Certain Types of Inflammation and BMI Predict Depression
At the 2016 meeting of the Society of Biological Psychiatry, researcher Femke Lamers and colleagues presented findings from the Netherlands Study of Depression and Anxiety. The inflammatory markers interleukin-6 and CRP were elevated in people with current major depression. These measures were correlated with BMI, a measure of body weight. High levels of interleukin-6 at the beginning of the study predicted who would have a chronic course of illness.
Editor’s Note: Previous studies have found that elevated levels of CRP predicted a future mood episode in people at high risk for bipolar disorder due to a family history of the illness.
These studies suggest that it might be useful to assess levels of these inflammatory markers (CRP, interleukin-1, interleukin-6, and TNF-alpha) in young people who are at high risk for bipolar disorder. Factors that put someone at high risk include a family history of depression or bipolar disorder, a history of adversity in childhood (abuse, neglect, loss of a parent, etc.), and preliminary symptoms.
Several interventions are available that may reduce the likelihood that someone at risk for bipolar disorder will go on to develop the illness. Family interventions such as the Family Focused Therapy developed by researcher David Miklowitz are helpful. In a 2013 study in the Journal of the American Academy of Child and Adolescent Psychiatry, Miklowitz reported that Family Focused Therapy outperformed treatment as usual for youth at risk for bipolar disorder.
Measures of inflammation might provide additional rationale for beginning interventions in youth at high risk for mood disorders. In addition to family interventions, omega-3 fatty acid supplementation is a low-risk option that is supported by some positive data. Since BMI was implicated in the study by Lamers and colleagues, keeping weight under control might also have some benefit.
For adults with depression who want to keep their weight under control, the combination of the antidepressant bupropion XR (150–300mg/day) and naltrexone (50mg/day), an opiate antagonist medication normally used to fight addictions, has been effective.
Emotional Abuse Increases Inflammation
Trauma in childhood is a risk factor for depression, and both childhood trauma and depression have been linked to increased inflammation. In a study presented at the 2016 meeting of the Society of Biological Psychiatry, Sarah R. Horn and colleagues found that emotional abuse in childhood predicted high levels of inflammation measured in the blood in adulthood.
Horn and colleagues took blood samples from 35 people with treatment-resistant depression and 28 healthy control subjects. The researchers measured inflammatory markers in the blood and also interviewed the participants about any physical, sexual, or emotional abuse they experienced in childhood. Among all the participants, emotional abuse was linked to elevated levels of several inflammatory markers, including interleukin-6, interleukin-10, interleukin-1a, interleukin-15, and fractalkine.
The researchers suggest that more research is needed to clarify the link between early trauma, depression, and inflammation. How elevated inflammation in people with a history of abuse may influence the effectiveness of different psychotherapies and medications for depression remains to be determined.
Inflammation Linked to Non-Response to Antidepressants
In a symposium on inflammation’s role in psychiatric disorders at the 2016 meeting of the Society of Biological Psychiatry, researcher Carmine Pariante reviewed the considerable literature indicating that major depression is often associated with measures of inflammation. Depression has been linked to elevated blood levels of the inflammatory proteins interleukin-1, interleukin-6, TNF alpha, and c-reactive protein, with about one-third of depressed patients having an elevated level of at least one of these proteins. People with elevated inflammatory markers are also less likely to respond to traditional antidepressants such as selective serotonin reuptake inhibitors (SSRIs).
Pariante reported that in depressed people, interleukin-6 is also elevated in cerebrospinal fluid in addition to blood, suggesting that inflammation in depression extends to the central nervous system. Increased secretion of interleukin-6 has been linked to depressive behaviors in mice exposed to stress.
There is some hope that anti-inflammatory treatments can help patients who do not respond to traditional antidepressant treatment. Some anti-inflammatory medications that may eventually be used to treat depression with inflammation include the COX-1 inhibitor aspirin, the COX-2 inhibitor celecoxib (Celebrex), or the antibiotic minocycline. Each of these approaches gained some support in preliminary clinical trials, but it has not yet been established that these anti-inflammatory treatments produce a better response in people with elevated inflammatory markers.
