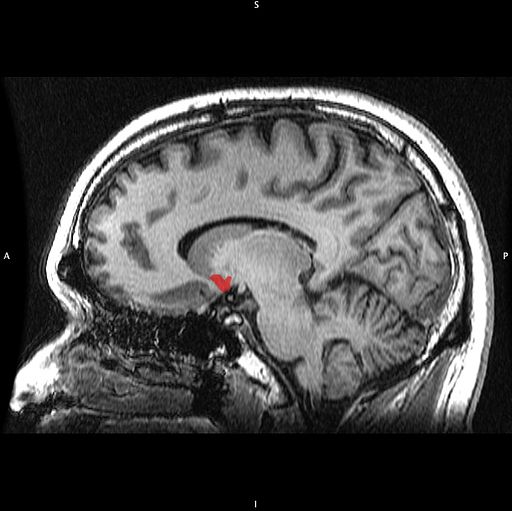
The Nucleus Accumbens in Depression
Brain-derived neurotrophic factor (BDNF) keeps neurons healthy and is critical for long-term memory and synapse formation. BDNF levels increase in the nucleus accumbens (the brain’s reward center) and decrease in the hippocampus during clinical depression and chronic cocaine use. In rodents, the same changes in BDNF levels occur during defeat stress (which resembles human depression).
Rodents who are repeatedly defeated by a larger rodent exhibit behaviors such as social withdrawal, lethargy, and decreased interest in sucrose. The increases in BDNF in the nucleus accumbens of these rodents could reflect the learning that takes place during the repeated defeat stress and the depression-like behaviors that follow it. Blocking the BDNF increases in the nucleus accumbens prevents these behaviors from developing.
Chadi Abdallah and other researchers at Yale University recently found that the left nucleus accumbens of patients with treatment-resistant depression is enlarged compared to normal controls, and the drug ketamine, which produces rapid-onset antidepressant effects, rapidly decreases the volume of the nucleus accumbens in the depressed patients. The mechanism by which it does so is unknown, but could reflect some suppression of the depressive learning.
Any relationship between the volume of the nucleus accumbens and its levels of BDNF is unknown, but ketamine’s effect on the size of this brain region could be linked to a decrease in the defeat-stress memories.
A Common Variant of BDNF Predicts Non-Response to IV Ketamine
Brain-derived neurotrophic factor (BDNF) is a protein in the brain that protects neurons and is necessary for long-term memory and learning. Different people have different genetic variations in BDNF depending on which amino acid the gene that codes for it inserts into the protein, valine or methionine. There are three possible combinations that vary in their efficiency. The Val66Val allele of BDNF is the most efficient for secreting and transporting BDNF within the cell body to synapses on dendrites, and is also a risk factor for early onset of bipolar disorder and rapid cycling. Twenty-five percent of the population has a Met variant (either Val66Met or Met66Met), which functions less efficiently. These people have mild decrements in some cognitive processing.
Increases in BDNF are necessary to the antidepressant effects of intravenous ketamine. In animals, ketamine also rapidly changes returns dendritic spines that had atrophied back to their healthy mushroom shape in association with its antidepressant effects. According to research published by Gonzalo Laje and colleagues in the journal Biological Psychiatry in 2012, depressed patients with the better functioning Val66Val allele of BDNF respond best to ketamine, while those with the intermediate functioning Val66Met allele respond less well.
Researcher Ronald S. Duman of Yale University recently found that increases in BDNF in the medial prefrontal cortex are necessary to the antidepressant effects of ketamine. If antibodies to BDNF (which block its effects) are administered to the prefrontal cortex, antidepressant response to ketamine is not observed.
Duman also found that calcium influx through voltage sensitive L-type calcium channels is necessary for ketamine’s antidepressant effects. A genetic variation in CACNA1C, a gene that codes for a subunit of the dihydropiridine L-type calcium channel, is a well-replicated risk factor for bipolar disorder. One might predict that those patients with the CACNA1C risk allele, which allows more calcium influx into cells, would respond well to ketamine.
Rationale for Using Ketamine in Youth with Treatment-Resistant Depression
At the 2013 meeting of the American Academy of Child and Adolescent Psychiatry, Vilma Gabbay of the Mount Sinai School of Medicine reiterated the findings from the TORDIA (Treatment of SSRI-Resistant Depression in Adolescents) study that 20% of young people with depression remained resistant to treatment, childhood-onset depression was more likely to be recurrent and more difficult than adult-onset depression in the long run, and suicide was the second leading cause of death in 12- to 17-year-olds in 2010 according to a Centers for Disease Control report in May 2013. Anhedonia (a loss of pleasure in activities once enjoyed) was the most difficult symptom to treat in adolescents.
