Psychiatric Risks in Offspring of Parents with Bipolar/Unipolar Disorders
 At the 2019 meeting of the International Society for Bipolar Disorders, researcher Martin Preisig and colleagues from Lausanne, Switzerland reported on a longitudinal study of mood disorders in offspring of parents with bipolar disorder, unipolar depression, or no history of psychiatric illness. The study included 446 children (with an average age of 10.1 years at the beginning of the study), who participated for an average of 11.9 years.
At the 2019 meeting of the International Society for Bipolar Disorders, researcher Martin Preisig and colleagues from Lausanne, Switzerland reported on a longitudinal study of mood disorders in offspring of parents with bipolar disorder, unipolar depression, or no history of psychiatric illness. The study included 446 children (with an average age of 10.1 years at the beginning of the study), who participated for an average of 11.9 years.
Preisig and colleagues determined symptoms and other factors that preceded psychiatric illness. They found that bipolar disorder in the offspring was preceded by sub-threshold hypomania, major depression, and conduct disorder. Bipolar disorder in the offspring was also predicted by parental early-onset bipolar disorder.
Major depression was preceded by separation anxiety disorder, and witnessing violence or being a victim of sexual abuse.
Preisig and colleagues concluded that not only did bipolar disorder and major depressive disorder have different familial origins, they also had different antecedents and risk factors.
Inflammation Associated with Cognitive Deficits
At the 2019 meeting of the International Society for Bipolar Disorders, researcher Katherine E. Burdick and colleagues at Brigham and Women’s Hospital and Harvard Medical School reported that in 240 patients with bipolar disorder who were not currently having a manic or depressive episode, markers of inflammation were associated with cognitive deficits.
Inflammation was associated with cognitive deficits in general, and there were also some relationships between specific inflammatory markers and types of cognitive processing. They found that the inflammatory markers TNF-alpha, TNFR1, and TNFR2 influenced cognitive flexibility. The inflammatory marker VEGF influenced reward processing, while IL-6/IL-6r influenced spatial processing. IL-1beta and IL-1RA influenced social cognition.
Burdick and colleagues found it was important to include both primary and secondary mediators of inflammation in their research “as the effects of the primary pro-inflammatory cytokines can be blocked by a number of decoy receptors and soluble antagonists.” Elevations in these can provide additional information about the function of the immune system.
Editor’s Note: Targeting inflammation with the anti-inflammatory treatments minocycline and celecoxib has been shown to improve depression. Now the role of anti-inflammatory drugs in improving cognition deserves further attention.
Mounting Evidence of Mitochondrial Dysfunction in Bipolar Disorder
At the 2019 meeting of the International Society for Bipolar Disorders, researchers Ana Andreazza, Olivia Dean and colleagues reviewed substantial data that implicate mitochondrial dysfunction in the mood and energy fluctuations that make up bipolar disorder. Most of the neurobiological alterations known to occur in bipolar disorder have a relationship to mitochondria, which produce energy within cells. These alterations include abnormalities in glutamate, gene expression, apoptosis (cell death), oxidative stress, low ATP (a molecule that stores energy), altered ion pumps, increased intracellular calcium, and insufficient glutathionine (an antioxidant made up of three amino acids).
Coenzyme Q10 is a mitochrondrial enhancer of Complex I, an enzyme that is key to the first step in mitochondrial energy production. A 2018 controlled study by Maryam Mehrpooya and colleagues published in the Journal of Clinical Psychopharmacology found that 200mg/day of CoQ10 was more effective than placebo at reducing symptoms of bipolar depression when added to patients’ stable treatment regimens that included mood stabilizers and antidepressants. The effect size was large (0.87), and it took eight weeks for the benefit over placebo to appear. Response rate to CoQ10 was 72% compared to 12% to placebo.
Editor’s Note: Some formulations of CoQ10 do not cross the blood-brain barrier easily, so only a very small percentage of the CoQ10 gets into the brain. Thus, consumers should be careful about the type of product they purchase. The one made by Takeda Pharmaceutical Company is likely to be effective.
