TDCS Better Than Placebo But Not as Good as Escitalopram at Improving Unipolar Depression
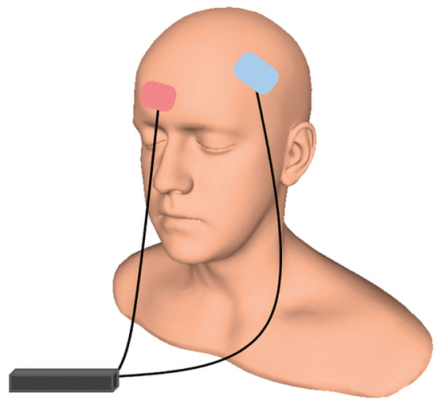 An article by André R. Brunoni and colleagues in the New England Journal of Medicine reports that transcranial direct current stimulation (tDCS) can treat unipolar depression more effectively than placebo, but not quite as effectively as the selective serotonin reuptake inhibitor (SSRI) antidepressant escitalopram. TDCS consists of a constant, low direct current applied to the scalp via electrodes.
An article by André R. Brunoni and colleagues in the New England Journal of Medicine reports that transcranial direct current stimulation (tDCS) can treat unipolar depression more effectively than placebo, but not quite as effectively as the selective serotonin reuptake inhibitor (SSRI) antidepressant escitalopram. TDCS consists of a constant, low direct current applied to the scalp via electrodes.
The study included 245 patients with moderate to severe depressive symptoms, many of whom also had anxiety disorders. To minimize the placebo effect, patients all participated in sessions wearing tDCS gear and received a daily pill. However, one group received real tDCS treatment but placebo pills, a second group received sham tDCS but real escitalopram pills, and the third group received both sham tDCS and placebo pills.
The real tDCS treatment consisted of 30-minute sessions of tDCS every day for 15 consecutive weekdays, then seven once-a-week treatments. The escitalopram dosage was 10 mg/day for three weeks, then 20 mg daily.
Ten weeks into treatment, those who received escitalopram showed the greatest improvement in depression. Those who received tDCS showed slightly less improvement, but still significantly more than those who received neither treatment. Cognitive performance either improved or stayed the same in all the groups.
In terms of side effects, those who received escitalopram were more likely to report sleepiness or severe constipation. Those who received tDCS reported more skin redness/tingling, itching, tinnitus, and nervousness. Two patients in the tDCS group had new-onset mania during treatment. There were no suicides, hospitalizations, or other serious side effects.
Arthritis Drug Celecoxib May Improve Bipolar Depression When Paired with Escitalopram
A new study suggests that for people with bipolar depression, the anti-inflammatory drug celecoxib (Celebrex), typically used to treat arthritis, can boost the effectiveness of the antidepressant escitalopram (Lexapro).
In the 8-week study by researcher Angelos Halaris and colleagues, adults with bipolar depression were randomly assigned to one of two groups. The first group received the selective-serotonin reuptake inhibitor (SSRI) antidepressant escitalopram plus celecoxib to target inflammation. The second group received just the antidepressant escitalopram and a placebo.
By the end of the study, 78% of the group taking the anti-arthritis drug had seen major improvement in their depression, with 63% reporting that it had lifted completely. Meanwhile in the placebo group, only 45% reported major improvement, and 10% reported remission.
The group that received celecoxib with their escitalopram also began seeing improvement within one week of beginning treatment, instead of after four to six weeks, which is typical of antidepressant treatment.
Researchers think depression creates an immune response leading to chronic inflammation, which can upset the balance of neurotransmitters in the brain and make antidepressants less effective. Halaris suggests that reducing this inflammation with a drug like celecoxib can make antidepressants more effective.
The research was presented at the Fifth International Congress on Psychiatry and the Neurosciences and has not yet been published.
Creatine Supplements May Speed Up Response to Escitalopram, Improve Brain Connectivity
Antidepressants can take weeks to begin working, and researchers have been investigating ways to speed up this process. A 2012 study by In Kyoon Lyoo and colleagues in the American Journal of Psychiatry found that among 52 women taking the selective serotonin reuptake inhibitor (SSRI) antidepressant escitalopram (Lexapro) for unipolar depression, those who were prescribed an additional creatine supplement had earlier and greater decreases in depression symptoms than those who received a placebo in addition to the escitalopram.