Gabbay carefully explained some of the rationales for using ketamine in young people with depression. The presence of inflammation is a poor prognosis factor, and ketamine has anti-inflammatory effects, decreasing levels of inflammatory markers CRP, TNF-alpha, and Il-6.Given that ketamine has been widely used as an anesthetic for surgical procedures, its safety in children has already been demonstrated. Ketamine did not appear to cause behavioral sensitization (that is, increased effect upon repetition) in a report by Cho et al. in 2005 that included 295 patients.
As noted previously, Papolos et al. reported in a 2012 article in the Journal of Affective Disorders that intranasal ketamine at doses of 50 to 120 mg was well-tolerated and had positive clinical effects in 6- to 19-year-olds with the fear of harm subtype of bipolar disorder that had been highly resistant to treatment with more conventional drugs.
Gabbay reluctantly endorsed further cautious controlled trials in children and adolescents, in light of ketamine’s suggested efficacy and good safety profile, which stands in contrast to its popular reputation as a party drug or “Special K.”
Editor’s Note: The discussant of the symposium, Neal Ryan of Western Psychiatric Institute and Clinic, added an exquisitely brief discussion suggesting that ketamine should ultimately be studied in combination with behavioral and psychotherapeutic procedures to see if its therapeutic effects could be enhanced. He made this suggestion based on the data that ketamine has important synaptic effects, increasing brain-derived neurotrophic factor (BDNF), which is important for healthy cells and long-term memory, and reverting thin dendritic spines caused by stress back to their normal mushroom shape. This editor (Robert Post) could not be more in agreement.
IV Ketamine Superior to IV Midazolam in Adults with PTSD
In a recent study, ketamine performed better than an active comparator on several measures in adults with post-traumatic stress disorder (PTSD). Since ketamine has noticeable dissociative effects, researchers have looked for another drug with mind-altering effects that would be a more appropriate comparator than placebo.
At the 2013 meeting of the American Academy of Child and Adolescent Psychiatry, Adriana Feder of Mount Sinai Hospital reported on the randomized study in those with PTSD, in which intravenous ketamine was compared to intravenous midazolam, a potent benzodiazepine that produces anti-anxiety and sedating effects. Murrough et al. previously showed that intravenous ketamine was superior to midazolam in treatment-resistant depression.
In the randomized study Feder described, the participants had suffered PTSD from a physical or sexual assault and had been ill for 12 to 14 years. Those who received ketamine improved more, in some instances for as long as two weeks (ketamine’s blood levels disappear after a few hours, and its clinical antidepressant effects usually last only a few days). Reports of side effects included three patients with blood pressure increases requiring treatment with propranolol, and four patients who each had a transient episode of vomiting.
These controlled data parallel previous open observations. When ketamine was used as a surgical anesthetic during operations on burn patients, only 26.9% subsequently reported PTSD compared to 46.4% who developed PTSD when an alternative to ketamine was used as the anesthetic.
Intranasal Ketamine May Be an Alternative to IV in Refractory Depression
At the 2013 meeting of the American Academy of Child and Adolescent Psychiatry, Kyle Lapidus of Mount Sinai Hospital reviewed the literature from controlled studies on the efficacy of intravenous (IV) ketamine at a dosage of 0.5 mg/kg over a 40-minute infusion for adults with treatment-resistant depression (with consistent response rates of 50% or more), and suggested that intranasal ketamine may also be effective.
Ketamine is a strong blocker of the glutamate NMDA receptor. At high doses (6 to 12 mg/kg) it is an anesthetic, at slightly lower doses (3 to 4 mg/kg) it is psychotomimetic (causing psychotic symptoms) and is sometimes used as a drug of abuse, and at very low doses it is a rapidly acting antidepressant, often bringing about results within 2 hours. Antidepressant effects typically last 3 to 5 days, so the question of how to sustain these effects is a major one for the field.
Murrough et al. reported in Biological Psychiatry in 2012 that five subsequent infusions of ketamine sustained the initial antidepressant response and appeared to be well tolerated by the patients. Another NMDA antagonist, riluzole (used for the treatment of ALS or Lou Gehrig’s disease), did not sustain the acute effects of ketamine, and now lithium is being studied as a possible strategy for doing so.