Early Predictors of Suicide and Lithium as an Anti-Suicide Drug
 At the 2019 meeting of the International Society for Bipolar Disorders, researcher Gin S. Malhi discussed early predictors of suicide in people with bipolar disorder, such as younger age of illness onset, early life stressors, and family history of suicide. Impulsivity, hopelessness, cognitive deficits and substance use are risk factors, both for suicide in general and for an imminent suicide attempt. Proximal risk factors that indicate someone may make a suicide attempt soon include: mood swings, rapid cycling, increased depression, hospitalization, and severe anxiety.
At the 2019 meeting of the International Society for Bipolar Disorders, researcher Gin S. Malhi discussed early predictors of suicide in people with bipolar disorder, such as younger age of illness onset, early life stressors, and family history of suicide. Impulsivity, hopelessness, cognitive deficits and substance use are risk factors, both for suicide in general and for an imminent suicide attempt. Proximal risk factors that indicate someone may make a suicide attempt soon include: mood swings, rapid cycling, increased depression, hospitalization, and severe anxiety.
Editor’s Note: Among all psychotropic drugs, lithium has the best data supporting its anti-suicide effects, both at therapeutic doses in patients with bipolar disorder and at trace levels in the water supply in the general population. People who live in locations where more lithium is naturally present in the water supply have lower rates of suicide than those who live in places with less lithium in the water. Malhi also noted that the antioxidant N-acetylcysteine (NAC), which has positive effects on mood and habitual behaviors, can reduce the incidence of lithium-induced dysfunction of the kidneys.
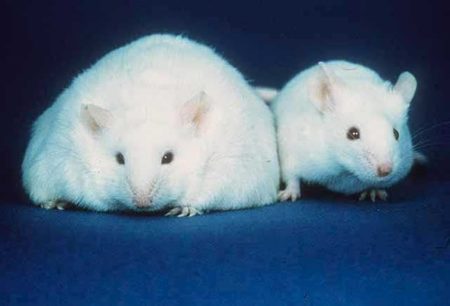
Obesity Associated with Inflammation and Brain Abnormalities
At the 2019 meeting of the International Society for Bipolar Disorders, researcher David J. Bond reviewed the data on the multiple adverse effects of obesity in patients with bipolar disorder. These include increased cardiovascular risk, poorer response to treatment, brain abnormalities, and decreased cognitive function, which is correlated with the degree of overweight.
Editor’s Note: These data emphasize the importance of starting a nutritious diet early in life and sustaining it through adulthood, avoiding the drugs most associated with weight gain such as clozapine and olanzapine, and facilitating weight loss with drugs. There are several treatments that can aid in weight loss. One is the diabetes treatment metformin, starting at a high dose of 500mg twice daily, and increasing to 1000mg twice daily if tolerated. The anticonvulsants topiramate or zonisamide also promote weight loss. The most effective option is a combination of the antidepressant bupropion sustained release (at a dose of 150–300mg) plus the anti–substance abuse drug naltrexone (50mg). This combination was associated with a loss of 10% of body weight over 12 weeks in women with diabetes.
Red Meat Interacts with Bacteria in the Gut to Raise Heart Disease Risk
 A 2018 study by a group of researchers at the Cleveland Clinic have clarified the way that a diet heavy in red meat may lead to heart disease. The research centers on trimethylamine N-oxide (TMAO), a gut bacteria byproduct that is formed during digestion. When gut bacteria digest choline, lecithin, and carnitine, nutrients that are common in certain animal products and red meat, TMAO is produced.
A 2018 study by a group of researchers at the Cleveland Clinic have clarified the way that a diet heavy in red meat may lead to heart disease. The research centers on trimethylamine N-oxide (TMAO), a gut bacteria byproduct that is formed during digestion. When gut bacteria digest choline, lecithin, and carnitine, nutrients that are common in certain animal products and red meat, TMAO is produced.
