Abuse Histories Decrease Rate of Remission to Antidepressant Treatment
Harkness et al reported in The Canadian Journal of Psychiatry (2023) “Greater severity of emotional maltreatment perpetrated by the mother was a significant and direct predictor of lower odds of week 16 remission (odds ratio [OR]=1.68, P =0.02). In contrast, the relations of paternal-perpetrated emotional maltreatment and physical maltreatment to week 16 remission were indirect, mediated through greater severity of anhedonia at week 8.”
Editors note: Response to ADs is less good in those with a history of abuse in childhood. Therefore psychotherapy should be added to medications in such situations to attempt to enhance responsiveness.
U.S. FDA Approves VRAYLAR® (cariprazine) as an Adjunctive Treatment for Major Depressive Disorder
“A Phase 3 Study 3111-301-001 showed a clinically and statistically significant change from baseline to week six in the Montgomery-Åsberg Depression Rating Scale (MADRS) total score for patients treated with cariprazine at 1.5 mg/day + ADT compared with placebo + ADT. A second registration-enabling study, RGH-MD-75, showed a clinically and statistically significant change from baseline to week eight in the MADRS total score for patients treated with cariprazine at 2-4.5 mg/day (mean dose 2.6 mg) + ADT compared with placebo + ADT.
Cariprazine was generally well tolerated in 6- and 8-week studies. Mean weight change was < 2lbs and ? 3% of patients had a weight increase of ? 7%.
The starting dosage of VRAYLAR is 1.5 mg once daily. Depending upon clinical response and tolerability, the dosage can be increased to 3 mg once daily on Day 15. In clinical trials, dosage titration at intervals of less than 14 days resulted in a higher incidence of adverse reactions. The maximum recommended dosage is 3 mg once daily.
Most common adverse reactions observed in the adjunctive MDD studies (? 5% and at least twice the rate of placebo) were:
Akathisia, nausea, and insomnia at the recommended doses in 6-week, fixed-dose trials
Akathisia, restlessness, fatigue, constipation, nausea, increased appetite, dizziness, insomnia, and extrapyramidal symptoms in one 8-week flexible-dose trial at a titration of less than 14 days”
First and Only Oral NDMA Receptor Antagonist for MDD Can Now Be Prescribed
| October 28, 2022 |
| FEATURED NEWS: First and Only Oral NDMA Receptor Antagonist for MDD Can Now Be Prescribed Extended-release dextromethorphan HBr-bupropion HCl (Auvelity™), the only oral N-methyl D-aspartate (NMDA) receptor antagonist approved for the treatment of major depressive disorder (MDD), is now available by prescription in the United States, maker Axsome Therapeutics Inc. announced. The drug is supplied in 105-mg tablets in 30-count bottles.On August 18th, 2022, the US Food and Drug Administration (FDA) approved dextromethorphan HBr-bupropion HCl extended-release tablets 45mg/105mg |
Scientific Mechanisms of Rapid-Acting Antidepressants
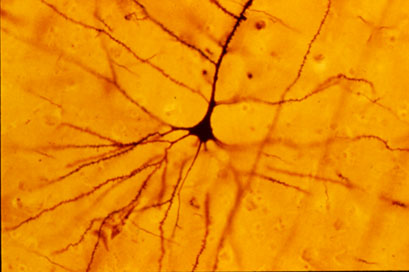
A pyramidal cell (Photo by Bob Jacobs, Laboratory of Quantitative Neuromorphology Department of Psychology Colorado College)
At a recent symposium, researcher Francis McMahon provided electrophysiological evidence that several different types of rapid-acting antidepressants—low-dose ketamine, scopolamine, and rapastinel (a partial agonist of the neurotransmitter NMDA)—act by decreasing the inhibitory effects of GABAergic interneurons on excitatory neurons called pyramidal cells, thus increasing synaptic firing.