The bioavailability of ketamine in the body depends on the way it is administered. Compared to IV administration, intramuscular (IM) administration is painful but results in 93% of the bioavailability of IV ketamine. Intranasal (IN) administration results in 25-50% of the bioavailability of IV administration, while oral administration results in only 16-20% of the bioavailability of IV administration, so Lapidus chose to study the IN route. He compared intranasal ketamine at doses of 50mg (administered in a mist ) to 0.5 ml of intranasal saline. Both were given in two infusions seven days apart. Lapidus observed good antidepressant effects and good tolerability. Papolos et al. had reported earlier that intranasal ketamine had good effects in a small open trial in treatment-resistant childhood onset bipolar disorder.
Editor’s Note: Further studies of the efficacy and tolerability of intranasal ketamine are eagerly awaited.
New Research on Ketamine
 The drug ketamine can produce antidepressant effects within hours when administered intravenously.
The drug ketamine can produce antidepressant effects within hours when administered intravenously.
Finding an Appropriate Control
Comparing ketamine to placebo has challenges because ketamine produces mild dissociative effects (such as a feeling of distance from reality) that are noticeable to patients. At the 2013 meeting of the Society of Biological Psychiatry, James W. Murrough and collaborators at the Mount Sinai School of Medicine reported their findings from the first controlled trial of intravenous ketamine in depression that uses an active control, the short-acting benzodiazepine midazolam, which has sedative effects and decreases anxiety, but is not known as an antidepressant. On virtually all measures intravenous ketamine was a more effective antidepressant following 2 infusions per week.
These data help dispel one of the criticisms of intravenous ketamine, that studies of the drug have not been sufficiently blinded (when patients and medical staff are kept from knowing which patients receive an active treatment and which are in the placebo control group) and that the lack of an appropriate active placebo contributed to the dramatic findings about ketamine’s antidepressant effects. It now appears that these criticisms have been appropriately answered and that intravenous ketamine is highly effective not only in comparison to placebo but also to an active comparator.
This research was presented as a poster at the meeting and published as abstract #442 in the meeting supplement to the journal Biological Psychiatry, Volume 73, Number 9S, and was also published in the Archives of General Psychiatry in 2013.
Slowing Down Ketamine Infusions to Reduce Side Effects
Ketamine is commonly given in 40-minute intravenous infusions. Timothy Lineberry from the Mayo Clinic reported in Abstract #313 from the meeting that slower infusions of ketamine over 100 minutes were also effective in producing antidepressant effects in patients with treatment-resistant depression. Lineberry’s research group used the slower infusion in order to increase safety and decrease side effects, such as the dissociative effects discussed above. In the 10 patients the group studied, they observed a response rate of 80% and a remission rate of 50% (similar to ketamine’s effects with 40-minute infusions).
Family or Personal History of Alcohol Dependence Predicts Positive Response to Ketamine in Depression
Mark J. Niciu and collaborators at the NIMH reported in Abstract #326 that a personal or family history of alcohol dependence predicted a positive response to IV ketamine in patients with unipolar depression.
Ketamine Acts on Monoamines in Addition to Glutamate
Ketamine’s primary action in the nervous system is to block glutamate NMDA receptors in the brain. In addition to its effects on glutamate, it may also affect the monoamines norepinephrine and dopamine. Kareem S. El Iskandarani et al. reported in Abstract #333 that in a study of rats, ketamine increased the firing rate of norepinephrine neurons in a part of the brain called the locus coeruleus and also increased the number of spontaneous firing dopamine cells in the ventral tegmental area of the brain.
Editor’s Note: These data showing that ketamine increased the activity of two monoamines could help explain ketamine’s ability to induce rapid onset of antidepressant effects, in addition to its ability to immediately increase brain-derived neurotrophic factor (BDNF, important for long-term memory and the creation of new synapses) and to restore healthy mushroom-shaped spines on the dendrites of neurons in the prefrontal cortex.
Family History Of Alcoholism Predicts Positive Response To Ketamine
 The drug ketamine can bring about antidepressant effects rapidly when given intravenously, but these effects last only a few days. In a recent study, bipolar depressed patients with alcoholism or a family history of alcoholism in first-degree relatives had a more extended positive antidepressant response to IV ketamine than those without this history, and fewer adverse effects from the treatment. The study, published by David Luckenbaugh et al. from the National Institute of Mental Health in the journal Bipolar Disorders in December 2012, replicates similar findings in patients with unipolar depression, where positive family history of alcoholism also predicted better response and fewer adverse effects from IV ketamine.