Inflammation Linked to Post-Stroke Depression
A 2016 study in the journal Psychoneuroendocrinology confirms that high levels of inflammatory cytokines in the blood are linked to higher risk of depression following a stroke.
The study, by Hee-Ju Kang and colleagues, followed 222 stroke sufferers for one year. Two weeks following the stroke, their levels of inflammatory cytokines IL-6 and IL-18 were measured. They were also assessed for depression both at the two-week point and one year later. The researchers also observed whether or not the participants were treated with statins, which are often prescribed to lower stroke risk and also have anti-inflammatory effects.
Those participants who had depression following their strokes (either at two weeks or at one year) tended to be older, to have a history of depression or stroke, to have a more severe stroke, and to have a stroke location toward the front of the brain.
Having any depression following the stroke was associated with higher levels of IL-6 and IL-18. This was particularly true of those participants who were not taking a statin. Among those taking statins, the statins may have interfered with the link between inflammatory cytokines and post-stroke depression. In the statin group, the only significant finding was a link between levels of IL-6 and depression at the two-week mark.
Blood and Now Brain Inflammation Linked to Depression
 There is growing evidence of a link between inflammation of depression. At the 2015 meeting of the Society of Biological Psychiatry, researcher Jeff Meyer summarized past studies on inflammatory markers. These are measurements, for example of certain proteins in the blood, that indicate the presence of inflammation in the body.
There is growing evidence of a link between inflammation of depression. At the 2015 meeting of the Society of Biological Psychiatry, researcher Jeff Meyer summarized past studies on inflammatory markers. These are measurements, for example of certain proteins in the blood, that indicate the presence of inflammation in the body.
Common inflammatory markers that have been linked to depression include IL-6, TNF-alpha, and c-reactive protein. At the meeting, Meyer reviewed the findings on each of these. Twelve studies showed that IL-6 levels are elevated in the blood of patients with depression. Four studies had non-significant results of link between IL-6 and depression, and Meyer found no studies indicating that IL-6 levels were lower in those with depression. Similarly, for TNF-alpha, Meyer found 11 studies linking elevated TNF-alpha with depression, four with non-significant results, and none showing a negative relationship between TNF-alpha and depression. For c-reactive protein, six studies showed that c-reactive protein was elevated in people with depression, six had non-significant results, and none indicated that c-reactive protein was lower in depressed patients.
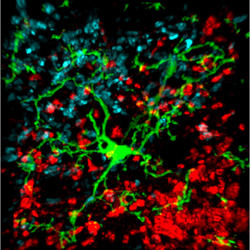
Most studies that have linked inflammation to depression have done so by measuring inflammatory markers in the blood. It is more difficult to measure inflammation in the brain of living people, but Meyer has taken advantage of new developments in positron emission tomography (PET) scans to measure translocator protein binding, which illustrates when microglia are activated. Microglial activation is a sign of inflammation. Translocator protein binding was elevated by about 30% in the prefrontal cortex, anterior cingulate cortex, and insula in study participants who showed symptoms of a major depressive episode compared to healthy control participants. The implication is that the depressed people with elevated translocator protein binding have more brain inflammation, probably via microglial activation.
The antibiotic minocycline reduces microglial activation. It would be interesting to see if minocycline might have antidepressant effects in people with depression symptoms and elevated translocator protein binding.
Antibody Sirukumab Improves Depression and Anhedonia in Patients with Rheumatoid Arthritis
Patients with rheumatoid arthritis have high levels of the inflammatory proteins known as interleukin-6 (IL-6), which have been implicated in depression and stress. Rheumatoid arthritis is sometimes characterized by depressive symptoms as well. New research by Dai Wang and colleagues presented at the 2015 meeting of the Society of Biological Psychiatry suggests that treating the high levels of IL-6 in rheumatoid arthritis with the human anti–interleukin-6 antibody sirukumab can reduce symptoms of depression and anhedonia (loss of capacity to experience pleasure).
In the study, patients with rheumatoid arthritis and symptoms of depression or anhedonia were randomized to receive either placebo or sirukumab. After 12 weeks, those who received sirukumab had significantly reduced depression.