In an article by Robert A. Koeth and colleagues in the European Heart Journal, the researchers show that diets that rely on red meat as the main protein source lead to more circulating TMAO than diets in which white meat or something other than meat is the primary source of protein. They found that in people who eat a lot of red meat, the kidneys are less efficient at expelling TMAO, and levels creep even higher. High levels of TMAO have been linked to hardening and narrowing of the arteries (atherosclerosis) and heart disease complications. High levels of TMAO in the blood can be a predictor of heart attack, stroke, and death.
The study of 113 participants consisted of three different diets that each participant followed in random order (with a washout period in between each diet). A month of eating a diet in which red meat was responsible for at least 25% of participants’ daily calories led to higher levels of TMAO in the blood and urine. TMAO increased threefold during the red meat diet periods compared to periods in which white meat or non-meat protein were the source of those calories, and in certain participants, TMAO increased as much as tenfold. When participants stopped eating the red meat diet, their TMAO levels fell over the following month.
Rich Western Diet Reprograms Immune Cells in Mice
A 2018 article by Anette Christ and colleagues in the journal Cell describes the process by which a Western diet can trigger changes to the immune system in mice. The mice fed a calorically rich Western diet started to show systemic inflammation. Blood measures of inflammation returned to normal after the mice resumed their regular diet, but their immune responses remained heightened, as if the immune system had been trained to overreact.
The vast majority of deaths in Western cultures are caused by noncommunicable diseases such as type 2 diabetes and cardiovascular disease, which have been linked to lifestyle factors such as diet and exercise. The immune system has two wings: one that responds to specific pathogens, and one that mounts general protection against infection and is triggered by immune signaling receptors. However, according to Christ and colleagues, in addition to reacting when microbes are present, this second wing may also respond to “sterile” danger signs, such as consumption of a Western diet. The immune system may become trained to react this way chronically, something that the researchers believe may trigger inflammation in noncommunicable diseases.
The Western diet triggered epigenetic changes to the mice’s immune system. Epigenetic changes are ones that affect the structure of DNA, for example how tightly it is packaged. In the case of the Western diet, these changes resulted in a heightened immune system that launched strong inflammatory responses in reaction to even small stimuli. Myeloid cells from bone marrow were reprogrammed to proliferate and provide a stronger immune response.
The researchers also took human monocyte cells trained with LDL (“bad”) cholesterol and stimulated them with lipopolysaccharide (an inflammatory compound made of fat and sugar). The cells showed a heightened immune reaction similar to that seen in the mice.
Mice genetically engineered to lack the inflammasome NLRP3, which activates inflammatory responses, did not show the systemic inflammation or the enhanced myeloid activity when fed the Western diet, so Christ and colleagues believe NLRP3 may play an important role in mediating the immune response to the Western diet.
Eating Walnuts and Other Tree Nuts May Lower Cholesterol
In a 2018 meta-analysis and systematic review published in the American Journal of Clinical Nutrition, researcher Marta Guasch-Ferré and colleagues shared their analysis of 26 studies of the effects of diets rich in walnuts on blood lipids and cardiovascular health. The studies included a total of 1059 participants. The walnut-heavy diets were associated with lower total cholesterol, lower LDL (“bad”) cholesterol, and lower triglyceride concentrations. They were also associated with lower apolipoprotein B, a component of LDL.
When walnut-enriched diets were compared to American diets and Western diets, the benefits of the added walnuts on total cholesterol and LDL cholesterol were even more dramatic. The researchers described a Western diet as high in red and processed meats, high-fat dairy products, processed and artificially sweetened foods, and with little intake of fruits, vegetables, fish, legumes, or whole grains.
Compared to control diets, the diets rich in walnuts did not cause weight gain or an increase in body mass index (BMI), and they also did not affect blood pressure.
The studies included in the meta-analysis lasted from four weeks to one year, with a mean length of 8 weeks. The amount of walnuts ranged from 15 to 108 grams per day. In most cases, participants were given whole walnuts to incorporate into whatever daily meal plan they were following, which in some cases was their usual diet and in others was an intervention diet such as a Mediterranean diet or a low-fat diet.