The drug ketamine can bring about antidepressant effects rapidly when given intravenously, but these effects last only a few days. In a recent study, bipolar depressed patients with alcoholism or a family history of alcoholism in first-degree relatives had a more extended positive antidepressant response to IV ketamine than those without this history, and fewer adverse effects from the treatment. The study, published by David Luckenbaugh et al. from the National Institute of Mental Health in the journal Bipolar Disorders in December 2012, replicates similar findings in patients with unipolar depression, where positive family history of alcoholism also predicted better response and fewer adverse effects from IV ketamine.
Alcohol and ketamine have a common mechanism of action. They are both antagonists of the glutamate NMDA receptor, meaning they limit the effects of glutamate, the major excitatory neurotransmitter in the brain. This suggests a theoretical explanation for why a history of alcoholism might relate to ketamine response.
Editor’s Note: Family history appears to be linked to how patients respond to different mood stabilizers. Lithium works best in those patients with a positive family history of mood disorders (especially bipolar disorder). Carbamazepine works best in those without a family history of bipolar disorder among first-degree relatives. Lamotrigine works best in those with a positive family history of anxiety disorders or alcoholism.
Drugs that are effective in patients with a family history of alcoholism all target glutamate in the brain. Lamotrigine decreases glutamate release, while ketamine reduces glutamate’s effects at the receptor. Both decrease glutamate function or activity. Like lamotrigine, carbamazepine also decreases glutamate release and has good effects in those with a history of alcoholism.
Memantine is another mood-stabilizing drug that is an antagonist of the NMDA receptor, like ketamine and alcohol. It will be interesting to see whether memantine will also be successful in those with a personal or family history of alcoholism.
Psychiatric Revolution: Changes in Behavior Are Associated with Dendritic Spine Shape and Number
New research shows that cocaine, defeat stress, the rapid-acting antidepressant ketamine, and learning and memory can change the size, shape, or number of spines on the dendrites of neurons. Dendrites conduct electrical impulses into the cell body from neighboring neurons.
Cocaine
Several researchers, including Peter Kalivas at the Medical University of South Carolina, have reported that cocaine increases the size of the spines on the dendrites of a certain kind of neurons (GABAergic medium spiny neurons) in the nucleus accumbens (the reward center in the brain). This occurs through a dopamine D1 selective mechanism. N-acetylcysteine, a drug that can be found in health food stores, decreases cocaine intake in animals and humans, and also normalizes the size of dendritic spines.
Depression
Depression in animals and humans is associated with decreases in Rac1, a protein in the dendritic spines on GABA neurons in the nucleus accumbens. Rac1 regulates actin and other molecules that alter the shape of the spines.
In an animal model of depression called defeat stress, rodents are stressed by repeatedly being placed in a larger animal’s territory. Their subsequent behavior mimics clinical depression. This kind of social defeat stress decreases Rac1 and causes spines to become thin and lose some function. Replacing Rac1 returns the spines to a more mature mushroom shape and reverses the depressive behavior of these socially defeated animals. Researcher Scott Russo has also found Rac1 deficits in the nucleus accumbens of depressed patients who committed suicide. Russo suggests that decreases in Rac1 are responsible for the manifestation of social avoidance and other depressive behaviors in the defeat stress animal model, and that finding ways to increase Rac1 in humans would be an important new target for antidepressant drug development.
Another animal model of depression called chronic intermittent stress (in which the animals are exposed to a series of unexpected stressors like sounds or mild shocks) also induces depression-like behavior and makes the dendritic spines thin and stubby. The drug ketamine, which can bring about antidepressant effects in humans in as short a time as 2 hours, rapidly reverses the depressive behavior in animals and converts the spines back to the larger, more mature mushroom-shape they typically have.
Learning and Extinction of Fear
Researcher Wenbiao Gan has reported that fear conditioning can change the number of dendritic spines. When animals hear a tone paired with an electrical shock, they begin to exhibit a fear response to the tone. In layer 5 of the prefrontal cortex, spines are eliminated when conditioned fear develops, and are reformed (near where the eliminated spines were) during extinction training, when animals hear the tones without receiving the shock and learn not to fear the tone. However, in the primary auditory cortex the changes are opposite: new spines are formed with learning, and spines are eliminated with extinction.
Editor’s Note: It appears that we have arrived at a new milestone in psychiatry. In the field of neurology, changes seen in the brains of patients with strokes or Alzheimer’s dementia have been considered “real” because cells were obviously lost or dead. Psychiatry, in comparison, has been considered a soft science because neuronal changes have been more difficult to see and illnesses were and still are called “mental.” Now that new technologies have made a deeper level of precision, observation, and analysis possible, we know that the brain’s 12 billion neurons and 4 times as many glial cells are exquisitely plastic–capable of biochemical and structural changes that can be reversed using appropriate therapeutic maneuvers.