Editor’s Note: These data are consistent with meta-analyses showing that IL-6 is elevated in depression and with a study by Scott Russo showing that in animals, interfering with IL-6 blocks the development of depression-like behaviors that typically occur after repeated defeat stress (when an animal is subjected to attacks from a larger, more dominant animal).
Inflammation Predicts Depression Persistence
Links between inflammation and depression continue to be identified in new research. Researcher N. Vogelzangs et al. reported in a 2014 article in Neuropharmacology that inflammatory and metabolic dysregulation in antidepressant users predicted an outcome of depression two years later. Elevated levels of the marker of inflammation Il-6, low HDL (or “good”) cholesterol, high triglycerides, and high blood sugar were associated with poor response to medication and chronicity of depression. Of 315 people treated with antidepressants (average age 43), 138 were in remission at 2 years, while 177 (56.2%) were still depressed. People with four or more types of inflammatory or metabolic dysregulations had a 90% chance of still being depressed at 2 years.
Among inflammatory markers including CRP and TNF-alpha, IL-6 alone was associated with chronic depression. Il-6 can cross the blood-brain barrier. We have previously reported that researcher Scott Russo found that in rats in a depression-like state known as defeat stress (brought about by repeated defeat by a larger rodent), blocking Il-6 can prevent depressive behaviors such as social avoidance or loss of preference for sucrose.
Like inflammation, metabolic abnormalities also complicate depression. Lipid dysregulation and hyperglycemia are associated not only with depression persistence, but also with the new onset of depression in humans.
Vogelzangs et al. conclude that these data “ suggest that inflammatory and metabolic dysregulation worsens depression course owing to reduced [antidepressant] response and that alternative intervention treatments may be needed for depressed persons with inflammatory and metabolic dysregulation.”
It is noteworthy that a 2014 meta-analysis of the anti-inflammatory drug celecoxib (Celebrex) published by Farhad Faridhosseini et al. in Human Psychopharmacology, showed that the drug, often prescribed for arthritis, is effective for unipolar depression when added to patients’ regular treatment.
It remains to be ascertained whether celecoxib’s effects are seen in depression in general, or if they pertain only to the 30% of depressed patients who show inflammation at baseline. Typical markers of inflammation include Il-6, CRP, TNFa, and Il-1.
Statins, prescribed to lower cholesterol, also have anti-inflammatory effects, and are also effective in preventing depression.
Determining treatment approaches for those patients showing signs of inflammation or metabolic irregularities remains a high priority for study. The preliminary data noted here suggest that treating these dysregulations in those with depression may be useful.
Inflammatory and Metabolic Abnormalities Predict Poor Response to Antidepressants
 There is mounting evidence that inflammation and metabolic problems are related to depression. A recent study by Vogelzangs et al. in the journal Neuropsychopharmacology examined 313 patients being treated for depression to see whether levels of inflammatory markers in the blood and metabolic factors such as cholesterol, blood pressure, and waist circumference predicted whether those patients would still (or again) be diagnosable with depression two years later.
There is mounting evidence that inflammation and metabolic problems are related to depression. A recent study by Vogelzangs et al. in the journal Neuropsychopharmacology examined 313 patients being treated for depression to see whether levels of inflammatory markers in the blood and metabolic factors such as cholesterol, blood pressure, and waist circumference predicted whether those patients would still (or again) be diagnosable with depression two years later.
Several factors predicted later depression, including high levels of the inflammatory marker interleukin-6, low HDL (“good”) cholesterol, higher than normal triglycerides, and high blood glucose (hyperglycemia).
People who had four or more types of inflammatory or metabolic abnormalities had almost twice the odds of having chronic depression. Among those study participants who had only recently begun taking antidepressant medication, having four or more of these risk factors made them almost 7 times more likely to be depressed during follow-up.
One explanation for the connection between inflammatory and metabolic dysregulation and depression is that inflammation and metabolic problems worsen and complicate a patient’s depression and reduce the patient’s responsiveness to traditional antidepressants. Alternative ways of treating these patients aimed at their inflammation and metabolism may be necessary.