Researcher Ronald Duman further dissected these effects, showing that ketamine and its active metabolite norketamine reduce the steady firing rate of GABA interneurons by blocking NMDA receptors, while the partial agonist rapastinel acts on the glutamate neurons directly, and both increase the effects of a type of glutamate receptors known as AMPA. These effects were demonstrated using a virus to selectively knock out GluN2B glutamate receptor subunits in either GABA interneurons or glutamate neurons.
Increasing AMPA activity increases synapse number and function and also increases network connectivity, which can reverse the effects of stress. Duman and colleagues further showed that when light is used to modulate pyramidal cells (a process called optogenetic stimulation) in the medial prefrontal cortex, different effects could be produced. Stimulating medial prefrontal cortex cells that contained dopamine D1 receptors, but not D2 receptors, produced rapid and sustained antidepressant effects. Conversely, inhibiting these neurons blocked the antidepressant effects of ketamine. Stimulating the terminals of these D1-containing neurons in the basolateral nucleus of the amygdala was sufficient to reproduce the antidepressant effects. These data suggest that stimulation of glutamate D1 pyramidal neurons from the medial prefrontal cortex to the basolateral nucleus of the amygdala is both necessary and sufficient to produce the antidepressant effects seen with ketamine treatment.
Researcher Hailan Hu reported that NMDA glutamate receptors drive the burst firing of lateral habenula (LHb) neurons, which make up the depressogenic or “anti-reward center” of the brain and appear to mediate anhedonic behavior (loss of interest or enjoyment) in animal models of depression. Ketamine blocks the burst firing of the LHb neurons, which disinhibits monoamine reward centers, enabling ketamine’s rapid-onset antidepressant effects. This may occur because inhibitory metabotropic glutamate receptors (mGluR-2) are activated, decreasing the release of glutamate.
MGluR-2 may also help explain the antidepressant effects of acetyl-L-carnitine supplements. L-carnitine is an amino acid that is low in the blood of depressed patients. The supplement acetyl-L-carnitine (ACL) activates the DNA promoter for mGluR-2, increasing its production and thus decreasing excess glutamate release. The acetyl group of the ACL binds to the DNA promoter for mGluR-2, thus this process seems to be epigenetic. Epigenetic mechanisms affect the structure of DNA and can be passed on to offspring even though they are not encoded in the DNA’s genetic sequence.
Risk of Suicide in People with Bipolar Disorder: Lowest with Lithium, Highest with Antidepressants
Researcher Markku Lähteenvuo and colleagues reported in the journal JAMA Psychiatry in early 2018 that long-acting injectable antipsychotics and lithium were best at preventing re-hospitalization in 18,018 bipolar patients in Finland who received an average of more than 7 years of follow up. Lähteenvuo and colleagues have now gone on to analyze suicide data from the same cohort of patients with bipolar disorder, and report that those taking lithium had the lowest rate of suicide, while those taking valproate had the next lowest suicide rate. Those patients with bipolar disorder who were treated with antidepressants had the greatest suicide rate. The suicide rate was particularly high for those once-hospitalized patients taking the MAO inhibitor antidepressant meclobemide, which is not approved for use in the US. Increased rates of suicide were also seen with use of sedatives and benzodiazepines.
Editor’s Note: Evidence continues to mount that lithium should be the definitive first line therapy in bipolar disorder for a multitude of reasons (as this editor Robert M. Post reviewed in an open-access article in the journal Neuropsychopharmacology in 2017). Still, lithium is not often prescribed for people with bipolar disorder in the US, and this does not seem to be in these patients’ best interests.
Use of antidepressants in bipolar disorder has remained controversial, but it is common in clinical practice despite a lack of evidence that it is effective, and the presence of some evidence that it is actually harmful. Antidepressant use in a person with bipolar disorder may cause switching into mania, cycle acceleration, dysphoria induction, and even suicide.
Clinicians should take these data seriously and overcome the impulse (leftover from treating unipolar depression) to use unimodal antidepressants as first line or adjunctive therapy for bipolar depression. Antidepressants are only effective in the long term in about 15% of patients with bipolar depression, and now it appears antidepressant use also carries an additional risk of suicide.