The difference between the two groups was evident by the second week of treatment. At the end of the 8-week study, 52% of those who received creatine had achieved remission, compared to 26% of those in the placebo group.
Creatine, a supplement sometimes used by weightlifters, increases cellular energy. The women received 3g/day of creatine for the first week of the study, and 5g/day thereafter.
The same research group recently published more data from their creatine study. The new article by Sujung Yoon and colleagues in the journal Biological Psychiatry shows that following the creatine supplementation, the women in the creatine group had greater levels of N-acetylaspartate (a sign of healthy neurons) in their prefrontal cortex and also had greater levels of brain connectivity than women in the placebo group.
Combination of SSRIs and Statins Better than SSRIs Alone
A large study in Denmark suggests that taking selective serotonin reuptake inhibitor (SSRI) antidepressants alongside cholesterol-lowering statin drugs improved depression more than SSRIs alone. The findings, by Ole Köhler and colleagues were reported in the American Journal of Psychiatry in 2016.
The study included 872,216 people in Denmark’s national health care database who took SSRIs between 1997 and 2012. The most common SSRIs were citalopram, sertraline, and escitalopram. Of these people taking SSRIs, 13.0% also took a statin drug, typically simvastatin. Those patients who were taking both an SSRI and a statin were less likely than those taking an SSRI alone to be hospitalized for any psychiatric problem, or for depression specifically.
Depression is known to be correlated with inflammation throughout the body. Statins reduce this inflammation as well as lowering cholesterol. A 2013 study by Ahmad Ghanizadeh and Arvin Hedayati in the journal Depression and Anxiety showed that the SSRI fluoxetine and the statin lovastatin reduced depression severity compared to fluoxetine alone.
The combination of SSRIs and statins did not seem to reduce deaths or suicidal behavior compared to SSRIs alone. Statins have some side effects, but combining them with antidepressants did not increase the risks associated with their use.
More Evidence that Statins Can Reduce Depression in People with Acute Coronary Syndrome
Many studies have linked depression and cardiovascular problems. The solutions may also be linked. A new study found that patients with depression and acute coronary syndrome saw their depression improve most when they took the selective-serotonin reuptake inhibitor (SSRI) antidepressant escitalopram and statins (used to lower cholesterol), while depression improved least among patients who took neither type of drug. Statin use was linked to improvement in depression after one year, while escitalopram was not. In a subset of the study, use of lipophilic statins in particular was linked to improvement in depression.
The study, published in 2015 by S.W. Kim and colleagues in the journal Translational Psychiatry, suggests that statins can improve depression regardless of antidepressant use, but combining statins with an SSRI may have an even more powerful effect on depression.
Preliminary Evidence That Anti-Inflammatory Celecoxib Helps in Bipolar Depression
A study currently in progress indicates that the anti-inflammatory COX-2 inhibitor celecoxib (better known as the arthritis treatment Celebrex) may aid in the treatment of bipolar depression. In a panel session on inflammation at the 2015 meeting of the Society of Biological Psychiatry, researcher Angelos Halaris reported results from the first 26 participants.
Participants were taking mood stabilizers for bipolar disorder and became depressed. They received either 20mg/day of the selective serotonin reuptake inhibitor antidepressant escitalopram (Lexapro) plus either 200mg twice a day of celecoxib or placebo for a total of eight weeks. Those participants who received celecoxib showed greater and more rapid reductions in depression symptoms than those who received placebo.
The study will continue, and Halaris and colleagues will also observe whether measures of inflammation in patients’ blood are correlated with the patients’ responsiveness to the combined treatment with escitalopram and celecoxib.
Mother’s Treatment for Depression Can Affect Children’s Symptoms
Studies have found that when a depressed mother’s symptoms remit, her children are less likely to show psychiatric symptoms. A new study by Myrna M. Weissman and colleagues in the American Journal of Psychiatry randomized 76 mothers to treatment with escitalopram, bupropion, or a combination of the two, and assessed the impact of the mothers’ treatment on their 135 children (aged 7–17).
