause Mania When Taken with a Mood Stabilizer
 Methylphenidate is an effective treatment for attention-deficit hyperactivity disorder (ADHD). Ritalin may be the most commonly recognized trade name for methylphenidate, but it is also sold under the names Concerta, Daytrana, Methylin, and Aptensio. A 2016 article in the American Journal of Psychiatry reports that methylphenidate can safely be taken by people with bipolar disorder and comorbid ADHD as long as it is paired with mood-stabilizing treatment.
Methylphenidate is an effective treatment for attention-deficit hyperactivity disorder (ADHD). Ritalin may be the most commonly recognized trade name for methylphenidate, but it is also sold under the names Concerta, Daytrana, Methylin, and Aptensio. A 2016 article in the American Journal of Psychiatry reports that methylphenidate can safely be taken by people with bipolar disorder and comorbid ADHD as long as it is paired with mood-stabilizing treatment.
The study was based on data from a Swedish national registry. Researchers led by Alexander Viktorin identified 2,307 adults with bipolar disorder who began taking methylphenidate between 2006 and 2014. Of these, 1,103 were taking mood stabilizers including antipsychotic medications, lithium, or valproate, while 718 were not taking any mood stabilizing medications.
Among those who began taking methylphenidate without mood stabilizers, manic episodes increased over the next six months. In contrast, patients taking mood stabilizers had their risk of mania decrease after beginning treatment with methylphenidate.
Viktorin and colleagues suggest that 20% of patients with bipolar disorder may also have ADHD, so it is not surprising that 8% of patients with bipolar disorder in Sweden receive a methylphenidate prescription.
Mood-stabilizing drugs can worsen attention and concentration, so methylphenidate treatment can be helpful if it can be done without increasing manic episodes. However, Viktorin and colleagues suggest that due to the risk of increasing mania, anyone given a prescription for methylphenidate monotherapy should be carefully screened to rule out bipolar disorder.
The researchers confirmed that taking methylphenidate for ADHD while taking a mood stabilizer for bipolar disorder is a safe combination.
Safety of Atypical Antipsychotics in Pregnancy
A 2017 article in the Journal of Clinical Psychiatry systematically reviewed data on the risks related to schizophrenia, bipolar disorder, and treatment with atypical antipsychotic medication during pregnancy. The article by researcher Sarah Tosato and colleagues suggests that a mother’s illness may be more harmful to a fetus than treatment for that illness is.
The review analyzed 49 articles about illness-related and atypical antipsychotic–related risks in bipolar disorder and schizophrenia. Tosato and colleagues found that abrupt discontinuation of treatment led to a high risk of relapse in pregnant women with bipolar disorder or schizophrenia.
Schizophrenia was linked to a slight increase in obstetric complications for mothers, while both bipolar disorder and schizophrenia were linked to a slight increase in complications for newborns. Mothers ill with schizophrenia had the highest risk for serious complications, including stillbirth, neonatal or infant death, and intellectual disability in the child.
The researchers reported that untreated bipolar disorder and schizophrenia are risk factors for birth defects, but use of atypical antipsychotics is not. Children’s neurodevelopment also does not seem to be affected by mothers’ use of atypical antipsychotics during pregnancy.
The authors suggest that, given parents agree and understand any risks involved, the least harmful choice of action is to maintain treatment of women with bipolar disorder and schizophrenia during pregnancy at the safest minimum dosage to keep their illness at bay.
Birth Defects from Valproate Lower in Bipolar Disorder than in Epilepsy
 The anticonvulsant valproate increases the risk of serious birth defects in fetuses exposed to it. However, a 2017 report by ANSM, France’s agency for health and product safety, and its national insurance fund for employed workers shows that these risks are lower for women taking valproate for bipolar disorder than for women taking valproate for epilepsy.
The anticonvulsant valproate increases the risk of serious birth defects in fetuses exposed to it. However, a 2017 report by ANSM, France’s agency for health and product safety, and its national insurance fund for employed workers shows that these risks are lower for women taking valproate for bipolar disorder than for women taking valproate for epilepsy.
In France, the risk of a major fetal malformation was 10.2 per 1000 women in the general population, about twice that (22.2 per 1000) in women taking valproate for bipolar disorder, and about 4 times higher (46.5 per 1000) in women taking valproate for epilepsy. The authors suggest that treatment for bipolar disorder may be more likely to be interrupted during pregnancy, and this could explain the different levels of risk by diagnosis.
Among the risks of defects in the fetuses of women being treated with valproate for epilepsy, the risk of a ventricular septal defect (a hole in the wall separating the lower heart chambers) was 11.2% compared to 2.7% in fetuses not exposed to valproate, while risk of an atrial septal defect (a hole in the wall separating the upper heart chambers) was 19.1% in the fetuses of those prescribed valproate for epilepsy compared to 1.9% in unexposed fetuses. Risk of hypospadias (placement of the urethra opening on the underside of the penis rather than its end) was 22.7% compared to 4.8% in the general population.
Risks of a major malformation were dose dependent in those with epilepsy (but interestingly, not in those with bipolar disorder), meaning the more valproate patients with epilepsy took, the higher their risk of a fetus with birth defects.
The only birth defects that were more common in the fetuses of women taking valproate for bipolar disorder than in fetuses not exposed to valproate were hypospadias (17.5% risk compared to 4.8% in the general population) and craniostenosis, a deformity of the skull (4.2% risk compared to 0.4% in the general population).
The relative safety of valproate in women being treated for bipolar disorder compared to those being treated for epilepsy is good news for some. However, fetal exposure to valproate has also been linked to deficits in cognitive development.
The risk of spina bifida, which causes lifetime paralysis, in a fetus may no longer be such a catastrophic issue for women taking valproate for bipolar disorder (where the risk did not exceed that of the general population), as was once assumed based on data from women with epilepsy (where the risk is usually 2-4%, but was 8% in this French study). This may be of some comfort to women with bipolar disorder who require valproate treatment to remain stable and wish to become pregnant or in those who experience an unplanned pregnancy.
Dutch Study Links Low Vitamin D to Bipolar Disorder
A 2016 study in the Netherlands found that people with bipolar disorder are more likely to have vitamin D deficiency than the general population. Vitamin D deficiency has been linked to other psychiatric disorders including schizophrenia and unipolar depression. Poor diet and lack of exposure to sunlight can put someone at risk for vitamin D deficiency.
The study, led by Remco Boerman and published in the Journal of Clinical Psychopharmacology, included 118 adults with bipolar disorder, 149 with schizophrenia, and 53 with schizoaffective disorder. More than 30% of these participants had deficient levels of vitamin D. Only 15% had optimum levels of the vitamin. More than 22% of the participants with bipolar disorder were deficient in vitamin D, while close to 35% of those with schizophrenia and schizoaffective disorder were deficient.
Study participants had vitamin D levels that were 25% lower than those of the white Dutch population, and vitamin D deficiency was 4.7 times more common in those with psychiatric disorders than the general Dutch population.
The authors suggested screening people with bipolar disorder, schizophrenia, and schizoaffective disorder for low levels of vitamin D.