Depression May Not Be All in Your Head
 Repeated social defeat stress (when an intruder mouse is repeatedly threatened by a larger mouse defending its home territory) is often used as a model to study human depression. Animals repeatedly exposed to social defeat stress start to exhibit depression-like behaviors such as social avoidance and loss of interest in sucrose. Georgia Hodes, a researcher at Mount Sinai School of Medicine, reported at a recent scientific meeting that repeated defeat stress–induced behavior was blocked when IL-6, an inflammatory cytokine released by white blood cells in the blood, was inhibited. The central nervous system did not appear to be involved.
Repeated social defeat stress (when an intruder mouse is repeatedly threatened by a larger mouse defending its home territory) is often used as a model to study human depression. Animals repeatedly exposed to social defeat stress start to exhibit depression-like behaviors such as social avoidance and loss of interest in sucrose. Georgia Hodes, a researcher at Mount Sinai School of Medicine, reported at a recent scientific meeting that repeated defeat stress–induced behavior was blocked when IL-6, an inflammatory cytokine released by white blood cells in the blood, was inhibited. The central nervous system did not appear to be involved.
Interestingly, mice with more white blood cells and more IL-6 release at baseline (prior to the social defeat stress) were more likely to show the defeat-stress depressive behaviors.
Editor’s Note: The higher number and greater reactivity of white blood cells seen in these mice could be a clinical marker of vulnerability to defeat stress, and such findings are worthy of study in human depression. White blood cells are critical to fighting infection and sometimes their overactivity can contribute to inflammation. In meta-analyses, a subgroup of depressed patients consistently show elevated inflammatory markers (including IL-1, IL-6, TNF alpha, and CRP), and it remains to be seen whether these markers of inflammation are generated in the central nervous system or come from white blood cells in the blood, and whether their targeted suppression could be a new route to antidepressant effects (as in the study of defeat stress in mice).
Inflammatory Markers of Bipolar Illness Course
 People with bipolar disorder often show signs of inflammation. These could eventually help clarify diagnosis, illness activity, and treatment response, and predict illness progression. Previous studies have shown increases in c-reactive protein (CRP), interleukin-6 (IL-6), and tumor necrosis factor-alpha (TNF-alpha) in adults with mood disorder. These high levels tend to improve with medications, are related to illness severity, and are also related to manic and mixed states.
People with bipolar disorder often show signs of inflammation. These could eventually help clarify diagnosis, illness activity, and treatment response, and predict illness progression. Previous studies have shown increases in c-reactive protein (CRP), interleukin-6 (IL-6), and tumor necrosis factor-alpha (TNF-alpha) in adults with mood disorder. These high levels tend to improve with medications, are related to illness severity, and are also related to manic and mixed states.
At the 2013 meeting of the American Academy of Child and Adolescent Psychiatry (AACAP), Ben Goldstein reported on a study that examined levels of TNF alpha, IL-6, and high sensitivity CRP (hsCRP) in 123 adolescents with an average age of 20.4 years, who had been ill for an average of 12.7 years.
CRP levels in adolescents with bipolar illness were equivalent to those with rheumatoid arthritis, and much higher than healthy controls. In children with bipolar disorder, higher levels of CRP were related to more time symptomatic. High hsCRP was related to lower socio-economic status and to substance abuse disorders.
Increases in IL-6 were linked to a longer time to achieve remission and more weeks depressed. High IL-6 was related to duration of illness, positive family history of substance use, and family conflict.
High TNF alpha was related to low socioeconomic status (SES), self-injury, suicidal ideation, and positive life events.
Goldstein said studies of these markers could eventually lead to therapeutic advances, but the process would be long and would require several steps: proof of concept studies, prospective validation studies in independent samples, and demonstration of clinical gains over standard predictive markers, culminating in enhanced patient care and outcome through better, faster prediction of response.
Editor’s Note: Ideally clinicians could jump ahead by immediately attempting to determine whether adding a medication with direct anti-inflammatory effects could enhance therapeutic effects in children with elevated inflammatory markers. Treating inflammation could also theoretically help prevent cognitive deterioration and decrease the considerable risk for cardiovascular dysfunction in patients with bipolar disorder.