There were no significant differences in the mothers’ symptoms or remission, but children’s depressive symptoms and functioning improved more if their mothers received (only) escitalopram. Only in that group was a mother’s improvement associated with her children’s improvement.
Mothers in the escitalopram group reported greater improvement in their ability to listen and talk to their children compared to the mothers in other groups, and the children of the mothers in the escitalopram group reported that their mothers were more caring.
Children of mothers with low negative affect improved significantly, while children of mothers with high negative affect only improved if their mothers were in the escitalopram group.
The authors suggest that for a mother’s improvement to help her children’s symptoms, her anxious distress and irritability must be reduced, and these may be better targeted with escitalopram than bupropion.
Ziprasidone Added to Escitalopram Improved Unipolar Depression
In a new study of patients with major depressive disorder who did not improve after eight weeks of the selective serotonin reuptake inhibitor (SSRI) antidepressant escitalopram, the addition of the atypical antipsychotic ziprasidone improved their depression more than did placebo. Patients took the combination of escitalopram (20mg/day on average) and ziprasidone twice a day at doses of 20–80 mg.
This was the first randomized, double-blind placebo controlled trial of ziprasidone as an adjunct treatment for unipolar depression. While ziprasidone was more efficacious than placebo, discontinuation of the study due to intolerance was higher among the patients who received ziprasidone.
Editor’s Note: Two atypical antipsychotics (quetiapine and aripiprazole) have been approved by the Federal Drug Administration for augmentation of antidepressants in unipolar depression. Now there have also been placebo-controlled positive trials of two others (ziprasidone and cariprazine).
These findings are of particular interest as the studies of ziprasidone monotherapy in bipolar depression not only failed, but response to ziprasidone and placebo was virtually identical (and negligible).
If You Are Depressed After a Heart Attack, Treat the Depression
 Depression is common following heart attacks, and it can complicate recovery. A recent study by Jae-Min Kim and colleagues investigated the safety of treating depression with escitalopram in people recovering from acute coronary syndrome. In a 2015 article in the Journal of Clinical Psychiatry, they reported that 217 people with depression and acute coronary syndrome were randomized to receive either escitalopram (in flexible doses ranging from 5–20 mg/day) or placebo for 24 weeks. Patients who received escitalopram saw more improvement in their depression on a variety of scales, and also showed improvements in social and occupational functioning. There were no adverse cardiac effects from escitalopram, though some people taking it did experience dizziness.
Depression is common following heart attacks, and it can complicate recovery. A recent study by Jae-Min Kim and colleagues investigated the safety of treating depression with escitalopram in people recovering from acute coronary syndrome. In a 2015 article in the Journal of Clinical Psychiatry, they reported that 217 people with depression and acute coronary syndrome were randomized to receive either escitalopram (in flexible doses ranging from 5–20 mg/day) or placebo for 24 weeks. Patients who received escitalopram saw more improvement in their depression on a variety of scales, and also showed improvements in social and occupational functioning. There were no adverse cardiac effects from escitalopram, though some people taking it did experience dizziness.
CRP, A Readily Available Marker of Inflammation, Predicts Response To Two Antidepressants
C-reactive protein, or CRP, is a protein found in blood plasma, the levels of which rise in response to inflammation. In a recent study, levels of CRP were able to predict which of two antidepressants a patient was more likely to respond to.
The 2014 article by Rudolph Uher et al. in the American Journal of Psychiatry reported that low levels of CRP (<1 mg/L) predicted a good response to the selective serotonin reuptake inhibitor (SSRI) escitalopram (Lexapro) while higher levels of CRP predicted a good response to the tricyclic antidepressant nortriptyline, a blocker of norepinephrine reuptake.
The research was part of the Genome-Based Therapeutic Drugs for Depression (GENDEP) study, a multicenter open-label randomized clinical trial. CRP was measured in the blood of 241 adult men and women with major depressive disorder. In the article the researchers say that CRP and its interaction with medication explained more than 10% of the individual variance in response to the two antidepressants.
If these findings can be replicated with these and similarly acting drugs, it would be a very large step in the direction of personalized medicine and the ability to predict individual response to medications.