The changes associated with abnormal behaviors, addictions, and even normal processes of learning and memory now have clearly been shown to correspond with the size, shape, and biochemistry of dendritic spines. These subtle, reproducible changes in the brain and body are amenable to therapeutic intervention, and are now even more demanding of sophisticated medical attention.
Intranasal Ketamine Helps Some Kids with Bipolar Disorder
 The anesthetic ketamine given intranasally may help children with a certain type of bipolar disorder. In an article published in the Journal of Affective Disorders in 2013, Demetri Papolos et al. reported seeing marked improvement in a subgroup of 12 children aged 6 to 19 years of age who were nonresponsive to the usual treatment regimens of lithium, mood stabilizers, and antipsychotics. Papolos has described these children as having the “fear of harm (FOH) subtype.” In addition to having typical mood swings, these children also have a fear of aggression, separation anxiety, sleep and circadian rhythm disorders, nightmares, thermoregulatory problems, and carbohydrate craving.
The anesthetic ketamine given intranasally may help children with a certain type of bipolar disorder. In an article published in the Journal of Affective Disorders in 2013, Demetri Papolos et al. reported seeing marked improvement in a subgroup of 12 children aged 6 to 19 years of age who were nonresponsive to the usual treatment regimens of lithium, mood stabilizers, and antipsychotics. Papolos has described these children as having the “fear of harm (FOH) subtype.” In addition to having typical mood swings, these children also have a fear of aggression, separation anxiety, sleep and circadian rhythm disorders, nightmares, thermoregulatory problems, and carbohydrate craving.
Ketamine was given as an intranasal spray using an inhaler in 10mg doses. Doses were increased until the targeted symptoms remitted. Average doses ranged from 30mg to 120mg, given every 3 to 7 days. All symptom areas including depression and mania improved markedly, usually within a few hours, and this improvement lasted 3 to 4 days. Four types of aggression (measured on the Overt Aggression Scale) decreased significantly.
There were some dissociative side effects that were usually mild to moderate, but occasionally severe. They resolved spontaneously, usually within the first hour after treatment, and there appeared to be tolerance to them following repeated administration.
The authors urged caution until findings from these cases are confirmed by more controlled studies, but they concluded that the magnitude and rapidity of effects in these children with treatment resistant bipolar disorder suggested effectiveness and safety.
Ketamine for OCD
At a recent scientific meeting, researcher Carolyn Rodriguez presented a randomized controlled crossover trial of ketamine in obsessive-compulsive disorder (OCD). In contrast to a previous negative study by Block and associates at the National Institute of Mental Health (NIMH), these investigators found that intravenous (IV) infusion of ketamine (0.5 mg/kg over 40 minutes) was associated with a larger reduction in obsessive-compulsive symptoms when compared with saline infusion. These effects were rapid in onset and persisted for approximately one week in 50% of the patients with OCD who had constant intrusive thoughts.
This dose of ketamine had previously been shown to induce rapid-onset improvement in depression and suicidal ideation in those with unipolar and bipolar depression. However, the improvement in obsessive-compulsive disorder symptoms appeared unrelated to any antidepressant effect because the individuals with OCD had minimal depressive symptoms at baseline.
The traditional pharmacological treatments for OCD are selective serotonin reuptake inhibitor (SSRI) antidepressants, which require high doses and weeks to months before the onset of full effect. In contrast, Rodriguez et al. found a 90% response rate to IV ketamine within 3 hours.
Ketamine is a blocker of the glutamate NMDA receptors, and these data suggest that targeting these receptors can induce rapid onset of positive effects in OCD. However, as is the case with the acute antidepressant response to ketamine in those with depression, the best ways to extend this therapeutic effect long-term remain to be determined.
Another blocker of NMDA receptors, the anti-Alzheimer’s drug memantine (Namenda), has been reported in open studies to show improvement in those with OCD as well. N-acetylcysteine, a substance found in health-food stores, likewise appears to re-regulate a hyper-responsive glutamatergic system in the nucleus accumbens by other mechanisms, and was also shown to have efficacy as an augmenting treatment in OCD in those who are inadequately responsive to SSRIs in a 2012 article by Afshaw et al.
Editor’s Note: Taken together, the data with ketamine, memantine, and N-acetylcysteine suggest that glutamate-based mechanisms are involved in OCD and may provide an alternative target for therapeutics in addition to serotonin.