Inflammation is Associated with Antidepressant Treatment Resistance
Researcher Ebrahim Haroon and colleagues report in a 2018 issue of Psychoneuroendocrinology that people whose depression failed to respond to at least three different antidepressants in their current episode of depression had higher levels of inflammation than those who had fewer than three failed antidepressant trials.
The researchers found that patients who had not responded to antidepressants had higher levels of the inflammatory markers TNF-alpha, TNF-alpha receptor 2, and Il-6. The inflammatory marker CRP was also significantly elevated in these patients when statistical analyses that excluded body mass index (BMI) were used.
Haroon and colleagues reported that a third of all patients with major depressive disorder fail to respond to currently available antidepressant treatments, and that inflammation may be to blame because it interferes with the neurotransmitter systems that antidepressants target.
Editor’s Note: These data indirectly support the use of anti-inflammatory drugs to augment the effects of antidepressants in patients with treatment resistant depression. A caution that may be very important is to assess evidence of inflammation at baseline, as some data suggest that people with low CRP may, for example, do more poorly with a blocker of TNF-alpha, while people with high CRP at baseline (over 3 pg/ml) show good improvement.
Meta-Analysis Finds Antidepressants More Effective Than Placebo
In a 2018 article in the journal The Lancet, researchers led by Andrea Cipriani compared the efficacy of 21 different antidepressants and established that antidepressants are more effective than placebo at reducing unipolar depression. To date, this is the largest meta-analysis of double-blind, randomized controlled studies of antidepressant efficacy, including 522 trials and a total of 116,477 participants. All 21 of the antidepressants were found to be more effective than placebo.
Looking at head to head studies, Cipriani and colleagues found that the most effective antidepressants were agomelatine, amitriptyline, escitalopram, mirtazapine, paroxetine, venlafaxine, and vortioxetine. The least effective antidepressants were fluoxetine, fluvoxamine, reboxetine, and trazodone.
In terms of tolerability, agomelatine, citalopram, escitalopram, fluoxetine, sertraline, and vortioxetine were most tolerable to patients, while amitriptyline, clomipramine, duloxetine, fluvoxamine, reboxetine, trazodone, and venlafaxine caused the most study dropouts due to side effects. Only agomelatine and fluoxetine had better dropout rates than placebo.
Interestingly, agomelatine, the medication found to be most effective and most tolerable, is unavailable in the US. Pharmaceutical company Novartis, which owns the rights to the drug, was disappointed by some lackluster studies of the drug and never applied for Food and Drug Administration approval to sell it in the US. The studies found potential problems regarding drug interactions related to the metabolic enzyme CYP1A2 and a risk of liver damage with longer-term use.
Editor’s Note: This meta-analysis should end any remaining controversy about the efficacy of antidepressants in the acute treatment of unipolar depression.
This study did not address maintenance treatment for the prevention of depressive episodes. Researcher John R. Geddes and colleagues have found robust, statistically significant data that continuation treatment with antidepressants can prevent depressive relapse, suggesting that if patients continue taking effective antidepressants, rather than switching to placebo, the antidepressants can reduce depressive occurrences by about 70%.
It is now recommended in most guidelines that patients with two or three prior episodes of depression consider staying on antidepressants indefinitely over their lifetime in order to prevent recurrence. Antidepressants increase the creation of new neurons and brain-derived neurotrophic factor (BDNF), which protects neurons and is important for learning and memory. Antidepressants can also prevent loss of hippocampal volume.
Using Antidepressants During Pregnancy Likely Does Not Increase Autism Risk
In the past year or so, several meta-analyses have analyzed data from numerous studies of a possible link between antidepressant use in pregnancy and autism in the offspring. In a 2017 article in the Journal of Clinical Psychiatry, researcher Chittaranjan Andrade offers a meta-analysis of these previous meta-analyses, and determines that while there is a small link between antidepressant use in pregnancy and autism in the offspring, it is most likely the mother’s depressive illness rather than the medications that is responsible for this link.