Another meta-analysis published in the American Journal of Clinical Nutrition in 2015 by Liana C. Del Gobbo and colleagues analyzed 61 studies about the effects of tree nuts on cholesterol and related measures, and similarly found that eating tree nuts lowers total cholesterol, LDL cholesterol, ApoB, and triglycerides. Del Gobbo and colleagues wrote, “The major determinant of cholesterol lowering appears to be nut dose rather than nut type.” Tree nuts include walnuts, pistachios, macadamia nuts, pecans, cashews, almonds, hazelnuts, and Brazil nuts.
Vitamin D Deficiency in Newborns Linked to Higher Risk of Schizophrenia in Adulthood
 A 2018 study by Darryl W. Eyles in the journal Scientific Reports found that newborns with vitamin D deficiency were more likely to develop schizophrenia later in life. The study made use of several Danish data depositories and had a large sample size of 2,602 participants. In this case control study, registries of patients treated for schizophrenia were matched up to preserved dried blood samples collected at their births, and these were compared to other dried blood samples from people without schizophrenia who shared the same sex and birthdate.
A 2018 study by Darryl W. Eyles in the journal Scientific Reports found that newborns with vitamin D deficiency were more likely to develop schizophrenia later in life. The study made use of several Danish data depositories and had a large sample size of 2,602 participants. In this case control study, registries of patients treated for schizophrenia were matched up to preserved dried blood samples collected at their births, and these were compared to other dried blood samples from people without schizophrenia who shared the same sex and birthdate.
The researchers divided participants into quintiles based on vitamin D levels at birth. Compared to those who fell into the fourth quintile, those in the lowest quintile were 44% more likely to be diagnosed with schizophrenia in adulthood. The researchers also determined polygenic risk scores for each participant, that is, they calculated schizophrenia risk based on the presence of various genes. The two processes together explained 1.2% of the variance in schizophrenia diagnoses.
Risk factors for vitamin D deficiency include being born in the winter or spring, living in high-latitude locations, spending early life in an urban setting, and being darker-skinned (especially in high-latitude locations). These risk factors are all correlated with decreased skin absorption of UV rays from the sun, which is how the human body produces vitamin D. The vitamin D receptor is expressed in the brain in areas that are relevant to schizophrenia, such as areas with a lot of dopamine activity, and each of the above risk factors also applies to schizophrenia.
As expected, participants born in the winter and spring had lower vitamin D levels. Participants whose parents had immigrated to Denmark had lower vitamin D than those with parents native to Denmark.
Newborns’ vitamin D levels depend completely on their mothers’ vitamin D levels, so Eyles and colleagues suggest that ensuring pregnant women have adequate vitamin D levels could prevent some cases of schizophrenia.
Adolescents with Bipolar Disorder May Have Higher Levels of Vitamin D–Binding Protein

Vitamin D binding protein. Illustration: Emw [CC BY-SA 3.0 (https://creativecommons.org/licenses/by-sa/3.0)]
A 2018 article by Brawnie Petrov and colleagues in the journal Translational Psychiatry suggests that adolescents with bipolar disorder have higher levels of vitamin D–binding protein than adolescents without a mood disorder. The researchers wrote that vitamin D–binding protein “responds early to cellular damage by binding…structural proteins and activating inflammatory cells.”
This pilot study suggests that measuring levels of vitamin D–binding protein could be a useful marker of bipolar disorder. The study was small, with only 12 participants who had bipolar disorder, 11 who had unipolar depression, and 13 with no mood disorder. The researchers hope to follow up with larger studies in adolescents and adults using blood that has already been collected from people with bipolar disorder.
Vitamin D–binding protein is not measured by a standard blood test. The study authors used a technique where they “fished” for inflammatory factors that might be linked to mood disorders. The researchers began by looking for a link between other inflammatory markers in the blood and bipolar disorder, which have repeatedly been found in other studies, but they did not find any such association. There also did not seem to be a link between bipolar illness and vitamin D levels in the blood, only vitamin D–binding protein levels.
It can be especially difficult to distinguish early bipolar disorder from unipolar depression, and if the results of this small study are replicated, a blood test might eventually help to identify people with bipolar disorder earlier.