Andrade found that antidepressant exposure was linked to an increased risk of autism spectrum disorders in the offspring even when the antidepressant use occurred only before conception occurred, when it could not possibly have affected the future fetus’ physiology. This implies that it is the mother’s illness rather than the antidepressant treatment that is a determinant of autism risk.
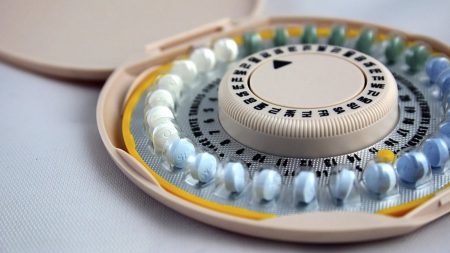
Use of Hormonal Contraceptives May Increase Depression Risk in Young Women
Women, particularly adolescent women, are at increased risk of developing depression if they use hormonal contraceptives, according to a 2016 study in the journal JAMA Psychiatry. The study by Charlotte Wessel Skovlund and colleagues used data from a Danish registry of more than one million women between the ages of 15 and 34 who had no history of depression or other psychiatric disorders. During follow-up (which lasted an average of 6.4 years), 55% of the women were using or had recently used hormonal contraceptives. These women were more likely to be prescribed an antidepressant for the first time, and more likely to be diagnosed with depression compared to women who did not use hormonal contraceptives.
The increased risk of being prescribed an antidepressant varied by contraceptive type. The norgestrolmin patch increased risk by 2.0 times, and the etonogestrel vaginal ring did so by 1.6 times. The levonorgestrel intrauterine device (IUD) made an antidepressant prescription 1.4 times more likely. Progestin-only pills increased risk by 1.34 times and combined oral contraceptive pills increased it by 1.23 times compared to women who did not use oral contraceptives.
The relative risk peaked at around six months after starting hormonal contraceptives.
Patients aged 15–19 were particularly vulnerable to depression. The likelihood of receiving an antidepressant prescription was 1.8 times higher in teens taking combined pills, 2.2 times higher in those taking progestin-only pills, and 3 times higher in teens using hormonal methods of birth control that are not delivered orally compared to those who did not use hormonal contraceptives at all.
Antidepressant Use in Pregnancy Does Not Increase Autism Risk
 Two large observational studies published in the journal JAMA in 2017 find no link between antidepressant use during pregnancy and risk of an autism spectrum disorder. Previous studies had suggested a link between the two, but may not have sufficiently accounted for confounding factors. In both new studies, autism rates did not differ between siblings exposed to antidepressants in utero and those who were not exposed.
Two large observational studies published in the journal JAMA in 2017 find no link between antidepressant use during pregnancy and risk of an autism spectrum disorder. Previous studies had suggested a link between the two, but may not have sufficiently accounted for confounding factors. In both new studies, autism rates did not differ between siblings exposed to antidepressants in utero and those who were not exposed.
One of the studies, by researcher Ayesha C. Sujan and colleagues, analyzed exposure to antidepressants in the first trimester and neurodevelopmental outcomes in almost 1.6 million Swedish children. Antidepressant use did slightly increase the chance of a preterm birth, but was not linked to autism spectrum disorder, attention-deficit hyperactivity disorder (ADHD), or small size of the fetus.
The researchers suggested that doctors and patients work together to decide how depression should be treated during pregnancy, based on severity of the depression, treatment history, and access to services.
The other study, by researcher Hilary K. Brown and colleagues, analyzed 36,000 births in Ontario, Canada and found no increased risk of autism spectrum disorder based on antidepressant exposure in utero. The study controlled for 500 characteristics such as mother’s education, age, and health history.
The journal JAMA Pediatrics also published a meta-analysis and review of 10 studies on the subject, finding that a woman’s history of psychiatric disorders weakened any link between antidepressant use during pregnancy and risk of autism spectrum disorder in her children. This implies that the underlying illness, not its treatment, may be responsible if there is any link between depression and autism. The meta-analysis was carried out by researcher Antonia Mezzacappa and colleagues.